Brain Tumour Guide

About seventy percent of brain tumors are benign.
The 5-year survival rate for benign brain tumor patients is approximately 95%.
30% of all primary brain tumors are meningiomas; the most prevalent are benign.
The incidence of benign brain tumors increases with age; the highest is in older than 60 years.
 A little about the brain cells
A little about the brain cells
The brain is the most intricate organ in the body. It communicates electrically and chemically with every area of the body. Most of our actions, including speaking, moving, thinking, learning, and feeling, are controlled, coordinated, and regulated by the brain. It is the “command post” of the nervous system.
The typical adult brain weighs roughly 3 pounds and has a 60% fat content. Water, protein, carbohydrates, and salts make up 40% of the body. Along with neurons and glial cells, the brain also has blood vessels and nerves.
The brain contains more than 80 billion billion nerve cells. Among them are:
The neurons are in charge of carrying information throughout the body and between brain cells. They can connect with other neurons and cells thanks to their long, branching structures called axons and dendrites.
- Glial cells: These cells support and feed the neurons in the brain. Glial cells come in various forms. There are microglia, oligodendrocytes, and astrocytes. Oligodendrocytes create the myelin sheath that surrounds and insulates axons; astrocytes support regulating the chemical environment around neurons and supply them with nutrients. Microglia assist in clearing out damaged or dead cells as part of the immune response in the brain.
- Ependymal cells: These cells line the central canal of the spinal cord and the ventricles (cavities) in the brain. Cerebrospinal fluid (CSF), which helps to smooth and shield the brain and spinal cord, is produced and circulated by them.
- Pituitary cells: The pituitary gland, which is found at the base of the brain, is composed of various cell types that create hormones that control diverse bodily activities. These hormones are released into the body's bloodstream, where they find their way to specific organs.
- Pineal cells: The hormone melatonin, which aids in regulating sleep and wakefulness, is produced by the pineal gland, a brain structure.
 What is a tumor in the brain?
What is a tumor in the brain?
When cells in the brain divide out of control, they form a mass. It is called a brain tumor. The brain tumor grows slowly, which is one thing that makes it different from cancer. Benign brain tumors tend to stay in one spot and don't grow. So, if the doctor removes the whole brain tumor during surgery, it usually doesn't return.
 Different kinds of benign tumors can happen in the brain; the most common ones depend on where and what type of tissue they affect. Here are some common benign brain tumors:
Different kinds of benign tumors can happen in the brain; the most common ones depend on where and what type of tissue they affect. Here are some common benign brain tumors:
- Meningiomas are tumors in the membranes covering and protecting the brain. They are the most common kind of brain tumor in adults and are mostly harmless.
- Pituitary adenomas are tumors that grow in the pituitary gland, which is at the base of the brain and makes hormones that control many of the body's functions. Most adenomas in the pituitary gland are not dangerous, but some can be cancerous.
- Acoustic neuromas, or vestibular schwannomas, are located on the nerve that goes from the ear to the brain. These tumors can make it hard to hear and keep the balance. Some of them can require surgery to treat brain tumors.
- Craniopharyngiomas: These tumors grow near the pituitary gland, making hormone production and growth hard to control. They are usually harmless, but they can be hard to eliminate.
- Astrocytomas: Astrocytes, which are cells that help nerve cells in the brain, grow into these tumors. Their appearance under microscopy can be low-grade (benign) or high-grade (cancerous).
- Gliomas are a type of brain tumor that arises from glial cells, which provide support and protection for the neurons in the brain. Gliomas can be benign or cancerous (malignant) depending on the specific type of glial cell from which they develop and their appearance under the microscope.
- Hemangiomas in the brain are typically made up of abnormal blood vessels that are thicker and more fragile than normal ones. They can cause problems if they grow in a location that puts pressure on surrounding brain tissue or disrupts the normal flow of blood.
Even benign tumors can be hazardous. They can damage and compress portions of the brain, resulting in severe damage. Brain tumors that develop in a crucial brain region can be fatal. Very rarely, benign tumors might transform into malignant ones.
