Cervical Cancer Guide

If cervical cancer is found at stage I, about 92% of women will be alive after five years.
90% of cases of this neoplasm can be avoided using the HPV vaccine at ages 11-12.
Three of every fourth cervix tumor cases can be prevented by screening.
At stage I, there are zero cervical cancer symptoms.
 What is the cervix?
What is the cervix?
Care of women’s health begins with information. The part of the uterus (womb) that sticks out into the vagina is called the cervix. It is a structure in the shape of a cylinder that separates the uterus from the vagina. Its main job is to let sperm into the uterus when a couple is sexually active and to let the baby out when the woman gives birth.
The cervix is also called “the uterus neck.” It comprises the squamous epithelium, a layer of cells outside the cervix, and the columnar epithelium, a layer of cells inside the cervix. The cervix is essential for keeping the pregnancy going because it makes a thick, sticky mucus that keeps the baby in the uterus while the woman is pregnant. It also affects the menstrual cycle because the cervix changes when hormones change.
 What is cervical cancer?
What is cervical cancer?
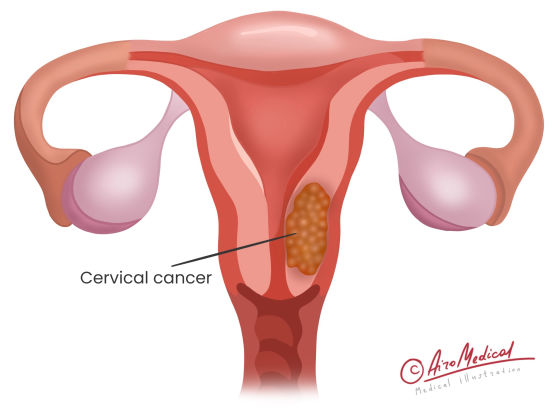 It is a tumor that grows in the cervix and comes in two primary forms:
It is a tumor that grows in the cervix and comes in two primary forms:
- Squamous cell carcinoma is a type of neoplasm that starts in the thin, flat cells lining the cervix's outside. It is the cause of about 90% of all cases that are found and treated.
- Adenocarcinoma is a type that happens less often. It starts in epithelial cells that make mucus and other fluids.
There are also several subtypes of cervical cancer, such as:
- neuroendocrine tumors,
- small cell carcinomas,
- sarcomas.
These subtypes are rare and tend to be more aggressive than squamous cell carcinoma or adenocarcinoma.
Cervical cancer spreads slowly, so most of the time, there is time to find it and treat it before it gets worse. Most often, women between the ages of 35 and 44 are affected. More than 15% of new cases happen in women over 65, especially those without regular checkups.
 What are the causes of cervical cancer?
What are the causes of cervical cancer?
Certain types of human papillomavirus are the main reason people get cervical cancer (HPV). HPV is a virus that can pass between people through sexual contact. There are more than 100 different kinds of HPV, some of which can cause cancer, including cervical.
HPV is a widespread infection, and most people who are sexually active will get at least one form of Human papillomavirus at some time in their lives. Most of the time, the infection will go away on its own and won't cause any problems. But some types of HPV can stay in the body and cause changes in the cells of the cervix. Over time, these changes can lead to malignancy.
Smoking, weak immune systems, and taking birth control pills for a long time are also risk factors. Women who have two pregnancies and more and have had more than one child are also more likely to get cervical cancer.
How to prevent cervical cancer?
It's important to note that cervical cancer is a disease that can be treated and stopped and is most curable when it is found early. Pap tests and HPV tests can help find it early. These tests can see changes in the cervix or abnormal cells that could be early signs of cervical cancer. Some vaccines can protect against getting infected with certain types of HPV, lowering the chance of cervical cancer by 90%.
 What are the symptoms of cervical cancer?
What are the symptoms of cervical cancer?
Women may not feel the pain in the early stages of the disease. However, as cancer progresses and spreads to nearby tissues and organs, women may experience pelvic pain or urinary problems. In addition, some feel a general malaise, tiredness, or decreased appetite. These signs are not necessarily cervical cancer, but it is essential to check for them.
Cervical cancer signs may include something unusual such as:
- Vaginal bleeding: after sex, menopause, a pelvic exam, or between periods,
- Vaginal discharge that is strange in color, consistency, or amount,
- Feelings – for example, pain during sex.
Pelvic pain can be constant or come and go, and it can be mild or harrowing.
It's essential to remember that other things can also cause these symptoms, and many women with cervical cancer don't have any.
 Diagnostic tests
Diagnostic tests
Early stages often have no symptoms and are hard to spot. Usually, it takes a few years before the first signs show up. The best way to avoid this cancer is to find abnormal cells during cervical screening.
Screening also called smear analysis, is essential to get a quick diagnosis. Screening finds changes that could lead to cancer or early cancer before there are any signs or symptoms.
The main goals are to:
- Find precancerous lesions or early-stage.
- Reduce the number of new cases and deaths.
- Give women peace of mind that their risk is low.
- Encourage healthy habits, like getting Pap tests regularly and following up on abnormal test results.
