Neurofibromatosis (NF) Guide

About 96% of all confirmed neurofibromatosis cases worldwide are represented by neurofibromatosis type 1.
On average, only one human out of 25,000 got a neurofibromatosis type 2.
About 0,3% of affected patients are not developing a single symptom but still can pass this condition to their offspring.
The most giant tumor removed from the patient with NF was reported to weigh nearly 110 kg (242 lb).
 What is neuroglia?
What is neuroglia?
Neuroglia includes many different cell types (excluding neurons) that are a part of the central and peripheral nervous systems. Neuroglia cells generally comprise about 50% of all nervous system cells. These cells cannot create and conduct electrical impulses but have numerous other vital functions.
Functions of the cells
Among them are the following:
- Creating a cover for neurons
- Separating neurons and nerve fibers
- Destroying different particles and infectious agents
- Supplying neurons with oxygen and various nutrients
- Holding nerves and structures in a stable position
- Destroying dead neurons
Neuroglia cells also participate in the process of neuron connection and creating neurotransmitters (specific substances necessary for conducting nervous impulses). Most neuroglia cells develop along with other parts of the nervous system. Therefore, various neurological diseases might arise in case of any developmental issues or dysfunctions of the neuroglia.
 What is neurofibromatosis?
What is neurofibromatosis?
 Neurofibromatosis is a collective name for several conditions associated with increased risk of nervous tissue tumor development. In most cases, patients with neurofibromatosis have numerous tumors that primarily arise from the neuroglia and much more rarely from the neurons.
Neurofibromatosis is a collective name for several conditions associated with increased risk of nervous tissue tumor development. In most cases, patients with neurofibromatosis have numerous tumors that primarily arise from the neuroglia and much more rarely from the neurons.
Fortunately, only 3-5% of these tumors might become malignant during the disease. The leading causes of neurofibromatosis are related to genetic mutations of specific genes, which vary depending on the particular type of the disease.
The leading cause of NF is a hereditary transmission of the defective gene from parents to offspring. Still, in about 50% of cases, the spontaneous mutation might occur at an early age (usually before 1 year old). So, the answer to the question, “Is neurofibromatosis a genetic disorder?” is 100% positive.
Types of neurofibromatosis
The modern classification of NF includes:
- NF type 1. The most widespread kind of neurofibromatosis, and about 1 in 3000 people have the risk of developing it.
- NF type 2. This type of NF represents only 3% of all cases, and only 1 in 25 000 people potentially get it.
- Schwannomatosis. Schwannomatosis is rarely called neurofibromatosis type 3 and often has some clinical similarities with NF type 2. It is one of the rarest NF types that affects only 1 in 1 700 00 patients.
Interestingly, the number and variety of genetic mutations that lead to neurofibromatosis have increased, making a genetic test less reliable and improving the diagnostic value of general medical examination. That's why regular medical check-ups in trustworthy clinics and hospitals are essential.
Neurofibromatosis type 1 vs. type 2
NF type 1 is mainly related to mutations in the so-called "NF1" gene located on chromosome 17, and NF type 2 is most often associated with mutation of the "NF2" gene of chromosome 22. Also, up to 50% of patients with NF type 1 disease have no family history of neurofibromatosis, while 93% of patients with NF type 2 have a previous family history of the disease. Both types of disease lead to tumors originating from nerve tissue cells.
The main difference between neurofibromatosis 1 and 2 is in the number and the location of tumors. Neurofibromas (tumors originating from a mix of various neuroglia cells) mainly occur in patients with NF type 1 and can be located all around the whole body. On the other hand, vestibular schwannomas (tumors originating from Schwann cells located near the base of the brain) and meningiomas (tumors arising from meningeal cells) are the main diagnostic criteria of NF type 2.
 Causes and NF prevention
Causes and NF prevention
Primary risk factors of neurofibromatosis
Nowadays, scientists and doctors don't find evidence that neurofibromatosis might be related to race, sex, ethnicity, lifestyle, and other factors. In most cases, mutations that cause NF occur spontaneously or are inherited. Also, there is no available information about potential factors that might increase the probability of spontaneous mutations.