 Risk factors and prevention
Risk factors and prevention
A risk factor includes anything that makes it more likely that a person will get a brain tumor. Even though risk factors often play a role in a brain tumor's growth, most do not directly cause one. Some people who have many risk factors never get a brain tumor, while others who have none do. But as of now, we don't know of any way to avoid getting a brain tumor by changing how you live.
Most of the time, no one knows what causes a brain tumor. However, the following things can make a person more likely to get one:
- Age. Brain tumors happen more often in children and older adults, but they can happen to people of any age.
- Gender. Overall, men are more likely to get a brain tumor than women. But women are more likely to get some kinds of brain tumors, like meningiomas.
- Toxic substances, both at home and work. The chance of getting a brain tumor may increase if you are exposed to some chemicals. But there isn't any scientific proof to back up this possible link.
- Family history. Hereditary genetic factors or conditions may cause about 5% of brain tumors.
- Infection, virus, and allergen exposure. Some viruses, like Epstein-Barr virus (EBV) and cytomegalovirus (CMV), are connected with certain types of tumors. Several other types of viruses can also cause brain tumors. Studies have shown that people who have had allergies in the past are less likely to get glioma.
- Race and background. Also, the chance of getting a brain tumor in northern Europe is nearly twice as high as in Japan.
- Ionizing radiation. Ionizing radiation, like x-rays, used to treat the brain or head in the past has increased the risk of a brain tumor.
- A trauma on the head linked with brain tumors. Some studies have found a connection between head trauma and tumor. A history of seizures has also been linked to brain tumors.
How to prevent brain tumors?
At the moment, no one knows how to stop benign brain tumors. Most benign brain tumors are hard to explain, and there are no known ways to stop them. Some things can make someone more likely to get a brain tumor. But just because they have one or more risk factors doesn't mean they will get a brain tumor.
If you are worried, you must talk to a healthcare provider. They can tell you more about the things that might put you at risk and suggest ways to lower that risk. It's also essential to follow the guidelines for cancer screening and tell a doctor immediately if you have any strange symptoms.
 What are the signs and symptoms?
What are the signs and symptoms?
Headaches that worsen when you move or wake up.
Seizures. People have numerous sorts of seizures. Medications can stop or control them. Motor seizures are involuntary muscle movements. Here's how different seizure types look:
- Myoclonic,
- Muscle spasms, twitches, or jerks,
- Grand Mal (Grand Mal).
Consciousness loss and twitching, then relaxing muscles. Loss of body function control, such as bladder control, can occur. The skin may turn blue, purple, gray, white, or green if a person doesn't breathe for 30 seconds. After a grand mal seizure, a person may feel weary, bewildered, weak, numb, or have painful muscles. It may cause repetitive motions resembling twitching.
Other common symptoms may include the following:
- Personality and memory changes
- Vomiting
- Fatigue
- Drowsiness
- Insomnia
- Problems remembering
- Changing walking or daily tasks
The specific signs of brain tumors also can occur:
- A cerebellar tumor can cause balance and delicate motor skill problems.
- A frontal lobe tumor can induce loss of initiative, sluggishness, muscle weakness, or paralysis.
- Occipital or temporal lobe tumors can cause visual loss.
- A frontal or temporal lobe tumor can affect speech, hearing, memory, and mood, causing aggression or problems understanding or recalling words.
- A frontal or parietal lobe tumor can modify how you perceive touch or pressure, weaken one arm or leg, or confuse your left and right sides.
- Pineal gland tumors can prevent looking up.
- Pituitary tumors induce lactation and menstrual cycle abnormalities. Adult hands and feet can grow.
- A brain stem tumor can cause problems with swallowing, facial paralysis, and double vision.
- A temporal, occipital, or brain stem tumor can cause vision loss or double vision.
How a benign brain lump makes a patient feel depends on size and location. Some tumors that grow slowly might not show any signs at first.
