Acoustic Neuroma (Vestibular Schwannoma) Guide

About 6–10% of all brain tumors are caused by an acoustic neuroma, or 1-20 cases to 1 million per year.
In about 90% of cases, the first from acoustic neuroma symptoms is hearing loss in just one ear.
More than 90% of the time, surgery for an acoustic neuroma stops the growth of the tumor.
The five-year survival rate for people with AN is around 95-97%.
 Some info about vestibular nerve
Some info about vestibular nerve
The eighth cranial nerve is the vestibular nerve. It consists of about 20,000 nerve fibers. The vestibular nerve's job is to notice how the head's position changes. The vestibular nerve has two main branches called the superior and inferior vestibular nerves. These nerves carry information about how the head moves in different directions.
The vestibular nerve is connected to the inner ear's semicircular canals and otolith organs, which sense rotational and linear acceleration changes. That information is sent to the brainstem, cerebellum, and cerebral cortex. These parts of the brain are involved in processing and integrating the information from the inner ear.
When the vestibular nerve gets hurt, it can lead to dizziness, vertigo, and trouble keeping your balance.
 What is acoustic neuroma?
What is acoustic neuroma?
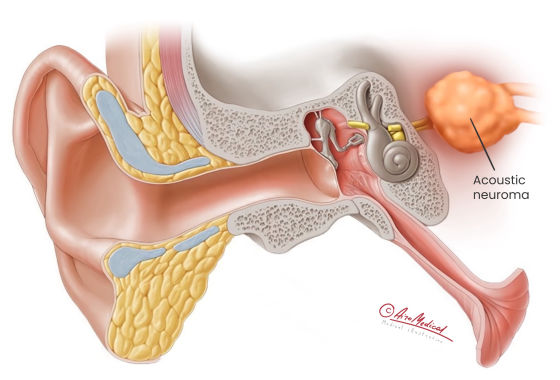 Acoustic neuroma, also called vestibular schwannoma, is a rare type of brain tumor.
Acoustic neuroma, also called vestibular schwannoma, is a rare type of brain tumor.
Tumors grow from cells called Schwann cells. Most of the time, they form in an area called the cerebellopontine angle near the base of the brain. Most of the time (95%), it is a harmless (not cancerous) growth. The tumor grows slowly and rarely spreads to other parts of the body.
Acoustic neuromas happen in 1 to 20 out of every 1 000 000 people worldwide yearly. Vestibular schwannoma tumor in the brain is the neoplasm that occurs more often in middle-aged men.
 What causes and risk factors of acoustic neuromas?
What causes and risk factors of acoustic neuromas?
No one knows what causes acoustic neuromas, but some things put people at risk.
Among the possible causes are
- Some genetic disorders, like neurofibromatosis type 2, make it more likely that the person will get an acoustic neuroma.
- Radiation: High radiation levels, like those used to treat cancer, can raise the risk of getting acoustic neuromas.
- Age: Adults between 30 and 60 will most likely get acoustic neuromas.
- Sex: Women are more likely to get acoustic neuromas than men.
- Family history: If someone in your family has had an acoustic neuroma, you may be more likely to get one yourself.
- Environmental factors: Some studies have shown that some workplaces expose people to toxins, such as chemicals, in the environment.
Most of the time, the causes of acoustic neuromas are unknown, and these tumors can happen to people with no significant risk factors.
How to prevent it?
Since no one knows what causes these tumors, it is hard to suggest specific ways to stop them.
But there is something you can do in general that may help lower your risk of getting a tumor:
- Avoid getting too much radiation, and limit your exposure to radiation sources, like unnecessary medical imaging tests.
- Keep your ears safe: To avoid hearing loss, a risk factor for acoustic neuromas, you should avoid loud noises or wear earplugs in noisy places.
- Maintain a healthy lifestyle. A healthy diet, regular exercise, and not smoking or drinking too much alcohol can help lower the risk of getting tumors.