Prevention of neurofibromatosis
Neurofibromatosis has not been associated with any kind of potentially preventable risk factors. As a result, there is no way to prevent neurofibromatosis for now except by carefully analyzing the family history of both partners before getting a child.
 Neurofibromatosis symptoms
Neurofibromatosis symptoms
Three primary forms of neurofibromatosis often share similar symptoms. However, most symptoms occur due to non-specific factors, e.g., pain due to the pressure of a tumor mass on the nerve or hearing loss for the same reason.
Also, various tumors might appear regardless of NF type. For example, schwannomas are one of the main signs of Schwannomatosis. However, up to 70% of patients with NF type 2 develop these tumors. Still, the number, cite, and kind of developed tumors help determine the exact pathology type in a particular case.
There is a neurofibromatosis cancer malignancy occurrence risk that highly varies depending on the type of primary diagnosis and tumor type. For example, 8-13% of patients with neurofibromatosis type 1 who developed neurofibromas show a risk of degrading into malignant peripheral nerve sheath tumors (MPNST). MPNST often indicates a tendency to create early metastases and considers highly dangerous tumors that significantly decrease the life expectancy of patients.
Signs of neurofibromatosis type 1
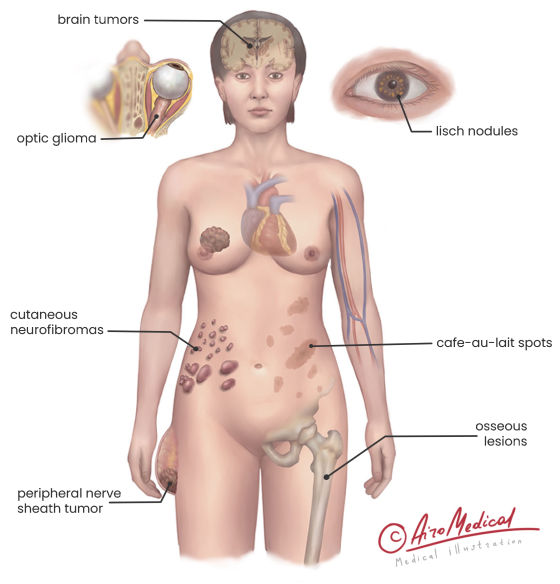
- Café-au-lait spots. These are brown, non-malignant spots that can occur anywhere on the body. Before the age of 1 year, up to 99% of patients with neurofibromatosis type 1 develop at least six café-au-lait spots greater than 5 mm.
- Neurofibromas. Neurofibromas are benign tumors often located on or under the skin surface. Still, they might be presented anywhere in the body. Some recent research on neurofibromatosis shows that up to 60% of patients with neurofibromatosis type 1 develop at least one big neurofibroma during the disease.
- Freckling on armpits. Over 90% of patients with NF type 1 develop freckling on armpits before age seven. However, they mostly remain asymptomatic and don't cause any trouble to patients.
- Lisch nodules. Lisch nodules are specific benign tumors on the iris and mostly could be found in adults. They mainly don't cause any additional issues and remain benign. About 95% of patients with NF type 1 develop such nodules.
- Optic nerve gliomas. Optic nerve gliomas are tumors that arise from the optic nerve and often result in various problems with vision, including rare cases of blindness. Up to 15% of patients with NF type 1 have optic nerve gliomas.
Primary symptoms of neurofibromatosis type 2
- Vestibular schwannomas. Vestibular schwannomas (on both sides or one side) are brain tumors that often cause hearing problems. About 95% of patients with NF type 2 develop bilateral (on both sides of the brain) vestibular schwannomas.
- Meningiomas. Meningiomas are the second of the most widespread tumors among patients with NF type 2 and are presented in about 50% of cases and are associated with increased mortality.
- Ependymomas. These are the tumors of the spinal cord, and up to 58% of patients with NF type 2 develop multiple ependymomas. Often, they might remain asymptomatic.
