Thymus Cancer Guide

In the USA, only about 390 new cases of thymus cancer are discovered yearly.
Every two in three patients with thymus cancer are asymptomatic when diagnosed.
Patients with thymus cancer have 28% more chances of developing other types of cancer.
Thymus cancer represents 20% of all tumors in the mediastinum.
 Thymus anatomy and main functions
Thymus anatomy and main functions
Thymus is the main lymphoid organ of the human immune system. Inside that organ, T-cells grow and get ready to become mature. These cells are one of the main elements of the so-called adaptive immune system (it's part of the immune system that reacts to various factors of the environment, including bacteria and viruses) and play an essential role in creating "immunological memory."
Where is the organ located?
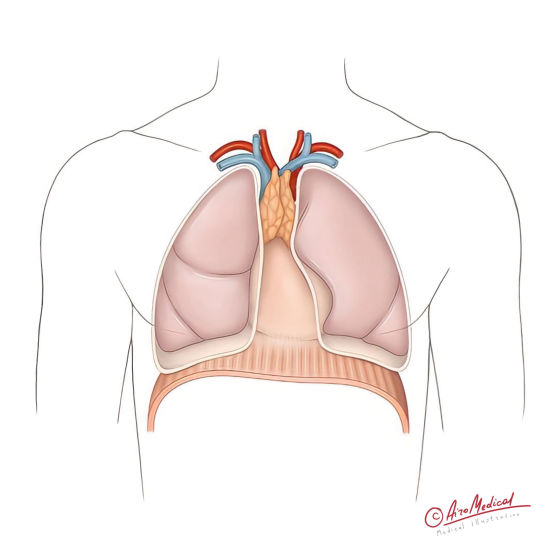 Thymus is located behind the sternum in the upper part of the chest, right in front of the heart. This part of the chest is also known as the mediastinum. After the human's birth, this organ is 5-6 cm long and weighs up to 60 g. Thymus increases in size until the human reaches puberty, and the "involution" process starts afterward. During "involution," the thymus slowly degenerates and decreases in size.
Thymus is located behind the sternum in the upper part of the chest, right in front of the heart. This part of the chest is also known as the mediastinum. After the human's birth, this organ is 5-6 cm long and weighs up to 60 g. Thymus increases in size until the human reaches puberty, and the "involution" process starts afterward. During "involution," the thymus slowly degenerates and decreases in size.
About thymus function
Thymus is much more important for youngsters and teenagers compared with adults. Still, even after the "involution," this organ plays a significant role in the work of the immune system. That's why performing a timely treatment of any thymus-related diseases is essential.
 Thymus cancer: What is it?
Thymus cancer: What is it?
Thymus cancer is a rare malignancy affecting about 0,13 people among every 100 000 of the population. The disease represents less than 1% of all human malignant tumors. Although T-cells originate from the thymus, it's not correct to call cancer of T-cells a thymus cancer. Instead, it's called lymphoma and primarily affects children. Thymus cancer rather mainly affects adults and is often called a thymoma.
Most thymomas show low or moderate malignant properties and don't show a significant tendency to develop metastases. For example, among US citizens with a thymus cancer diagnosis, only 8% tend to develop distant metastases.
Types of thymus cancer based on cellular specs
WHO (World Health Organization) developed a specific classification of thymomas depending on the histological presentation of certain cell forms. Those types of thymus cancer are the following:
- A type. A type of thymus cancer is set up when tumor cells have mostly fusiform or oval shapes. About 11% of all thymomas are A type.
- B type. Thymus cancer considering B type when most tumor cells have round or polygonal shapes. It's also divided into three subtypes: B1 type (shows up in about 17% of cases), B2 type (shows up in about 28% of cases), and B3 type (shows up in about 21% of cases).
- AB type. This thymus cancer shows up in 23% of cases and usually mixes features of both A and B types.
What do we know about metastatic thymus cancer?
