Prostate Cancer Guide

About 1 in 8 men will get prostate cancer during his life.
The early-stage prostate cancer 5-year survival rate is 99%.
About 60% of malignant prostate tumors are detected at age 65+.
A family history of the neoplasm in the prostate gland doubles the risk of getting it.
 Some info about the prostate gland
Some info about the prostate gland
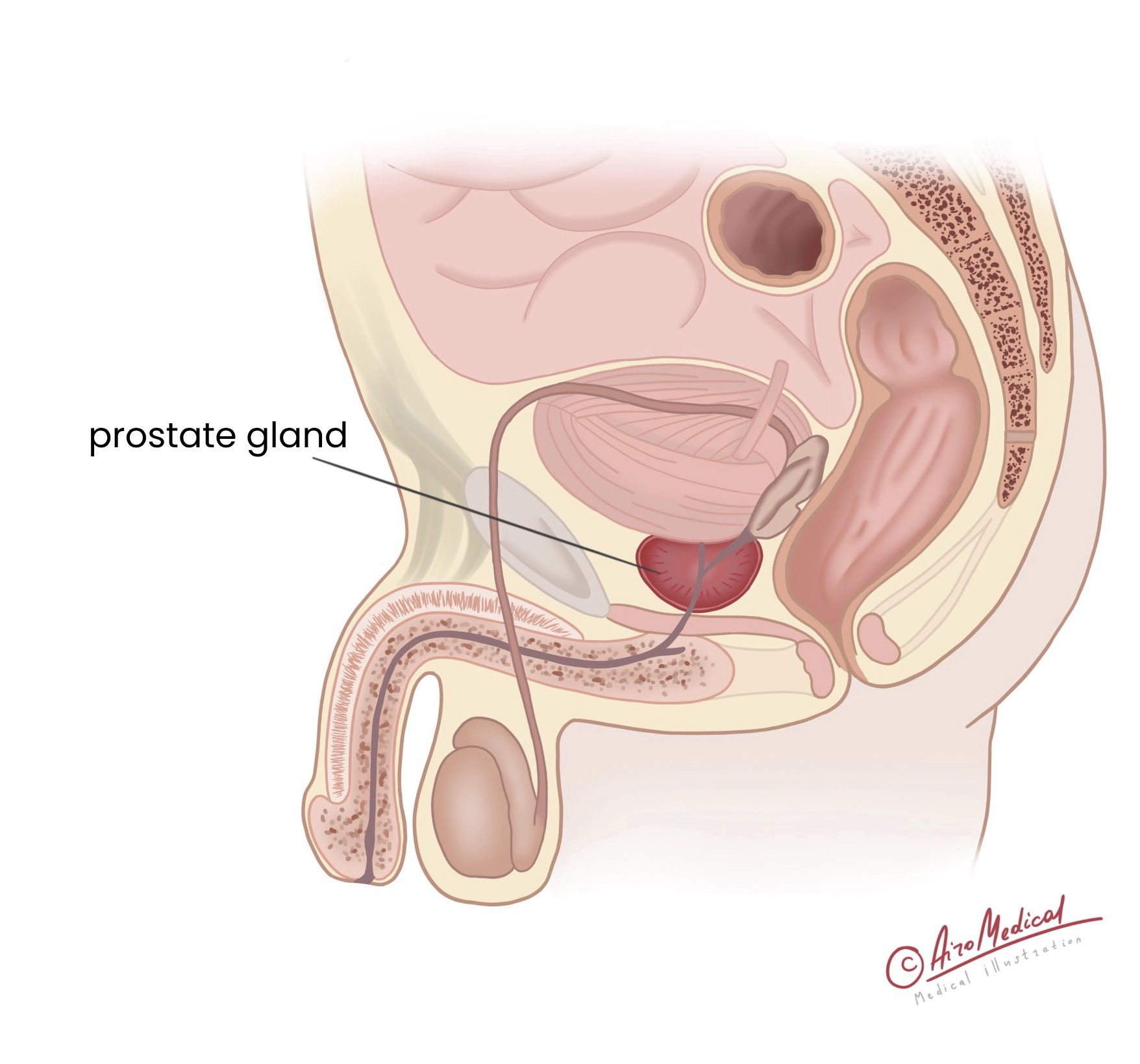 Between the penis and the rectum is a small, rubbery prostate gland. It helps make seminal fluid (semen), which mixes with sperm from the testicles. Sperm need seminal fluid to move and stay alive.
