Personalized Theranostics in Occult Peritoneal Carcinomatosis from MINUTE Medical - Case Report
This remarkable clinical case from MINUTE Medical in Vienna demonstrates how a carefully selected arsenal of isotopes, guided by the latest clinical findings, paved the way to complete remission for a patient experiencing peritoneal carcinomatosis after a robot-assisted Da Vinci prostatectomy. While often surprising to patients, peritoneal carcinomatosis following robotic prostate surgery is actually not rare. It is partly a direct consequence of the surgical technique itself; the use of pneumoperitoneum combined with continuous intraoperative irrigation can inadvertently facilitate the dissemination of tumor cells deep into the most remote peritoneal recesses of the abdominal cavity.
Because prostate cancer typically grows at a very slow rate, these peritoneal metastases can remain clinically undetectable for years. Diagnostic challenges often arise even when PSA levels climb well above 1 ng/ml. Traditional PSMA PET-CT scans utilizing gallium-68 or fluorine-18 frequently reach their diagnostic limits in these scenarios. The metastatic lesions are simply too small, their PSMA expression is too low, and the physiologic background activity of surrounding normal tissue is too high to provide a clear picture. Consequently, after what is usually an unsuccessful course of local radiotherapy, many patients are placed on long-term antihormonal treatment. Unfortunately, this empirical approach can mask the underlying peritoneal carcinomatosis until the disease inevitably progresses to a castration-resistant stage.
In this specific case, however, the patient firmly declined empirical hormone therapy and insisted on discovering the exact cause behind his rising PSA. His self-advocacy led to the utilization of an advanced 89Zr-PSMA PET-CT scan. This study successfully detected tiny peritoneal lesions and confirmed their PSMA expression, a breakthrough enabled by the unique properties of zirconium-89. Compared to gallium-68, which has a short half-life of just 68 minutes, zirconium-89 boasts a much longer half-life of approximately 78 hours. This crucial difference allows delayed imaging up to several days after tracer injection. Over this extended period, the diagnostic radiopharmaceutical continues to accumulate in even the smallest or least PSMA-avid lesions, while naturally washing out of normal tissues. The result is dramatically reduced background activity and a much sharper diagnostic contrast.
Armed with these precise findings, the clinical team designed a highly modern theranostic treatment concept grounded in two recent studies: PSMAddition and VIOLET.
- The tailored approach began with a short antihormonal pretreatment using relugolix, strategically administered to increase the tumor's PSMA expression. Unlike classical GnRH agonists (such as leuprorelin), relugolix is a GnRH antagonist. This means it immediately lowers testosterone and entirely avoids the initial testosterone surge, or "flare effect." Furthermore, once relugolix is discontinued, testosterone levels recover rapidly, restricting disruptive side effects like fatigue and hot flashes to a very brief window.
- Following this priming phase, the patient underwent PSMA radioligand therapy utilizing a highly customized combination of radionuclides: a single treatment with terbium-161 and two treatments with lutetium-177. The inclusion of Tb-161 was a calculated decision, as it is particularly well-suited for targeting microscopic disease, including the micrometastases characteristic of peritoneal carcinomatosis.
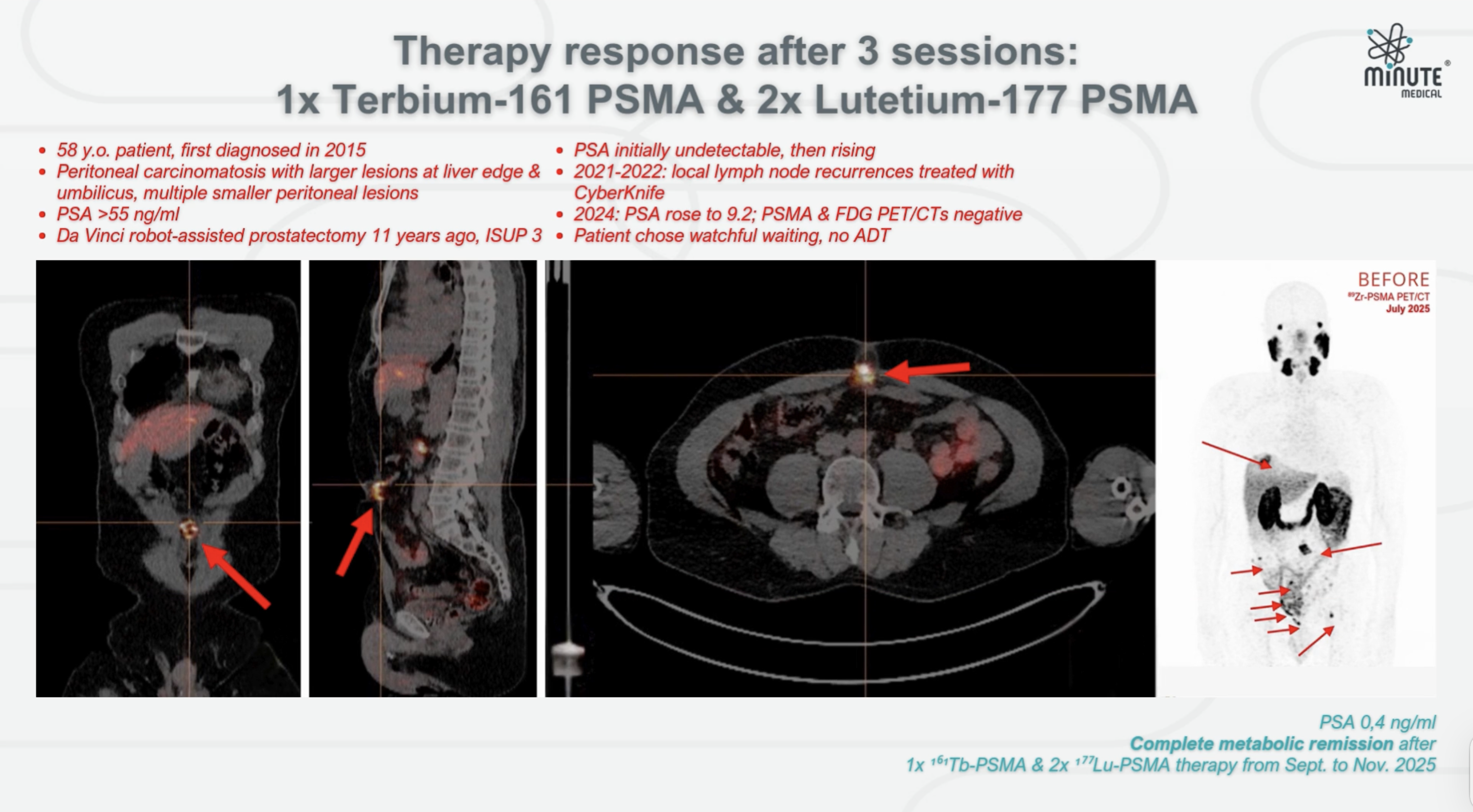

Today, the patient's outcome is excellent, allowing him to maintain a high quality of life. As of the end of January 2026, his PSA had plummeted to 0.4 ng/ml alongside fully recovered, normal testosterone levels. Most importantly, a follow-up 89Zr-PSMA PET/CT scan confirmed complete metabolic remission, validating the power of this highly personalized, isotope-driven approach.
