Stroke Guide

One person dies from a stroke every 3.5 minutes.
One will have a stroke for every four adults aged 25 and up worldwide.
It is possible to prevent 8 out of 10 strokes by changing the lifestyle and managing risks.
Annually, 15 million people have a stroke; 5 million die, and 5 million suffer disabilities.
 Some about the brain and its blood vessels
Some about the brain and its blood vessels
The brain contains various areas, each responsible for specific functions:
- The frontal lobe is responsible for thinking and movement control;
- The parietal lobe for processing sensory information;
- The temporal lobe for managing hearing and language;
- The occipital lobe for interpreting vision;
- The cerebellum for maintaining balance;
- The brainstem for regulating vital functions like breathing.
Blood vessels in the brain play a critical role in our well-being, as they supply oxygen and nutrients to keep the brain healthy. Under normal conditions, these vessels ensure proper blood flow and regulate blood pressure for smooth functioning.
However, bleeding or blood clots (thrombosis) can disrupt the blood vessels' normal function and potentially lead to a stroke.
 What’s a stroke?
What’s a stroke?
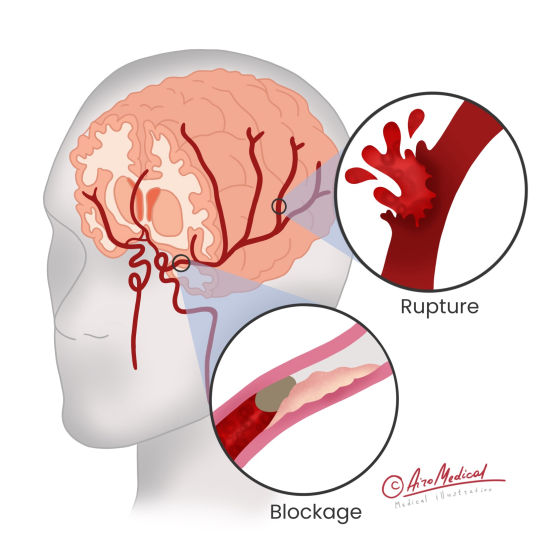 It occurs when blood circulation to the brain is stopped. A stroke causes brain cells to lose oxygen and essential nutrients, which makes them stop working and die quickly. When brain cells die, the brain can't work correctly, leading to difficulty moving, speaking, thinking, etc.
It occurs when blood circulation to the brain is stopped. A stroke causes brain cells to lose oxygen and essential nutrients, which makes them stop working and die quickly. When brain cells die, the brain can't work correctly, leading to difficulty moving, speaking, thinking, etc.
During a stroke of the brain, the lack of blood flow causes various issues. Brain cells can't do their everyday tasks and begin to die within minutes. It affects the brain's ability to send and receive messages, causing stroke symptoms.
The seriousness of a stroke depends on where it happens in the brain and how big the affected area is. The aim is to treat patients ASAP, within 60 minutes of arriving at the hospital, known as the "golden hour".
Types of strokes by location
Different strokes can happen in any part of the brain where blood vessels are present:
- Stroke at the brainstem, including the pontine, can affect breathing, heartbeat, and speech, often leading to severe disabilities or death. Some symptoms include difficulty speaking or swallowing, weakness or numbness in the face, double vision, dizziness or imbalance, and trouble with coordination and movement.
- Cerebellum strokes cause problems with coordination, balance, and fine motor skills, making it difficult for patients to move and perform everyday tasks.
- A stroke of the spine can cause paralysis, loss of feeling, and difficulty with bladder or bowel control, depending on the specific location of the damage.
- Thalamus stroke causes sensory and motor issues and problems with memory, speech, and emotional problems since the thalamus is a critical relay center for many brain functions.
Stroke by origin hemorrhagic vs. ischemic
There are two main kinds of stroke:
Ischemic stroke
It happens when a blood clot, thrombus (or a fatty deposit) blocks a blood vessel, limiting the blood supply to a brain part. Acute ischemic strokes, which account for 87% of all strokes, can occur in large and small blood vessels. They usually happen in the middle, anterior, and posterior cerebral arteries.
There are two main kinds of ischemic strokes:
- A thrombotic stroke happens when a blood clot forms within an artery in the brain, obstructing blood flow. It is often caused by plaque buildup in the arteries. It is often caused by plaque buildup in the arteries.