Between the penis and the rectum is a small, rubbery prostate gland. It helps make seminal fluid (semen), which mixes with sperm from the testicles. Sperm need seminal fluid to move and stay alive.
There are different parts of the gland. Malignancy usually starts in the area around the rectum. During a digital rectal exam, this is why the doctor looks at the prostate with a gloved finger (DRE).
Life does not depend on the prostate, but reproduction does. Sperm can live and reproduce only in healthy sperm. Semen has zinc, citrate, fructose, and enzymes like PSA, which are used to check for prostate cancer. Semen may help keep germs and infections from getting into the urinary tract and sperm.
The prostate gland’s cell types include:
- Epithelial cells that produce semen.
- Stromal cells shape and sustain the prostate gland.
- Prostate smooth muscle cells regulate urine and sperm flow.
- Endothelial cells line prostate blood arteries and control blood flow.
- Immune cells protect the prostate from infection.
 What is prostate cancer?
What is prostate cancer?
 Malignancy in the prostate starts in the gland’s cells, specifically in the epithelial cells that line the gland. These cells change and begin to grow out of control, which is what causes a tumor to form. The cancerous cells could then move to other body parts, like the bones and lymph nodes.
Malignancy in the prostate starts in the gland’s cells, specifically in the epithelial cells that line the gland. These cells change and begin to grow out of control, which is what causes a tumor to form. The cancerous cells could then move to other body parts, like the bones and lymph nodes.
Tumors in the prostate are not always cancerous. Adenomas don't spread to other body parts, so they don't pose a health risk.
The condition is considered the most common type of oncological illness in men. Statistics from the American Cancer Society show that a man will be diagnosed with prostate cancer once every eight years for his life.
A bad thing about such cancer is that its malignant growth is slow but spreads fast. Compared to cancers of the esophagus or liver, prostate cancer grows very slowly. However, even small tumors can spread throughout the body and kill the patient. Even though neoplasm is still in its early stage, it can metastasize and spread to other organs and parts of the body (spine, hips, pelvis, liver). And it is the most worrying thing.
There are several types of prostate cancer, including:
- Adenocarcinoma is the most frequent cancer type and starts in the cells that produce prostate gland secretions.
- Small cell carcinoma: This rare type is often more aggressive than adenocarcinoma.
- Squamous cell carcinoma grows from the flat, scale-like cells that line the prostate gland.
- Transitional cell carcinoma starts from the cells that line the prostate gland's tubes, which transport semen.
- In situ, prostatic ductal carcinoma is non-invasive cancer in the prostate's ducts.
- Prostatic neuroendocrine carcinoma develops from the neuroendocrine cells of the prostate.
It's essential to note that some tumors may be more aggressive and fast-growing than others, and treatment options will depend on the type and stage of cancer.
 What are the risk factors?
What are the risk factors?
The leading causes are:
Age. Prostate cancer rates rise with age. It affects 60% of 65-year-old males. That's why middle-aged men should discuss PSA testing with their doctors.
Family history. Some diseases are inherited. Parent-to-child transmission is the highest. Genes cause 58% of malignant neoplasms. Men with a close relative with it are twice as likely to have it, and those with two or more relatives are roughly four times as likely. Risk increases if a family member is diagnosed before 60.
Genetic factors. As we understand more about how genes cause cancer, men with a strong family history of breast, ovarian, colon, or pancreatic neoplasms may also have a higher risk of prostate cancer. Because families share many genes, multiple genetic factors may increase risk in a family. However, mutations in genes like BRCA2 can raise the risk. Men with these gene mutations may need additional testing.
Race. Why black men are 75% more likely than white men to have prostate cancer and over twice as likely to die from it is unknown. Black males had a higher death rate due to socioeconomic factors such as access to healthcare, insurance, PSA screening, treatment, and follow-up. It is also crucial to realize that not all Black men get such neoplasm and that early detection improves treatment and cure rates.
Other risk factors are:
- Diet: Men may be more likely to get prostate cancer if they eat a lot of animal fat and not enough fruits and vegetables.
- Exposure to certain chemicals: Men exposed to chemicals like cadmium and pesticides may be more likely to get malignancy.
- Obesity. Men who are overweight or obese might be more likely to get malignant prostate tumors.
- Inflammation: Men with a history of chronic inflammation, such as from inflammatory bowel disease, may have a higher risk of prostate cancer.
It's important to remember that having a risk factor doesn't mean a person will get prostate cancer. At the same time, many men don't have any known risk factors and get a neoplasm.