 Diagnostic tests
Diagnostic tests
Most neoplasms are diagnosed after symptoms show up. A general practitioner or neurologist does this. The doctor may order more tests to find how fast the neoplasm is growing and if it has spread to other body parts.
Several diagnostic tests may be used to detect benign brain tumors:
- Magnetic resonance imaging (MRI): An MRI uses a magnetic field and radio waves to make detailed brain images. It is often the best test for diagnosing brain tumors.
- MRS scanning, also called magnetic resonance spectroscopy, is a type of MRI that is more specialized. It is helpful to learn about how chemicals in the brain change.
- Computed tomography (CT) scan: A CT scan uses X-rays to create detailed brain images. An MRI is more precise than a CT, but it is faster and may be used if an MRI is not possible.
- Positron emission tomography (PET) scan: A small portion of a radioactive element is used in a PET scan. It is called a tracer and helps to show how the brain functions. It can help guide the difference between benign and cancerous tumors.
- The SPET or SPECT scan shows how the brain's blood flows. On the scan, spots with more blood flow, like tumors, will look brighter.
- Biopsy: A biopsy involves removing a small tissue sample from the tumor and examining it under a microscope. A biopsy is usually done to confirm the diagnosis and determine the type of brain tumor. In other situations, a surgical biopsy is done when surgery on a real brain tumor is done.
- Other tests, such as blood tests, can check the body's overall health and determine hormone levels; an electroencephalogram (EEG) may be used to help diagnose a brain tumor.
It's important to note that these tests can help determine if a brain tumor is present. Still, they cannot always distinguish between benign and cancerous tumors. A biopsy is usually needed to determine the type of brain tumor.
Where can tumors in the brain be treated the best?
 How is a brain tumor treated?
How is a brain tumor treated?
The treatment's goal could be eliminating the tumor, slowing its development, or helping relieve symptoms by making it smaller. Surgery is often the only treatment that can help.
Neurosurgery can be used to remove the whole tumor or just part of it. It is called "total resection" or "partial removal." A partial resection may be the best option when the tumor is close to large blood vessels or an essential part of the brain. Even the slightest damage can make someone blind or paralyzed.
The following types of neurosurgical procedures are used as brain tumor treatments:
- A craniotomy is the most common type of surgery. It is used to remove a brain tumor. Under general anesthesia, all or part of the lump is taken out. The surgeon cuts out a piece of the patient's skull to get to the brain. The growth is cut out, and the bone is put back where it belongs. At the moment, this job is done with the help of a computer navigation system.
- Endoscopic transsphenoidal surgery can remove brain tumors and other abnormalities. It's a minimally invasive procedure done through the nose with an endoscope, light, and camera. The endoscope is inserted through tiny cuts in the nose. An endoscope camera allows the surgeon to view the inside nose and sinus. Using endoscopic equipment, the surgeon eliminates the tumor. Endoscopic transsphenoidal surgery is less painful and scarier than open brain surgery.
- The tubular retractor system is a new, less invasive way of brain surgery. A retractor is a tool that moves or holds tissue so the surgeon can get to a particular area. The tubular retractor is helpful because it forces the seams and gentle tissues of the brain without injuring them as much as other surgical instruments do. It doesn't cut the tissue; instead, it moves it.
So, to the question “ Can brain tumors be cured?” we answer yes. And the following options give more opportunities than ever.
What clinics do we advise?
 New treatment approaches for brain tumors
New treatment approaches for brain tumors
Doctors can treat some types of benign brain tumors without surgery. Possible treatments include taking medicine, getting radiation therapy, or using focused ultrasound. The treatment choice will affect the tumor type, location, and the patient's overall health and medical history. In some cases, oncologists might use all of these treatments together.
If it is impossible to remove the entire tumor, further treatment will be required. In addition, sometimes, the surgeon cannot operate because the neoplasm is located in a place inaccessible to the surgeon or is close to vital structures. Such neoplasms are inoperable, so the brain tumor cure in these cases requires new or alternative methods.