- An embolic stroke occurs when a thrombus or debris from another body part travels through the bloodstream and gets stuck in a brain artery. It stops blood flow and causes a stroke. Embolic strokes are usually caused by clots that come from the heart.
Hemorrhagic stroke
This type occurs when the brain blood vessel ruptures or leaks, causing bleeding in the brain. Hemorrhagic strokes make up 13% of all strokes. They can happen in different brain parts, such as the space around or inside the tissue.
The kind of stroke and its specific location in the brain will determine the symptoms a person experiences and the severity of the stroke.
 What causes a stroke?
What causes a stroke?
There are two main ways how does a stroke happen. The first is a blocked artery; the second is a leaky or blood vessel burst. Some people have a short blood flow disruption in the brain, called transient ischemic attacks (or TIA strokes), without long-lasting symptoms.
The main risk factors for stroke
The most common risk factors for stroke include:
- High blood pressure is the most significant risk factor, putting extra strain on blood vessels. Due to the study, if someone has high blood pressure with a systolic reading of 160/95 mm Hg or higher, stroke risk is about four times higher than someone with normal blood pressure.
- Common heart issues in stroke patients include heart attack, heart failure, and irregular heartbeats like atrial fibrillation, ventricular tachycardia, and ventricular fibrillation.
- Smoking can damage blood vessels and increase about twice the risk of experiencing a stroke in their lifetime compared to those who have never smoked.
- Diabetes: High blood sugar levels damage blood vessels and double the risk of clots.
- High cholesterol: studies found that high cholesterol is linked to lacunar stroke. The highest level was associated with twice the risk for this type.
- Obesity: Being overweight can contribute to high blood pressure, high cholesterol, and diabetes, so the risk of stroke increases. For every unit increase in BMI (body mass index) over 20, the risk of ischemic stroke increases by 5%.
- Drinking too much alcohol raises blood pressure and leads to other risk factors.
- Low physical activity: A sedentary lifestyle increases blood pressure, cholesterol, and body mass.
- Age: Approximately every ten years after turning 55, the likelihood of having a stroke doubles.
- A family history of strokes or heart conditions increases the risk.
- Personal history: A previous stroke or TIA increases the risk of future strokes.
- Gender: 40% of women have high blood pressure, and unique stroke risks include pregnancy-related high blood pressure, certain birth control medicines, smoking, and higher depression rates.
Concerning the question, can stress cause a stroke? The fact is that constant stress might increase the chances of experiencing a heart attack or stroke, as suggested by a recent study.
How to prevent stroke?
To prevent stroke, follow these healthy lifestyle choices and manage medical conditions:
- Control blood pressure by reducing salt intake, exercising regularly, and taking prescribed medications. Lowering diastolic blood pressure by just five mm Hg can reduce stroke risk by around 34%.
- Manage cholesterol: Eat a low-fat, high-fiber diet and take medications if necessary. The latest stroke research indicates that reducing cholesterol may decrease the chance of another stroke by around 20%.
- Quit smoking: Eliminate tobacco use to reduce stroke risk.
- Limit alcohol intake in moderation or not at all.
- Maintain a healthy weight: Exercise regularly and eat a balanced diet.
- Exercise regularly: 150 minutes of moderate-intensity aerobic activity weekly is recommended.
- Manage diabetes: Monitor blood sugar levels, follow a diabetic-friendly diet, and take medications as prescribed.
- Eat a healthy diet of fruits, vegetables, whole grains, lean proteins, and healthy fats.
- Reduce stress: Practice stress-reduction techniques such as meditation, yoga, or deep breathing exercises.
Additionally, make sure to have regular medical checkups and follow your doctor's recommendations for managing any existing health conditions that increase the risk of stroke. It is much easier than achieving recovery from a stroke.
 Symptoms and signs of a stroke
Symptoms and signs of a stroke
If you ask, “How do I know if I am having a stroke” here’s a short and informative answer.
Remember that time is crucial during a stroke! Prompt treatment can reduce the brain damage that may result from a stroke. By recognizing the symptoms of a stroke, you can act quickly and potentially save a life, even your own.
Use the algorithm FAST to detect if you or someone else experiences a stroke.
- Face: Is the person able to smile? Do they have a drooping mouth or eye?
- Arm: Can the person lift both arms?
- Speech: Can the person speak clearly and repeat your words?
- Time: Deal emergency if you notice even one of these symptoms.