How to fewer the risk?
Doctors recommend doing several things to lower the chance of getting prostate cancer. Here are some of them:
- A healthy diet includes fruits, vegetables, and whole grains.
- Keeping the weight in a good range;
- Regular exercise will help;
- Neither smoking nor using tobacco;
- Putting limits on alcohol use;
- Getting screenings regularly, starting at age 50 or earlier, if you are at a higher risk.
It is essential to talk to a urologist to find out the best way to lower your risk based on your health and your family's health history.
 What are the signs of prostate cancer?
What are the signs of prostate cancer?
Most tumors don’t cause any symptoms at all, but the following can be signs and symptoms of prostate cancer:
- Difficulty starting or stopping urination;
- Weak or interrupted urine flow;
- A frequent need to urinate, especially at night;
- Pain or discomfort while urinating;
- Blood in the urine or semen;
- Painful ejaculation;
- Pain or discomfort in the lower back, hips, or upper thighs.
An enlarged prostate gland can cause discomfort or pain when sitting.
However, many men with early stages do not have any symptoms.
Similar symptoms can also be caused by prostate conditions that aren't cancer. A bladder infection or other health problems can also cause urinary symptoms.
The prostate cancer symptoms of the spreading tumor are:
- Back, hip, thigh, shoulder, or pain in other bones;
- Leg or foot swelling or fluid buildup;
- Loss of weight for no visible reason;
- Fatigue;
- Changes in the way your gut is working.
 Diagnostic tests
Diagnostic tests
Screening is the first step in determining if a man has prostate problems.
- Finger-rectal exam: This is done by touching the prostate gland through the anus.
- PSA (prostate-specific antigen): A blood sample is taken from a vein, and a substance made by the prostate is looked for and measured in the blood. The higher level is a sign of problems with the prostate, like inflammation, growth, or even cancer.
After the screening, the doctor decides if there is a need for more tests:
- Ultrasound scan: A probe is put into the rectum, which sends an image of the prostate gland to the doctor to determine the size, structures, and any abnormalities.
- MRI (magnetic resonance imaging) uses a magnetic field to get a clearer picture of the prostate.
- Biopsy (prostate tissue sampling): A thin needle is used to remove a small piece of tissue for a more accurate test in the lab to see if there are cancer cells.
- PET-CT (positron emission tomography) measures how organs and tissues work using a small amount of radioactive material, a special camera, and a computer. This method can find the start of a disease earlier than other methods because it looks for changes at the cellular level.
- PSMA PET-CT, or PSMA positron emission tomography, is a type of computed tomography that uses a radioactive material (68Ga-PSMA-11). This drug sticks to prostate cancer cells and helps find where they are. So, the method accurately tells whether a tumor or metastasis is present.
- For a bone scan (osteoscintigraphy), a radiopharmaceutical drug that gives off gamma radiation is injected into the body. A gamma camera is used to study how it is spread out. One of the most popular methods in nuclear medicine can find problems with how bones work, not changes in their structure.
Prostate cancer stages
They refer to the progression of the disease and determine the treatment options available.
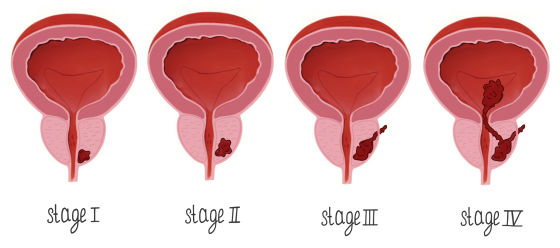
Based on tumor size, lymph nodes involved, and distant metastasis, prostate cancer is generally classified into four stages:
- Stage I: cancer is confined to the prostate and considered small and localized.
- Stage II: cancer is still confined to the prostate but is considered more significant.
- Stage III: malignant cells have spread outside the prostate and may involve nearby lymph nodes or tissues.
- Stage IV: Cancer has spread to distant organs or bones.
Where to go to treat?
 Prostate cancer treatment options
Prostate cancer treatment options
When the diagnosis has been verified, the next step is to choose the best treatment approach. It will vary from patient to patient based on the illness's stage and the patient's particular characteristics.
With a prostatectomy, the prostate gland is taken out by surgery. It is the best treatment for prostate cancer at its early stages. There are many different kinds of prostatectomies, such as:
- Radical prostatectomy is the most common type of surgical treatment. It involves taking out the whole prostate gland and some of the tissue around it.