- Regular checkups help find problems like tumors before they worsen.
These steps can help lower the risk of getting a tumor. Still, they do not guarantee that acoustic neuromas won't happen.
 Symptoms of acoustic neuroma
Symptoms of acoustic neuroma
There may be no unmistakable signs of a small tumor. Because acoustic neuroma increases slightly, the symptoms typically develop over a long period.
Signs experienced by patients with acoustic neuromas
- Unilateral hearing loss was the most frequently reported symptom, with 80% of patients experiencing it. In 90% of these cases, the hearing loss was progressive.
- Unilateral tinnitus was the second most common symptom, affecting 6.3% of patients.
- Other less common symptoms included ataxia (loss of control over body movements), vertigo (dizziness), and headache, accounting for 3.8%, 3.4%, and 2% of cases, respectively.
About 90% of the time, hearing problems in just one ear are the first sign of an acoustic neuroma. As the acoustic neuroma tumor grows, it can cause various symptoms, such as hearing loss and balance problems. It can lead to facial weakness, numbness, and difficulty swallowing if it becomes larger. In some cases, it can even cause severe neurological deficits like paralysis and coma.
 Diagnostic tests for acoustic neuroma
Diagnostic tests for acoustic neuroma
Several diagnostic tests can be used to detect acoustic neuromas, including:
- Audiometry: A hearing test that can detect changes in hearing, such as those associated with acoustic neuromas.
- Magnetic Resonance Imaging (MRI): An imaging test that uses powerful magnets and radio waves to produce detailed images of the brain and the acoustic nerves.
- The computed tomography (CT) scan is an X-ray study that produces detailed brain images. It can detect even small tumors, including acoustic neuromas.
- Electrophysiological tests: These tests measure the electrical activity of the brain and auditory nerves in response to sound and can help identify the location and extent of the tumor.
- Balance tests: These tests evaluate balance and coordination, which may be affected by an acoustic neuroma.
- Otoacoustic Emissions (OAE) test: This test can detect changes in the inner ear caused by an acoustic neuroma.
- Auditory Brainstem Response (ABR) test: This test measures the electrical activity of the auditory nerve and brainstem in response to sound and can help detect abnormalities caused by an acoustic neuroma.
Depending on the tumor's suspected size and location, the doctor may recommend some or all of these tests to diagnose and evaluate the acoustic neuroma accurately.
Stages of acoustic neuromas
- Stage 1: This is the early stage of the tumor, where it is small and confined to the internal auditory canal. Symptoms are usually mild or absent.
- Stage 2: The tumor has grown beyond the internal auditory canal and into the cerebellopontine angle. Symptoms may include hearing loss, tinnitus, and balance problems.
- Stage 3 is characterized by further tumor growth into the brainstem or adjacent structures. Symptoms may become more severe, including facial weakness, numbness, and difficulty swallowing.
- Stage 4: In this final stage, the tumor has reached a large size and may compress vital structures in the brain, such as the brainstem. Symptoms may include severe neurological deficits, such as paralysis, coma, and death.
Not all acoustic neuromas progress through these stages; some may remain small and asymptomatic for many years. The vestibular schwannoma treatments and management will depend on the tumor's size, location, growth pattern, and the individual patient's health status and preferences.
Where to go to treat acoustic neuroma?
 Treatment options for acoustic neuroma
Treatment options for acoustic neuroma
Treatment options depend on several factors, including the size and location of the tumor, the patient's age and overall health, and the severity of symptoms.
Standard treatment options for acoustic neuromas treatment
- Observation: The doctor may recommend regular monitoring if the tumor is small and not causing any symptoms. It is recommended in some cases, particularly for elderly or frail patients, instead of surgery or radiation therapy. It involves regular MRI scans and treating symptoms as they arise.
- Radiation treatment for an acoustic neuroma may shrink or slow the tumor’s growth. This treatment is often used for small tumors or in cases where surgery is not an option.