The tests for diagnosing cervical cancer include:
The pelvic organs are looked at by hand and with a speculum to check for any changes in the cervix, uterus, vagina, ovaries, and other nearby organs. There is also the Papanicolaou test (cells are taken to be checked under a microscope). This exam usually takes a few minutes and is done in a room at the doctor's office where exams are done.
Several diagnostic tests also may be used:
- A Pap test (a Pap smear) means taking cells from the cervix and looking at them under a microscope to determine if there are any problems.
- A colposcopy. Powerful optic helps to see the cervix and the surrounding area in more detail.
- During a biopsy, a small piece of suspicious tissue from the cervix is taken under a microscope to discover if there are cancer cells.
- Endocervical curettage (ECC): A small piece of tissue is removed from the cervical canal (the opening to the uterus) during an ECC. After that, it searched under a microscope to see if there were cancer cells.
- The human papillomavirus (HPV) test looks for certain types of HPV known to cause cervical cancer.
- CT scan is a diagnostic procedure that uses X-rays to make detailed pictures of the inside of the body. A CT scan may determine how far the tumor is spreading.
- The magnetic resonance imaging (MRI) technique is a sort of imaging examination that creates in-depth pictures of the body's inside by combining powerful magnets and radio waves. An MRI may determine if cervical cancer has spread to other body parts.
- A positron emission tomography (PET) scan is an imaging examination that creates detailed images of the inside of the body by utilizing a small amount of radioactive material. A PET scan may determine if the neoplasm has extended to other organs and its stage.
Stages of cervical cancer
The treatment plan depends on several things, such as the cancer stage, the type of treatment, and the patient's overall health. Here are some general estimates of how long people are likely to live based on the stage of the tumor when it is found:
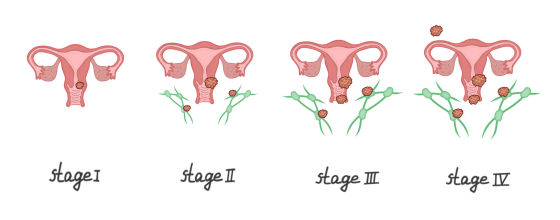
- Carcinoma in situ, or stage 0, means that the cancer is located on the surface of the cervix and has not spread to deeper tissues. About 95% of people at this stage will still be alive after five years.
- Stage I Cancer is only in the cervix and does not spread to lymph nodes or other organs nearby. The survival rate is 92%.
- Stage II: Cancer has spread from the cervix to the uterus or the upper part of the vagina but not to the lymph nodes or other organs. About 83 % of patients at this stage will still be alive after five years.
- Stage III: Cancer has extended to the vagina's lower part of the pelvic walls. It may have also applied to the lymph nodes but not other organs. About 58% of people at this stage will still be alive after five years.
- Stage IV: Cancer has spread to other body parts, like the bladder or rectum. The survival rate is 18% at this stage.
It's important to remember that these survival rates are estimates and may be accurate for some. The treatment team can tell about the prognosis based on the patient's situation.
Where to go to treat cervical cancer?
 Methods of care
Methods of care
Treatment for cervical cancer depends on many factors, like how far along the disease is, how old the person is, and whether or not they want to save the chance to have children in the future.
Some possible ways to treat the condition are:
Surgical treatment is the standard way for cervical cancer. The type of surgery recommended will depend on how far along the cancer is and how healthy the patient is. Some of the most common operations can be any of the following:
- Cryosurgery: Cancer cells are frozen with liquid nitrogen and used in the beginning stages.
- Laser surgery: A laser beam is used to burn cancer cells, and the surgeon can also do it in the early stages of the disease while the patient is still at home.
- Conization: A cone-shaped cervical tissue with changed areas is cut out with a surgical or laser knife.
- Hysterectomy means that the cervix and uterus are taken out. The surgeon can do the surgery by cutting the lower abdomen, going through the vagina, or using a laparoscope.
- Radical hysterectomy: the cervix, the uterus, and the tissues around it, including part of the vagina, are taken out. Some lymph nodes might also need to be removed.
- Trachelectomy: The cervix and part of the vagina are removed the uterus is left in place—an option for people who want to have children in the future.
- Pelvic exenteration: the cervix, uterus, organs, tissues around them, and nearby lymph nodes are removed. If the disease comes back, doctors suggest this method.
Systemic chemotherapy may kill cancer cells that have spread beyond the cervix or shrink a tumor before surgery or radiation therapy. Most of the time, it is given through an IV or a vein in the arm. When used to treat, systemic chemotherapy may cause nausea, vomiting, hair loss, and tiredness. Chemotherapy plans and schedules usually include several cycles over a certain amount of time.
Immunotherapy is a way to fight cancer by using the body's immune system. It works by getting the body to find cancer cells and attack them. Immunotherapy is not often used to treat such tumors. Still, it is being looked at as a possible treatment in clinical trials. Some immunotherapies being studied to treat cervical cancer are medicines that block proteins cancer cells use to hide from the immune system. Another way is cancer vaccines, which trigger the immune system to attack cancer cells.