Radiosurgery, also called CyberKnife or GammaKnife, is a high-tech way to deliver a high radiation dose to a lump in the brain. It is a painless, non-invasive procedure called "radiosurgery" because of how precise it is. Stereotactic radiosurgery is another name for this method. A narrow beam of radiation is sent from a device to the lump by a robotic arm that keeps moving around the patient's body. Brain scans before and during the process help the robotic arm track and adjust for small movements. A precise map of where the tumor is in the amount of radiation that gets to healthy tissue near the tumor.
Endovascular embolization is a procedure used to stop blood flow to vascular tumors. Most of the time, a brain neoplasm is fed by large blood vessels. During the process, a thin tube ( catheter) is put into an artery in the leg. With the help of X-rays, the catheter is then guided through the artery to the brain. The catheter is placed into one of the brain lump's blood vessels. The next step is to inject a substance that blocks the blood vessel, such as a jelly-like substance or small particles.
Focused ultrasound suits those looking for brain tumor treatment without surgery. It is a non-invasive therapy. It promises to improve the quality of life for people with brain tumors and lower the cost of their care. With this new technology, beams of ultrasonic energy can hit targets deep in the brain without hurting the normal tissue around them.
Focused ultrasound can be used alone or as part of other treatments. It is non-invasive, so it doesn't come with additional risks like infection or slow wound healing after surgery. It can reach the target without hurting the tissue around it. Focused ultrasound does not use ionizing radiation and can be repeated. The clinical trials continued.
Symptom-treating medicine
Patients may also be given medicine before or after surgery to help with some of the symptoms, such as:
- Anticonvulsants to prevent epileptic fits (seizures).
- Steroids reduce swelling around the tumor, which can help ease some symptoms and make surgery easier.
- Painkillers to treat headaches.
- Anti-emetics to prevent nausea.
Doctors practicing new treatment for brain tumors
 Statistics and prognosis
Statistics and prognosis
Most of the time, benign brain tumors are less dangerous and have a better outlook than malignant ones. But the outlook and treatment options will depend on some factors. There are the tumor type and location and the patient's health.
The American Brain Tumor Association says that about 30 percent of all brain tumors are harmless. Meningiomas and acoustic neuromas are the most common types of benign brain tumors. Despite a slight improvement recently, the five-year survival rate for brain tumors in case they are malignant is only 36%. At the same time, according to NCBI, the 5-year treatment prognosis for benign brain tumors reaches 96.1%.
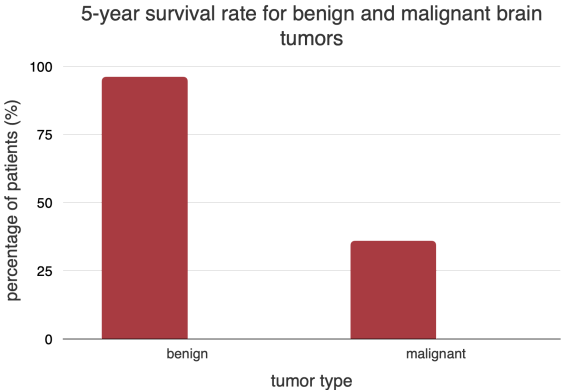
Patients with benign brain tumors have a high chance of living five years after treatment, and many get better. But therapy can be complex sometimes, and some benign tumors can grow back after they are taken out. It's essential to find a company that can help on time and works with a healthcare team to figure out the best treatment plan and keep an eye on the tumor to see if it changes in any way.
References:
- BMJ: Brain tumours: incidence, survival, and aetiology
- National Brain Tumor Society: Quick Brain Tumor Facts
- American Brain Tumor Association: Emotional impact of a brain tumour
- NHS: Treatment - Benign brain tumour (non-cancerous)
- Cancer.Net: Brain Tumor: Types of Treatment
- Cancer Council: Treatment for brain tumors

