- Laparoscopic prostatectomy is a less invasive version of radical prostatectomy. The prostate gland is removed through several small incisions and special tools.
- Transurethral resection of the prostate (TURP): removes a piece of the prostate gland through the urethra. It is used to treat an enlarged prostate.
Most of the time, the decision to have a prostatectomy is based on the cancer stage, the patient's health, and personal preferences. Prostatectomy can be a way to treat prostate cancer in its early stages.
Radiation therapy, also known as radiation, is a method of treating cancer that involves using various beams and accelerators to kill malignant cells. Utilizing it in the early stages, in combination with surgical treatment (either before or after surgery), and for local exposure to single metastases has proven effective.
Hormone treatment, or Androgen deprivation therapy (ADT), is a prostate cancer treatment that lowers androgen levels. Prostate cancer cells need androgens to grow. Oral, injectable, and implantable hormone treatments are available. Hormone therapy is often combined with radiation or surgery.
Chemotherapy is a drug-based therapy that kills cancer cells by stopping their growth and division. It is usually used as a treatment for prostate cancer metastasis. Oral and intravenous administration is possible.
Cryotherapy is a technique that uses shallow temperatures to kill cancer cells. The prostate gland is accessed by inserting a probe and introducing a cold gas (liquid nitrogen or argon). The cell is destroyed by freezing the cancerous tissue at temperatures ranging from -90 degrees Celsius to -150 degrees Celsius.
Immunotherapy is a treatment that uses medications to boost the body's immune system to kill cancer cells. It is often dosed and produced separately for each patient, depending on his specific needs.
Target therapy is a pharmacological treatment that targets specific cancer cells and inhibits the growth and spread of the disease at the molecular level. Concentrate on treating the disease while having as little of an effect as possible on healthy tissues.
What hospital to choose to treat prostate cancer?
 Newest prostate cancer treatment
Newest prostate cancer treatment
As mentioned above, prostate cancer is one of the most common oncology diseases. The American Cancer Society says that each year there are about 20 million new cases of prostate cancer and almost 10 million deaths from it. And according to data from A Cancer Journal for Clinicians, prostate cancer is the fourth most common type of cancer. It makes up 7.3% of all new cancer cases.
Scientists worldwide are trying to find better ways of alternative treatment for prostate cancer because it is so widespread. Here are some of the most creative ways to treat the disease:
- Prostate removal with the Da Vinci robot (Da Vinci robotic prostatectomy): a surgeon and a robot work together in an automated system. At the console, the doctor can see everything in 3D.
- Lutetium-177 therapy (Lu-177 PSMA therapy): Lutetium-177 is given through a vein and binds to cancer at the cellular level. At the same time, targeted radiation helps shrink tumors and is an effective treatment for metastatic prostate cancer.
- Actinium-225 therapy (also called Ac-225 PSMA therapy): Actinium-225, which contains radionuclides, is given through an IV. It spreads through the blood and sticks to cancer cells.
- Radium-223 therapy (Ra-223 PSMA therapy): a radioactive drug given through an IV that selectively binds to cancer cells and kills them by sending out radioactive particles.
- Proton therapy is a radiotherapy in which a beam of protons with a certain amount of radiation is sent straight to the affected area while avoiding nearby organs.
- Radio-guided surgery (PSMA-RGS surgery) is a new way to find lesions in people with recurring prostate malignancies. After the treatment, they can be removed more easily by surgery.
- High-intensity focused ultrasound (HIFU) is a type of focused ultrasound that kills cancer cells. It leads to malignant tissue death and kills cancer cells.
- Brachytherapy, also called "internal radiotherapy," involves injecting small granules that contain radiation directly into the organ that needs help. It goes straight to the tumor and has a minor effect on nearby organs.
- Radiosurgery (CyberKnife, GammaKnife) uses unique radiosurgical systems to remove tumors without surgery. They make it possible to take out the focus without taking out the whole organ.
Who treats prostate cancer the best?