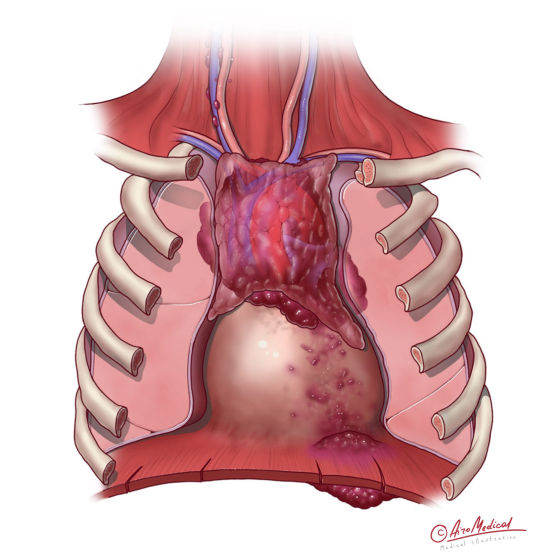 Metastatic thymus cancer, also called secondary thymic cancer, is also a pretty rare condition. Mostly, this fact is related to the specific anatomy and low blood distribution rates in the thymus of adults.
Metastatic thymus cancer, also called secondary thymic cancer, is also a pretty rare condition. Mostly, this fact is related to the specific anatomy and low blood distribution rates in the thymus of adults.
Among the most frequent primary tumor locations that show a tendency to cause metastatic lesions in the thymus are:
- Breast cancer (about 20% of cases)
- Digestive system tumors (about 13% of cases)
- Lung cancer (about 7% of cases)
When thymus cancer develops very fast and tends to expand aggressively, most oncologists call it thymic carcinoma. Luckily, only one of every five thymus tumors shows signs of carcinoma. In addition, only 0,06% of all thymic malignancies were verified as actual thymic carcinoma. Various variants of thymus neuroendocrine tumors also might be discovered occasionally.
 What causes thymus cancer?
What causes thymus cancer?
Nowadays, there is no universally recognized unified theory about a single cause of a tumor of the thymus. Still, doctors verified a few risk factors that might increase the probability of thymoma development.
Among the risk factors are the following
- Age. Thymus cancer tends to develop among older people, peaking among those aged 40-50. Still, cases among children and even more older people also might occur.
- Ethnicity and race. African Americans, Asians, and Pacific Islanders are more likely to develop thymus cancer than Caucasians.
- Certain immune diseases. There is a strong association between certain autoimmune diseases and thymus cancer. Among those diseases are myasthenia gravis (up to 15% of patients tend to develop thymus cancer), pure red cell aplasia (up to 5% of patients develops thymomas), and systemic lupus erythematosus (up to 2% of patients tend to develop thymus cancer).
Thymus cancer has no reported associations with any specific diet, nutrition factors, lifestyle, and habits. In addition, doctors didn't find any relation between thymomas and the impact of such factors as radiation exposure, professional harm, and the effect of chemicals. Still, a slight association with Epstein Barr Virus was suspected in some patients, but additional studies are required to confirm it.
How to prevent thymus cancer?
Unfortunately, it's impossible to prevent thymomas as oncologists don't know the exact reason for their occurrence. In addition, thymus cancer is not associated with any avoidable risk factors. That raises a question about the importance of regular check-ups to know if the patient is healthy and to understand the patient's current condition.
 Symptoms of thymus cancer
Symptoms of thymus cancer
Interestingly, about 66% of all patients with newly diagnosed thymus cancer showed no symptoms. In most cases, severe symptoms began to show up only in the advanced stages of the disease.
Common signs of the disease
Still, it's crucial to seek the help of medical practitioners if the patient shows any of the following signs:
- Cough. In some cases, a thymus tumor might press a trachea. As a result, the patient might have difficulty breathing and start coughing.
- Pressure in the chest or chest pain. Due to the pressure that the tumor might create on the nearby organs, pressure, and chest pain might show up. Patients with advanced stages of thymus cancer or giant tumors develop those symptoms.
- Phrenic nerve palsy. Thymus cancer might create pressure on the phrenic nerve, and as a result, palsy might occur. In that case, a patient will have additional breathing difficulties.