Signs of a stroke
Even if the symptoms, like a droopy face from a stroke, are brief, they might still indicate brain damage. Immediately call an ambulance if you or someone you know has any of the symptoms that occur suddenly:
- Face, arm, or leg numbness or weakness, particularly on one side of the body;
- Confusion, difficulty speaking or understanding speech;
- Vision problems in one or both eyes;
- Dizziness, loss of balance or coordination, trouble walking;
- Severe headaches with no known reason.
Other warning signs may include double vision, drowsiness, and nausea or vomiting.
A stroke happens quickly, so acting fast when you notice any of these symptoms is crucial.
Don't drive yourself to the hospital or ask someone else guides you. Call for an ambulance so medical staff can start lifesaving treatment for brain stroke on the way to the emergency room.
Some people might have symptoms like headaches or numbness before a severe stroke. A study found that 43% had signs of mini-stroke up to a week before a significant episode.
How to recognize a stroke?
Some differences exist between conditions with similar symptoms.
Bell's palsy vs. stroke
Bell's palsy and stroke both involve sudden onset symptoms but differ. Bell's palsy causes facial weakness or paralysis on one side of the face, difficulty with facial expressions, problems closing the eye, drooling, altered taste, and increased sensitivity to sound in one ear. In contrast, a stroke leads to one-sided weakness or numbness, confusion, difficulty understanding or speaking, vision problems, severe headache, dizziness, and loss of balance.
Stroke vs aneurysm
Aneurysms are different from strokes. An unruptured aneurysm often has no symptoms, but a large one can cause pain, vision changes, or other neurological signs depending on location. A ruptured aneurysm can also lead to hemorrhagic stroke, which shares similar symptoms with a regular stroke.
Stroke symptoms in women are generally the same as in men. However, the study found more frequent headaches, mood changes, confusion, nausea, feeling odd, tiredness, or discomfort. Man stroke symptoms like coma, paralysis, speech issues, swallowing problems, and urinary incontinence are fewer compared to those in women.
 How is a stroke diagnosed?
How is a stroke diagnosed?
Diagnosing a stroke involves checking a person's symptoms and using special methods, including imaging techniques. These tests for strokes help doctors discover the cause and the part of the affected brain.
Clinical evaluation
When someone arrives at the hospital with possible stroke symptoms, the doctor will examine them and may do blood tests, check their pulse, and measure their blood pressure.
Imaging methods
To diagnose a stroke, two main imaging methods are used to look at the brain when a stroke is suspected: CT and MRI scans.
- CT scans create a 3D brain image using multiple X-ray images. They are usually faster than MRI scans.
- MRI scans use strong magnetic and radio waves to make detailed brain pictures. This method is helpful when the symptoms are complex or when it's unclear where the damage is in the brain.
Additional tests
Other tests, such as a swallow test, determine if the person can swallow adequately. A carotid ultrasound scan checks for any problems in the neck arteries, and an echocardiogram examines the heart, including a stroke assessment. These tests help doctors create the right plan to treat a stroke.
Stages of the stroke: How is it evolve?
The seven stages of stroke recovery are:
- After a stroke, muscles become weak and unresponsive.
- Muscles start to tighten and become stiff as nerves recover.
- Muscles get tighter, causing difficulty and movement pain.
- Muscles regain some control as spasticity reduces.
- As patient coordination improves, movements can be more difficult.
- Muscle control becomes refined as tightness fades.
- Patients regain most or all pre-stroke movement abilities.
Each patient's recovery is unique; not everyone will reach all stages.
 What is the treatment for stroke?
What is the treatment for stroke?
Stroke treatment depends on its type and underlying cause. The main goal is to restore blood flow to the brain and minimize brain damage. Here are some standard treatment options for stroke:
If you have an ischemic stroke
Treatments for ischemic stroke that happens because of a blood clot that blocks circulation to the brain aim to dissolve or remove the clot.
Medications to dissolve a clot
Drugs for thrombolysis are conservative medications for the treatment of embolic stroke. Clot-dissolving medications, such as alteplase (tPA), can be given within 4.5 hours of stroke symptoms. It is an emergency treatment, so the sooner it is used, the better the chances of recovery. Using tPA by itself, the success rate was about 37%.
Angioplasty & stent
Stroke treatment with angioplasty and stent placement involves using a catheter to navigate to the blocked blood vessel in the brain. The angioplasty balloon is inflated to open the narrowed artery, and then a stent is placed to keep it open, improving blood flow and reducing the risk of another stroke. The success rate of the procedure reaches 99%.