Symptoms of schwannomatosis
- Schwannomas. The leading type of tumor that occurs in patients with schwannomatosis is schwannomas. They might be located all around the body and often cause chronic pain. About 89% of patients with schwannomatosis develop peripheral schwannomas.
- Meningiomas. These tumors develop in the brain and spinal cord of patients with schwannomatosis. Only about 5% of patient with schwannomatosis develops multiple meningiomas.
 How is neurofibromatosis diagnosed?
How is neurofibromatosis diagnosed?
As every type of neurofibromatosis is related to the development of tumors, it often might be difficult to distinguish it and set a proper diagnosis.
Primarily, diagnosis is based on the results of an examination by oncologists. Still, additional tests and medical procedures might be required to confirm the diagnosis.
Primary tests
Here are some of the most useful methods that help to verify the diagnosis:
- MRI and CT These methods can help to get images of the patient's brain and spinal cord to confirm a diagnosis of NF type 2 or schwannomatosis.
- Biopsy. Biopsy remains the most effective method that helps to know more about tumors' features with nearly 100% accuracy. Surgeons remove a small piece of a tumor without entirely removing it and then examine them under the microscope.
- Genetic screening. Genetic screening tests are not widely spread, but sometimes it's essential to undergo these for early or prenatal (before the birth of the baby) diagnostics. It also helps to distinguish different types of neurofibromatosis.
General examinations
Before starting further treatment, it’s necessary to undergo additional general lab and clinical examinations. Their number and specific list might vary depending on the type of neurofibromatosis, type of tumor, and severity of the condition. Mainly, they include whole blood count, biochemical blood test, and evaluation of kidneys’ and hepatic functions.
Also, before surgery, the patient should take some tests to help evaluate possible changes in bleeding. All these tests will help doctors to develop the most suitable and safe treatment plan.
Countries with the best treatment for NF
 Neurofibromatosis treatment options
Neurofibromatosis treatment options
Unfortunately, there are no specific treatment methods for neurofibromatosis nowadays. Still, modern medicine creates many ways that can help improve the quality of life for patients with these diseases.
Mainly, they can help remove various symptoms due to tumor growth. For example, patients with NF type 2 who got vestibular schwannomas and didn't receive proper treatment show a 16% hearing decline during three years of observation. So, treating tumors that create additional issues remains essential so patients can live more comfortably. Here are the primary treatment methods:
Surgery for neurofibromatosis
Surgical removal
Most superficial tumors related to neurofibromatosis can be removed during surgery. About 74,4% of patients who undergo surgery reported improvement in their condition. Surgical removal is one of the most widespread methods of management and treatment for neurofibromatosis type 1-related tumors.
Laparoscopic surgery
Surgeons might use laparoscopic surgery for neurofibromatosis tumors if they are located inside the body. Unfortunately, laparoscopic surgery can be helpful mainly for tumors less than 2 cm in diameter, often making it useless for patients with this disease.
Treatment to shrink tumors
Chemotherapy
Chemotherapy considering a good treatment option for malignant tumors with metastasis or tumors that can't be removed during surgery immediately. Statistically, up to 75% of patients show a decrease in tumor sizes, allowing them to undergo further surgery.
Immunotherapy
The main goal of immunotherapy is to restore and enhance the immune response and increase the ability to fight tumor growth. Many immunotherapy methods are already used, and numerous currently undergo clinical trials. For example, PegIFN-α2b (laboratory-enchased human protein) helped patients decrease tumor volume by 10-22%.
Targeted therapy
Targeted treatment aims to interrupt the supply of vital substances to decrease the ability of tumors to grow and develop. Currently, lots of options exist for various types of neurofibromatosis tumors. For example, epidermal growth factor receptor (EGFR) and Erb2 inhibitors helped to decrease the volume of vestibular schwannomas by 15.7–23.9% during nine months of treatment for neurofibromatosis type 2.
Radiotherapy
Radiation is currently used as a method of adjuvant therapy (in addition to surgery methods) in most cases and helps improve the results of the primary treatment. Currently, oncologists often use chemotherapy and radiation therapy to increase the response of tumors to radiation therapy.