- Superior vena cava (SVC) syndrome. If the thymus cancer grows big enough, it might cause superior vena cava (SVC) syndrome. The tumor squeezes the superior vena cava (the big vein that delivers blood from the upper part of the body to the heart), and, as a result, the patient might get swelling, increased heart rate beat, and blueish skin.
- Paraneoplastic syndromes. Symptoms of thymic cancer include immune system reactions in 90% of cases, and a significant part of them are paraneoplastic syndromes. They have many endocrines, hematological and endocrine manifestations and can be very helpful in suspecting the tumor.
- Swollen thymus. Rarely, the patient's thymus might grow up and swell to the size when they can detect it in the mirror.
If a distant second opinion relevant to you?
As you can see, no specific symptoms can help oncologists understand possible thymic cancer without further examination. As a result, it's often possible for doctors to set an appropriate diagnosis that creates additional importance to getting a second opinion.
AiroMedical will gladly help you get all the information about the best medical practitioners in oncology, thoracic surgery, radiology, and other specialties to get the most extended and comprehensive multidisciplinary approach to future treatment and diagnosis.
 How do you know if you have thymus cancer?
How do you know if you have thymus cancer?
Due to a frequent lack of symptoms, the tumor becomes an accidental finding in about 30% of all thymus cancer cases. Usually, these tumors become an incidental finding during an X-ray chest examination. Mostly, X-ray results are not a direct confirmation of the illness. Still, many ways exist to detect and confirm thymus cancer with significant certainty.
Imaging diagnostic
- X-ray imaging. More than 80% of thymomas are obvious on the chest x-ray. Still, no specific way exists to confirm that it's thymus cancer and not some other pathology via x-ray.
- CT scan might help get a more profound understanding of thymus cancer's nature, for example, to know more about the size and condition of the nearest organs. More than 90% of thymomas are visible during CT, and about 98% are visible during CT with contrast. Still, there is a significant chance of becoming misdiagnosed when using CT only.
- MRI scan. It shows similar efficiency in detecting thymus cancer as CT but still can't be used to verify the histological type of tumor and some other features. Modern MRI shows up to 87% of sensitivity when detecting thymus tumors.
- PET and PET/CT. Radiologists inject a small portion of a specific substance absorbed mainly by cancer cells in the patient's vein and scan the whole body. This method is extremely valuable in detecting distant metastases.
Biopsy (tissue sampling)
A biopsy is the only method that helps to verify thymus cancer with nearly 100% efficiency. Oncologists examine a small portion of the tumor via the microscope and get more information about its various features. Still, primarily, a biopsy might be performed only after detecting a primary tumor or metastatic lesion via other methods.
Additional diagnostic tools
Other methods, like lab blood tests (whole blood count, chemistry panels, etc.), might be helpful to know more about the patient's condition and general health. Still, unfortunately, they can't help to verify thymus cancer. However, the results of those lab tests can significantly impact future treatment plans and influence doctors' decisions.
Thymus cancer stages
There are at least a few thymoma staging systems, including the Masaoka-Koga classification. Still, the TNM staging system remains the most versatile and widely used classification that helps better understand how bad thymus cancer is in particular cases. TNM system is based on the condition of the primary tumor (T), including size, volume, etc., the state of lymphatic nodes (N), and the appearance of distant metastases (M). About 80% of all metastatic cases didn't spread further than the patients' chest.
According to the TNM staging system, thymus cancer has four stages based on the abovementioned factors. For example, stage 4 thymus cancer might show any features of a primary tumor, including small size but distant metastases or/and significant involvement of lymphatic nodes, will be presented. Also, thymus cancer has stages IVA and IVB, which oncologists introduce to separate cases with pericardial and pleural metastases and cases with distant metastases.
The best countries to treat thymus cancer
 What is the treatment for thymus cancer?
What is the treatment for thymus cancer?
Thymus cancer especially detected in the early stages show a remarkable tendency to be successfully treated. Only 31% of patients might develop metastases or recurrence after the first treatment. Interestingly, most patients who got a relapse or developed metastatic lesions were remarkably younger than those who didn't.