Carotid endarterectomy
The procedure helps prevent strokes by removing plaque buildup from the carotid arteries, which supply blood to the brain. It's recommended for patients with mild strokes, transient ischemic attacks, and severe artery narrowing. The procedure involves an incision in the neck, opening the affected artery, and removing the plaque.
In case of hemorrhagic stroke
Treatment for hemorrhagic stroke caused by a burst or leaking blood vessel aims to control bleeding and reduce pressure on the brain.
Blood pressure control
Blood pressure management is done by medications to lower high blood pressure and reduce the risk of further bleeding as a part of treatment for acute stroke.
BP control involves using stroke medications such as ACE inhibitors (e.g., lisinopril), beta-blockers (e.g., metoprolol), calcium channel blockers (e.g., amlodipine), and diuretics (e.g., hydrochlorothiazide) to lower high blood pressure, which helps reduce the risk of further bleeding. Hydralazine (Apresoline) is used in hypertensive emergencies, dilating arterioles to improve blood flow and cardiac output during stroke treatment.
Surgical treatment
In some cases, various types of surgery may be needed to repair the damaged blood vessel, remove the blood, or relieve pressure on the brain. Some options include:
- Hematoma removal: Surgeons remove a piece of the skull during open surgery to access and remove the blood clot.
- In aneurysm neurosurgical clipping, a surgeon opens the skull to reach the aneurysm. They put a small metal clip on the aneurysm's base to stop blood flow and prevent massive bleeding. It helps keep the aneurysm stable and protects nearby brain areas.
- Endovascular coiling is a minimally invasive treatment for stroke used to treat brain aneurysms, preventing them from causing hemorrhagic strokes. By inserting soft platinum coils into the aneurysm through a catheter, the blood clots, sealing off the aneurysm from the blood circulation and reducing the risk of rupture or bleeding.
The chosen treatment depends on factors like hemorrhage location and size, the patient's health, and the medical team's expertise.
Standard after-stroke treatment
After a stroke, treatment is essential to help patients recover and regain their independence. It typically involves various therapies:
Medications
Various drugs can be used post-stroke treatment to prevent blood clots, lower blood pressure, and reduce cholesterol levels. Common drugs include blood thinners, statins, and blood pressure medications.
Rehabilitation for stroke
Rehabilitation after stroke helps patients regain their daily life. It includes various therapies focusing on different aspects of recovery, including inpatient stroke rehabilitation:
- Physical therapy in paralysis stroke treatment aims to improve strength, balance, coordination, and mobility. Physical therapists create personalized exercise programs for patients.
- Mirror therapy is a simple method to help stroke patients get better at moving their limbs. The patient looks at a mirror showing their healthy limb while trying to move the weak one. This allows the brain to relearn movements and aids in recovery.
- Occupational therapy helps patients regain to do daily activities like dressing, eating, and personal hygiene. They may suggest adaptive equipment or home modifications.
- Speech therapy is a stroke rehabilitation that addresses communication and swallowing difficulties. It involves muscle-strengthening exercises or alternative communication methods.
- Cognitive therapy: Improves cognitive skills like memory, problem-solving, and attention. It can also help with emotional challenges like depression or anxiety.
- Recreational therapy: Uses leisure activities to boost physical, cognitive, and emotional well-being during rehabilitation for a stroke. Activities include art, music, sports, or games.
Lifestyle changes
Adopting a healthy lifestyle is essential for preventing future strokes. It includes maintaining a balanced diet, exercising regularly, quitting smoking, and limiting alcohol consumption.
Ongoing medical care
Regular check-ups are essential for monitoring recovery and managing any ongoing health issues related to the stroke.
The main principles of standard stroke treatment focus on prompt diagnosis, immediate administration of appropriate medication, and complex rehabilitation from stroke.
Rehabilitation centers for the stroke patients
 New treatments for stroke
New treatments for stroke
New stroke treatments are continually developed to improve patient outcomes and recovery. Some of them are promising:
Stem cell therapy
Researchers are exploring stem cells’ potential, calling it a breakthrough in stroke treatment. It helps promote brain tissue healing and regeneration after a stroke. It could potentially help improve functional recovery and reduce long-term disability.
Due to the latest studies, stroke treatment with stem cells has shown promising results, helping to repair damaged brain cells and protect the brain from further harm. This therapy leads to better brain function and increased survival rates.