- Surgical tumor removal may be recommended if it is large or causes significant symptoms. Surgery aims to remove the tumor while preserving hearing and facial nerve function.
Three main ways to remove an acoustic neuroma
- The retro sigmoid approach involves cutting behind the ear and removing some bone to reach the tumor. It can be used for tumors of any size, and some patients may keep their hearing.
- The translabyrinthine approach also involves cutting behind the ear and removing some bones. Still, it also removes part of the inner ear. It can result in complete deafness, but many patients with acoustic neuromas are already deaf before the surgery.
- The middle fossa approach is suitable for small tumors in patients with good hearing. A cut is made above the ear to get to the lesion, and the bone is removed.
Acoustic neuromas are non-cancerous tumors that can seriously impact a person's daily life, even after removing them. The long-term effects of acoustic neuroma surgery may occur, such as losing hearing in one ear and hearing a ringing sound (tinnitus). Even after treatment, hearing loss may continue to be a problem.
The treatment team will choose the best approach for each patient. During surgery, the doctors use advanced monitoring techniques to reduce the risk of damage to nearby nerves and the brain. Acoustic neuroma surgery’s success rate at stopping tumor growth is usually greater than 90%.
It's important to note that each treatment for acoustic neuromas has risks and benefits, and the best approach depends on the individual case. Patients should work closely with their doctors to determine the best course of action for their specific situation.
Treatment centers for acoustic neuroma
 New treatments for acoustic neuroma
New treatments for acoustic neuroma
The aim of developing new tumor treatment methods is to prevent neurological complications, and specialists in neurology and electrophysiology monitor any changes in the activity of facial and auditory nerves and the brain during treatment.
Radiosurgery
One innovative treatment for vestibular schwannoma is stereotactic radiosurgery, which involves delivering precise radiation to the tumor's location in the brain. The tumor's exact position is determined by a series of scans using a metal frame attached to the scalp, similar to a halo. Stereotactic radiosurgery can be performed using a conventional radiation therapy machine, CyberKnife, or GammaKnife.
- GammaKnife has been used to treat acoustic neuroma for a long time. It is a high-precision radiation therapy that does not hurt the patient and can stop small to medium-sized tumors from growing. During GammaKnife treatment for acoustic neuroma, the machine sends multiple beams of radiation straight to the tumor, causing damage to healthy tissue around it. Most people only need one treatment session and can usually return to their lives within a few days. GammaKnife is thought to be a safe and effective way to treat acoustic neuroma, especially for people who need to be better candidates for surgery because of their age, health, or tumor location.
- CyberKnife treatment for acoustic neuroma involves imaging through a CT scan, which is then imported into the CyberKnife treatment planning system. A team of specialists, including a neurosurgeon, an otolaryngologist, a radiological oncologist, and a radiological physicist, works together to plan treatment that targets the vestibular schwannoma while minimizing harm to surrounding critical structures.
Proton therapy
Fractionated stereotactic radiotherapy is another technique that uses a head ring and a beamformer system to deliver photon beams to the tumor's location. The ring is attached to the patient's head, and the linear accelerator directs the photon beam to the tumor, killing its cells based on computed tomography data.
Early intervention with these methods can reduce the risk of hearing loss associated with rapidly growing acoustic neuromas. This alternative treatment for acoustic neuroma has also shown up to a 96% success rate in controlling tumors in patients with acoustic neuroma, even after five years.
If you don’t know what the best treatment for acoustic neuroma is, it depends on several factors, including the size and location of the tumor, the patient's overall health, and their preferences and priorities. It might be worth referring your case to the leading clinics worldwide to check for possible options.
Doctors specializing in acoustic neuroma
 Statistics and prognosis for acoustic neuroma
Statistics and prognosis for acoustic neuroma
As previously mentioned, neuroma on the auditory nerve is a slow-growing tumor that typically does not metastasize. Nevertheless, the disease can lead to certain complications. The most common complication is hearing loss, which can vary in severity and is unique to each patient.