Treatment methods for thymus cancer
Thymus removal surgery
To remove thymus cancer, thoracic surgeons need to perform a thoracotomy (the cut on the chest) first. After that, the medical practitioner removes the thymus and all surrounding tissues involved. This is the best treatment method for early-stage thymus cancer. Also, only 1% of patients with stage 1 thymus cancer who undergo thymus removal surgery experience relapses in the future.
Chemotherapy
A combination of various medications is believed to be the most effective method of chemotherapy for patients with thymus cancer. Chemotherapy that includes four drugs shows a 91,8% response rate among patients with stages 3 and 4 of invasive thymoma. It is an excellent method for patients with advanced stages of tumor and those who experience relapse.
Immunotherapy
In some cases, oncologists consider activating patients' immune systems to fight thymus tumors. But unfortunately, immune therapy is a bad option for patients with severe paraneoplastic syndromes. Still, some methods (e.g., immune checkpoint inhibitors) show promising results and about a 30% response rate in patients with severe thymic cancer.
Targeted therapy
The main goal of targeted therapy is to influence substances, genes, or other factors essential for the further growth and development of thymus cancer. This is one of the most essential thymus cancer treatment methods for patients with numerous relapses and severe metastases. For example, IMC-A12 (Cixutumumab) showed a 10% reduction in primary tumor size in patients with metastatic thymus cancer.
Radiotherapy
Radiation therapy for thymus cancer is mainly used as adjuvant therapy (it's part of the treatment given after the primary treatment to lower the risk of relapses). In most cases, doctors prefer to use external beam radiation therapy (EBRT). About 77% of patients reported that radiation therapy helped them to achieve local control over the tumor after the surgery.
More about the combined approach
Combined therapy is a standard thymus cancer treatment method, especially for patients with many distant metastases. Combined therapy might include any of the abovementioned methods depending on the patient's condition. To pick the most suitable components of combined therapy, oncologists must often carefully evaluate the patient's condition and avoid those methods that can potentially bring more complications than benefits, considering the patient's current state.
Certified thymus cancer treatment centers
 New and advanced methods of thymus cancer treatment
New and advanced methods of thymus cancer treatment
Some methods of thymus cancer treatment are more suitable for particular cases (e.g., massive or numerous pleural metastatic lesions), and others still need to be approved worldwide. As a result, it's possible to get new and advanced thymus cancer treatment abroad or in some particular clinics.
Latest treatment options
AiroMedical has a database that includes many reliable hospitals and clinics worldwide that can offer patients new and advanced methods of thymus cancer treatment. Among those methods, for example, are the following:
Robotic-assisted thymus removal
Surgeons might use robotic-assisted systems (for example, da Vinci systems) during thymus removal to achieve precise movements and avoid unnecessary damage. As a result, the probability of adverse effects significantly decreases. For example, only 5% of patients who undergo robotic-assisted thymus removal about any complications.
Brachytherapy (radioactive seeds)
Doctors put a small source of radioactive exposure inside the tumor during brachytherapy. For patients with thymus cancer, brachytherapy might often become a procedure to decrease the primary tumor's stage and proceed with surgical removal.
Tumor ablation
During ablation, patients with thymus cancer experience the local influence of various physical factors (high or low temperature, radiofrequency, electric field, etc.) to destroy a tumor. For example, 90% of patients with stage I thymoma achieved satisfactory results after radiofrequency ablation.
Radiosurgery
Radiosurgery is the most advanced type of radiotherapy that helps avoid unnecessary damage to the tissues surrounding the tumor. CyberKnife is believed to be among the most effective and adverse effects-free radiosurgery methods. Up to 96% of patients with stages 3 and 4 of thymus carcinoma who undergo treatment with CyberKnife pass the five-year overall survival rate.
Transarterial chemoembolization (TACE)
During transarterial chemoembolization, interventional radiologists insert a tiny tube via blood vessels until they reach a tumor. After that, doctors inject a portion of chemical substances via the tube that will help create an obstacle for blood flow inside cancer.