Repetitive transcranial magnetic stimulation (rTMS)
It is a new way of treating stroke. It is a non-invasive method being researched for depression after stroke treatment with promising efficacy in around 60%. It uses a device on the scalp to send magnetic fields into specific brain regions to modify their activity.
Depending on the affected side, rTMS can be applied at low, medium, or high frequencies. For example, if a stroke weakens the left side of the body, low-frequency rTMS would stimulate the left side of the brain, while medium or high-frequency rTMS would target the right-sided.
Deep brain stimulation (DBS)
This technique uses electrodes placed inside the brain to help with stroke recovery. It targets brain areas linked to movement problems and has shown the potential to improve motor function. It activates nerve cells and supports motor rehabilitation, helping patients with leg issues by stimulating difficult-to-reach areas. Some patients have seen improvements in arm movement after DBS.
Neuromuscular electrical stimulation (NMES)
It is a treatment for stroke patients that uses electrical impulses to stimulate all affected muscles and improve their function. By sending signals to the muscles, NMES helps strengthen them, regain movement, and enhance overall motor function after a stroke. For swallowing restoration, the NMES treatment effective rate is 90.91%.
Hyperbaric oxygen therapy (HBOT)
It is a stroke treatment where patients breathe pure oxygen in a pressurized room. It helps improve blood flow, lowers inflammation, and aids brain healing. HBOT led to a notable improvement in cognitive function, benefiting 86% of stroke patients.
New stroke rehabilitation techniques
Newer techniques help people recover more quickly and effectively than traditional stroke rehab methods.
Robotic rehabilitation
Robotic stroke rehabilitation is an innovative approach to stroke recovery that uses automatic devices such as exoskeletons or robotic gloves to help patients regain their motor function, for example, walking after a stroke.
These devices assist in repetitive, task-specific training—this help to rebuild the connections and improve movement in arms and legs, balance, and walking. Robotic devices enhance traditional therapy methods by providing consistent, precise, and adjustable support, making rehabilitation more effective and efficient.
Constraint-induced movement therapy (CIMT)
One of the stroke rehabilitation techniques that helps improve the use of a weak or affected arm. In this therapy, the unaffected arm is restrained or restricted, encouraging the patient to use their affected arm more. CIMT helps the brain reorganize and develop motor skills by repeatedly doing focused, goal-driven tasks and activities.
Virtual reality (VR)
It is a tool used as a new treatment for stroke rehabilitation to create realistic and interactive settings. It helps patients practice movements, thinking, and communication engagingly. With VR, patients receive instant feedback, and the activities can change based on their progress and needs.
Brain-computer interfaces (BCIs)
The tool lets patients control computers or devices with their brain signals. This technology helps patients relearn movements and boost motor skills by encouraging the brain to reorganize and adapt—BCIs used in inpatient or outpatient rehabilitation show the potential to help with thinking and movement rehab.
Botulinum toxin
Injections, known as Botox, can treat specific side effects of a stroke, particularly for muscle spasticity and stiffness. Spasticity leads to pain, contractures, and difficulty with movement and daily activities. Botox works by temporarily blocking nerve impulses to muscles, thereby reducing muscle contractions and relaxing the muscles. It also can be used as a treatment for double vision after a stroke.
Alternative treatments for stroke
These techniques can be used with standard therapies to help with recovery:
- Acupuncture: Using thin needles to improve blood flow and promote healing.
- Massage therapy: Helps relax muscles and improve circulation.
- Herbal medicine: Supplements like ginkgo biloba may support brain health.
- Biofeedback: Teaches patients to control bodily functions for stress management.
- Mind-body practices: Yoga, tai chi, and meditation can reduce stress and improve well-being.
- Aromatherapy: Essential oils can help with relaxation and emotional health.
Before trying these treatments, discuss them with a healthcare professional. They should be used with, not instead of, regular medical care.
Certified stroke rehabilitation specialist
 Stat results for stroke patients
Stat results for stroke patients
Recovery after a stroke can differ significantly among patients. By looking at statistics, we can better understand the possible outcomes and what to expect for patients and their families.
Helping stroke survivors walk again is a crucial goal. In a study from the U.S. National Institutes of Health, patients did rehab for two years, and in the end, 74% of them could walk independently.
Prognosis of stroke recovery
The timeline for stroke recovery varies for each person and depends on factors like stroke severity, brain area affected, age, and health. Some people recover well, while others have lasting disabilities.