In addition to hearing loss, a large neuroma can impede fluid flow in the brain, leading to hydrocephalus. If left untreated, pressure in the brain can build up inside it, resulting in permanent damage. The enlargement of a neuroma can also place pressure on neighboring brain structures and nerves, causing damage that can be irreversible.
The preferred treatment method for vestibular schwannoma depends on the size of the neuroma, the age and health status of the patient, and other factors. The study indicates that 45.4% of patients undergo surgical treatment, while 54.6% undergo active observation.
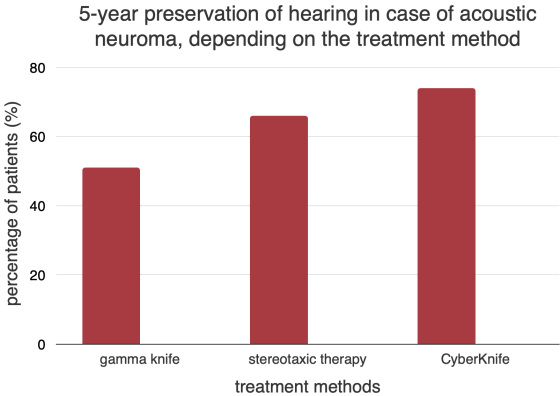
A clinical study published in The New England Journal of Medicine examined the degree of hearing preservation for five years using different treatment methods. After Gamma Knife treatment for acoustic neuroma, the hearing preservation rate was 51%. In comparison, fractional stereotaxic therapy showed a rate of 66%, and CyberKnife treatment resulted in a preservation rate of 74%.
At AiroMedical, our team collaborates with leading ear, nose, and throat surgeons, neurootologists, neurologists, neurosurgeons, neurooncologists, radiation therapy specialists, radiologists, and other healthcare professionals to diagnose and treat the disease early and effectively.
References:
- Meijer, O.W.M., Wolbers, J.G., Baayen, J.C., & Slotman, B.J. Fractionated stereotactic radiation therapy and single high-dose radiosurgery for acoustic neuroma: early results of a prospective clinical study. Int J Radiat Oncol Biol Phys. 2000 Jan 1;46(1):45-9. doi: 10.1016/s0360-3016(99)00328-7.
- Nellis JC, Sharon JD, Pross SE, Ishii LE, Ishii M, Dey JK, Francis HW. Multifactor Influences of Shared Decision-Making in Acoustic Neuroma Treatment. Otol Neurotol. 2017 Mar; 38(3): 392–399. doi: 10.1097/MAO.0000000000001292.
- Greene J, Al-Dhahir MA. Acoustic Neuroma. In: StatPearls [Internet]. 2022 Jan-. Last Update: June 4, 2022. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430812/
- Foley RW, Shirazi S, Maweni RM, Walsh K, McConn Walsh R, Javadpour M, Rawluk D. Signs and Symptoms of Acoustic Neuroma at Initial Presentation: An Exploratory Analysis. Cureus. 2017 Nov; 9(11): e1846. doi: 10.7759/cureus.1846.
- Kabashi S, Ugurel MS, Dedushi K, Mucaj S. The Role of Magnetic Resonance Imaging (MRI) in Diagnostics of Acoustic Schwannoma. Acta Inform Med. 2020 Dec; 28(4): 287–291. doi: 10.5455/aim.2020.28.287-291.
- Mahboubi H, Sahyouni R, Moshtaghi O, Tadokoro K, Ghavami Y, Ziai K, Lin HW, Djalilian HR. CyberKnife for treatment of vestibular schwannoma: a meta-analysis. Otolaryngol Head Neck Surg. 2017 Jul;157(1):7-15. doi: 10.1177/0194599817695805.

