Cryotherapy
Most often, during cryotherapy, oncologists use various methods to create a necessary impact of low temperatures on a tumor's tissues to destroy them and avoid further growth and development. As a result, up to 90% of thymus cancer lesions removed with cryotherapy show no recurrence potential.
Hyperthermic Intrathoracic Chemotherapy (HITHOC)
Hyperthermic intrathoracic chemotherapy is a valuable method for patients with thymus cancer that spreads across the chest or peritoneum and is used as an additional part of the surgery. After removing the primary tumor, surgeons add an inside chest solution, slowly heat it to 38-39 C°, and insert a device that spreads a portion of the chemotherapeutic medication. More than 80% of patients who undergo HITHOC in addition to surgery achieved 5-year survival rates.
Infiltrating lymphocytes therapy (TIL)
Scientists find out that patients' lymphocytes that surround tumors create an especially significant anti-tumor effect. To boost this effect, they gather these lymphocytes and artificially enhance them in the laboratory. After that, these lymphocytes injects back into the patient. Patients with aggressive thymus cancer of 3 and 4 stages show up to a 28,6% response rate after infiltrating lymphocyte therapy (TIL).
CAR T-cell therapy
CAR T-cell therapy is another method of immune therapy that helps activate and increase the number of T-cells to help the patient's immune system fight cancer. Oncologists take a portion of the patient's blood, gather T-cells, and then grow them in the laboratory. Ultimately, they inject T-cells back into the patient's blood vessels. Lab tests show that about 79% of thymus cancer cases might give a positive reaction after CAR T-cell therapy.
Also, many different new and advanced methods of thymus cancer treatment are undergoing various stages of clinical trials right now. In some cases, it's still possible to become a part of these trials and help doctors evaluate the efficiency of treatment and receive an additional chance to overcome thymus cancer. AiroMedical can easily help patients find the above-mentioned opportunities and check if their cases are eligible for clinical trials.
Doctors who specialized in thymus cancer treatment
 Thymus cancer statistics
Thymus cancer statistics
The thymus cancer survival rate is mainly related to the histological type of the tumor and the stage. However, other factors, like age, other diseases, and the patient's current condition, also play some role.
The survival rate by stage
Here is a graph that showcases the relationship between the stage of thymus cancer and the five-year survival rate:
- I stage - 92,8%
- II stage - 89,3%
- III stage - 71,6%
- IV stage - 25,9 - 31,2%
What is the prognosis without treatment?
In any case, the importance of adequate and timely treatment is evident. For example, the five-year survival rate of patients who didn't complete treatment and was diagnosed with thymus cancer is only 50%.
That's why the AiroMedical team carefully gathered all information about all available methods of thymus cancer treatment, the best doctors, and hospitals where you can get the necessary help. So don't hesitate to press the contact us button and share the information about your case to get the best possible and most suitable treatment options worldwide.
References:
- Rajan A, Giaccone G. Treatment of advanced thymoma and thymic carcinoma. Curr Treat Options Oncol. 2008;9(4-6):277-287. doi:10.1007/s11864-009-0083-7
- Engels EA. Epidemiology of thymoma and associated malignancies. J Thorac Oncol. 2010;5(10 Suppl 4):S260-S265. doi:10.1097/JTO.0b013e3181f1f62d
- Weis CA, Yao X, Deng Y, et al. The impact of thymoma histotype on prognosis in a worldwide database. J Thorac Oncol. 2015;10(2):367-372. doi:10.1097/JTO.0000000000000393
- Minervini F, Kocher GJ. When to suspect a thymoma: clinical point of view. J Thorac Dis. 2020;12(12):7613-7618. doi:10.21037/jtd-2019-thym-05
- Wei ML, Kang D, Gu L, Qiu M, Zhengyin L, Mu Y. Chemotherapy for thymic carcinoma and advanced thymoma in adults. Cochrane Database Syst Rev. 2013;2013(8):CD008588. Published 2013 Aug 23. doi:10.1002/14651858.CD008588.pub2
- Markowiak T, Hofmann HS, Ried M. Classification and staging of thymoma. J Thorac Dis. 2020;12(12):7607-7612. doi:10.21037/jtd-2019-thym-01