Targeted therapy is a type of cancer treatment that targets specific molecules or proteins inside cancer cells that help them grow, divide, and spread. It works by stopping these molecules or proteins from doing their jobs. It can stop cancer cells from growing or kill them.
Radiation therapy is a way to treat cancer that uses high-energy radiation to kill or stop cancer cells from growing. It is often used alone or with surgery or chemotherapy. Radiation therapy is usually given in a series of daily sessions over a few weeks. The specific treatment regimen will depend on the stage and location of the tumor and the patient's overall health.
When cervical cancer is found early, there are more ways to treat it. Doctors will think about how the disease and treatment will affect the patient's sexual function, ability to have children, and other things when making a treatment plan.
What clinics do we recommend for cervical cancer?
 New treatment options
New treatment options
Researchers worldwide always look for better ways to prevent and treat cervical cancer. Some of the new things that look good are the following:
- Transarterial chemoembolization (TACE) is a minimally hurting procedure used to treat metastases from primary tumors. It involves putting a chemotherapy drug right into the affected area (through the vessels). Embolization is the blocking of blood vessels that feed cancer. It stops the flow of blood and keeps the chemotherapy inside the tumor.
- Transarterial chemoperfusion (TACP) can also be used for cancer that has extended to other organs. During the procedure, tiny beads of the chemotherapy drug are put into the blood vessels that feed the tumor. It is done with a catheter. The beads block the blood vessel, so blood can't reach the tumor. At the same time, the balls release drugs that are used in chemotherapy to shrink the tumor.
- Brachytherapy, also called "internal radiotherapy," is a type of radiation therapy in which microscopic beads containing a radiation source are injected directly into the tissue of the cervix. It makes it possible to act now on cancer.
- Proton therapy is a type of radiotherapy in which a beam of radiation (protons) with a particular amount of radiation is sent right to the affected area of the cervix while avoiding and not hurting nearby tissues.
- High-Intensity Focused Ultrasound (HIFU): Special tools are used to focus beams of ultrasonic energy. At the point where the rays meet, tissue is "ablated" or destroyed by heat. It means that oncologists can treat the tumor without surgery. This non-invasive technology makes it possible to treat malignancy deep inside the body without hurting healthy tissue.
- Da Vinci robot-assisted surgery uses a robotic system to remove the affected organ. With the da Vinci system, gynecological surgeries can be done with more minor cuts, which lowers the risk of complications and speeds up recovery. Some women with cervical cancer, especially those with larger tumors, can be operated on by a robotic system. Or, patients whose cancer has spread to lymph nodes nearby may be able to have surgery with the help of a robot. It can be used with other treatments, like chemotherapy or radiation therapy.
Cancer of the cervix is a slow-moving disease that can still lead to death outcome. However, now that modern treatment methods exist and are used, the patient can improve their life quality and live longer.
Who treats cervical cancer the best?
 Statistics and prognosis
Statistics and prognosis
The World Health Organization says cervical cancer is women's fourth most common type. It will cause more than 600,000 new cases and more than 350,000 deaths in 2021. Not long ago, cervical cancer was the main reason women died worldwide. It was an alarming trend, but research into screening, diagnosis, and treatment has changed this.
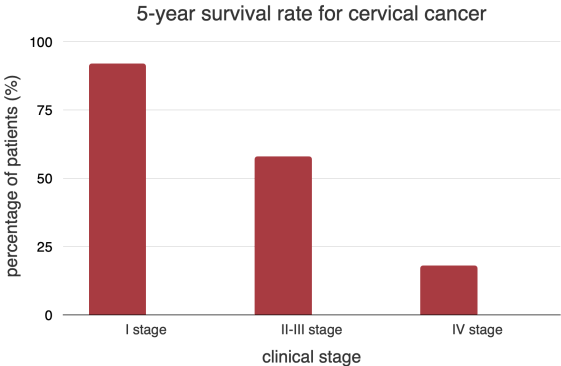
The American Cancer Society has found that 92% of people with stage I cervical cancer will still be alive after five years. Cancer in stages II–III has a 58% chance of being gone after five years, while cancer in stage IV has an 18% chance of being gone after five years.
Cancer of the cervix is curable. How well cancer treatments work depends on many things, like the stage, type, and location of cancer. Studies show that only 10–15 percent of people with early-stage cervical cancer have it come back after treatment. Also, we can prevent it through regular check-ups.
Imagine that you or someone in your family is told they have cervical cancer. In that case, the most important thing is to find a group of professionals who can talk to you. Tell you in detail about the treatment plan and help you decide which option will help you improve as quickly as possible.
Like any other problem, cancer is a problem only if you don't know how to solve it.
AiroMedical can solve and help.
References:
- National Cancer Institute: Human Papillomavirus (HPV) Vaccines
- Cancer Council NSW: Staging and prognosis for cervical cancer
- American Cancer Society: Risk Factors for Cervical Cancer
- WebMD: Cervical Cancer
- Cancer.Net: Cervical Cancer: Statistics
- NHS inform: Cervical cancer
- National Library of Medicine: Colposcopy and Treatment of Cervical Precancer

