 Prostate cancer stats and predictions
Prostate cancer stats and predictions
How long a person with cancer will live depends on how quickly it is found and how far it has spread. A five-year survival rate gives an idea of how cancer will turn out. The International Center for Cancer Research says that it is made up of the following:
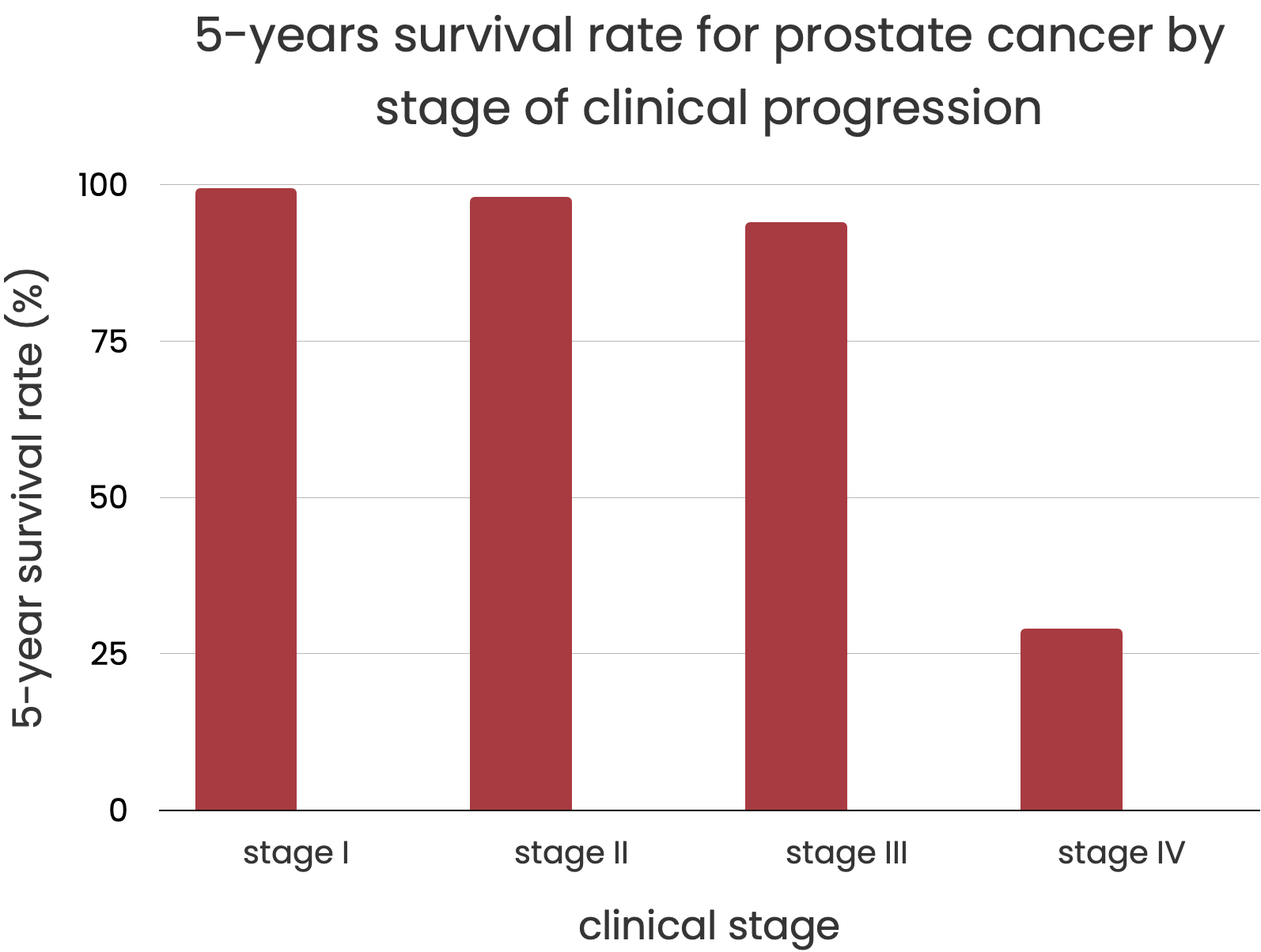
No matter how far along the disease is, there are statistics for people who have had a radical prostatectomy. For example, the survival rate after five years is 99%; after ten years, it's 98%; and after fifteen years, it's 96%. It is one of the best survival rates for cancers in general.
References:
- World Health Organization: Cancer
- A Cancer Journal for Clinicians: Global Cancer Statistics 2020
- ESMO (European Society for Medical Oncology): Clinical Practice Guidelines
- National Cancer Institute: PSMA PET-CT Accurately Detects Prostate Cancer Spread, Trial Shows
- RadiologyInfo: Positron Emission Tomography-Computed Tomography (PET/CT)
- UCSF (Department of Radiology & Biomedical Imaging): Prostate-Specific Membrane Antigen (PSMA) PET Imaging for Prostate Cancer
- American Cancer Society: Key statistics for prostate cancer

