The answer is yes to whether you die of a stroke. One in every six deaths from heart disease is caused by a stroke, due to the Centers for Disease Control and Prevention.
The National Stroke Association states that 10% of patients recover almost entirely, and 25% recover with minor issues. However, 40% face moderate to severe problems needing special care, affecting daily life. Additionally, 10% need long-term care in places like nursing homes.
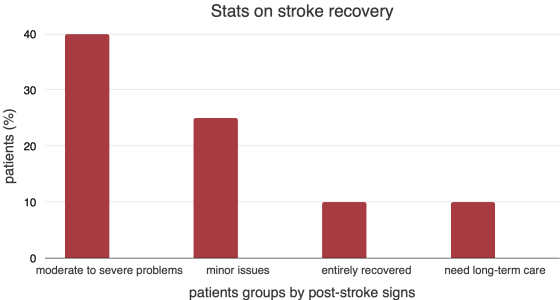
Early and consistent rehab helps improve recovery, but each person's journey is unique, making it hard to predict the outcome.
Life expectancy after a stroke
Due to the study, after a stroke, 79% of people survive two years after a stroke, and the survival rate decreases as time goes on. About 61% of individuals survive three years after stroke, and only 5% survive 16 years. The number drops to 1% of people staying alive 20 years after a stroke. Remember that it may vary based on age, overall health, and stroke severity. Life expectancy after a mini-stroke is greater but TIA still short life by 20%.
Patients who have strokes always have to deal with serious problems. It is the main reason why adults have been disabled for a long time and the main reason why they are severely disabled. The best way to get back on your feet after a stroke is to let a team of professionals like Airomedical plan a program just for you that will help you heal, keep your dignity, and stay motivated.
References:
- Bao S, Khan A, Song R, Tong RK. Rewiring the Lesioned Brain: Electrical Stimulation for Post-Stroke Motor Restoration. J Stroke. 2020 Jan;22(1):47-63. doi: 10.5853/jos.2019.03027. PMID: 32027791; PMCID: PMC7005350.
- Berlet R, Anthony S, Brooks B, Wang ZJ, Sadanandan N, Shear A, Cozene B, Gonzales-Portillo B, Parsons B, Esparza Salazar F, Lezama Toledo AR, Rivera Monroy G, Vega Gonzales-Portillo J, Borlongan CV. Combination of Stem Cells and Rehabilitation Therapies for Ischemic Stroke. Biomolecules. 2021 Sep 6;11(9):1316. doi: 10.3390/biom11091316. PMID: 34572529; PMCID: PMC8468342.
- Yang S, Li R, Li H, Xu K, Shi Y, Wang Q, Yang T, Sun X. Exploring the Use of Brain-Computer Interfaces in Stroke Neurorehabilitation. Biomed Res Int. 2021;2021:9967348. doi 10.1155/2021/9967348. PMID: 34239936; PMCID: PMC8235968.
- Somani A, Kar SK. Efficacy of repetitive transcranial magnetic stimulation in treatment-resistant depression: the evidence thus far. Gen Psychiatr. 2019;32(4):e100074. doi 10.1136/psych-2019-100074. PMID: 31552384; PMCID: PMC6738665.
- Jerath NU, Reddy C, Freeman WD, Jerath AU, Brown RD. Gender Differences in Presenting Signs and Symptoms of Acute Ischemic Stroke: A Population-Based Study. Gend Med. 2011 Oct;8(5):312-319. doi: 10.1016/j.genm.2011.08.001. PMID: 21925968; PMCID: PMC3324562.
- Hadanny A, Rittblat M, Bitterman M, May-Raz I, Suzin G, Boussi-Gross R, Zemel Y, Bechor Y, Catalogna M, Efrati S. Hyperbaric oxygen therapy improves neurocognitive functions of post-stroke patients – a retrospective analysis. Restor Neurol Neurosci. 2020;38(1):93-107. doi: 10.3233/RNN-190959. PMID: 31985478; PMCID: PMC7081098.
- Sadighi A, Stanciu A, Banciu M, Abedi V, El Andary N, Holland N, Zand R. Rate and associated factors of transient ischemic attack misdiagnosis. eNeurologicalSci. 2019 Jun;15:100193. doi 10.1016/j.ensci.2019.100193. PMID: 31193470; PMCID: PMC6529772.

