It's important to understand that methods of treating neurofibromatosis might vary depending on the type of tumors, their number, size, and many other features. Also, getting as much information about the patient's condition is essential. As a result, before starting any treatment, it's vital to undergo a full medical check-up and get an appointment with various medical practitioners, including genetics, oncologists, dermatologists, and more.
AiroMedical gathered a database of the most skillful and experienced doctors that treat neurofibromatosis. So don't hesitate to contact us and get all the information regarding available treatment and diagnostic options.
Best neurofibromatosis clinics
 New treatments for neurofibromatosis
New treatments for neurofibromatosis
Unfortunately, no effective methods can guarantee full recovery from any neurofibromatosis. So, nowadays, the question "Is there a cure for neurofibromatosis?" have a negative answer. Still, a few promising modern methods might help decrease the volume and number of multiple lesions and slow down the growth of all tumors. Among these methods are:
Latest medications for NF
Koselugo (Selumetinib)
FDA approved this drug as the primary neurofibromatosis medication for children older than two years and adults. Up to 71% of patients with neurofibromatosis type 1-related neurofibromas show a decrease in tumor sizes by more than 20%. Other types of tumors also show decent treatment responses. Selumetinib also undergoes clinical trials as a medication for neurofibromatosis type 2.
Bevacizumab
Bevacizumab is a ligand-targeting drug that helps to achieve up to 50% of tumor volume shrinking among patients with NF type 2-associated vestibular schwannomas. Some patients also achieved a 15-30% improvement in hearing. Unfortunately, these effects might be achieved only in the case of prolonged treatment (more than nine months in a row), which is only sometimes possible due to the toxical impacts.
Gene therapy
Gene therapy neurofibromatosis methods are still being developed, and nowadays, it's impossible to treat these diseases by replacing the whole defective gene with a fully functional one. Still, some technologies like CRISPR/Cas9 show great potential in replacing some parts of the dysfunctioning gene. Still, these methods are not widely available due to a deficiency of clinical data.
Fractionated stereotactic radiation therapy (FSRT)
Primarily, fractionated stereotactic radiation therapy uses to treat those tumors that are hard or impossible to reach during traditional surgery. Instead, patients receive a dosage of radiation exposure that damages the tumor and prevents them from further growth. CyberKnife is one of the most modern apparatuses that might help to perform FSRT and stereotactic surgery (SRS). Among patients with vestibular schwannomas who undergo FSRT, up to 97% reach a 5-year progression-free rate.
New robotic-assisted surgery
Nowadays, robotic-assisted surgery is mainly used to treat schwannomas and malignant peripheral nerve sheath tumors of the pelvic and abdominal area. Compared to traditional open surgeries, robotic-assisted surgeries are traditionally associated with lower blood loss in patients (87.4 vs. 3889 mL), faster recovery after surgery (3,4 vs. 6 days), and other clinical benefits. Most definitely, this surgery method will develop further as a treatment of neurofibromatosis-related tumors of different localizations.
Alternative methods of drug delivery
In some cases, due to physiological and anatomical features, tumors might receive an insufficient concentration of drugs. As a result, oncologists have to use greater dosages that might lead to boosted toxic effects.
Alternative drug delivery methods can help deliver medications right into the tumor and significantly increase the efficiency of chemotherapy, immune therapy, and targeted therapy. For example, providing medicines for vestibular schwannomas via the oval window (a membrane that separates the inner ear from the middle ear) helps to improve the treatment efficiency up to 2-3 times. Still, it might be associated with adverse effects, including cerebrospinal fluid leaks.
Much more methods are being developed by medical practitioners all around the globe and could bring the cure to patients with NF. Some of them are still undergoing clinical trials and might require additional participants. AiroMedical might help people with neurofibromatosis to become a part of these trials and try some newly created treatment options.
Top neurofibromatosis doctors
 Statistic and life expectancy of NF
Statistic and life expectancy of NF
Unfortunately, the prognosis for patients with neurofibromatosis is pretty poor. Only a small number of patients didn't develop tumors and might not require any potential treatment. Also, neurofibromatosis is often associated with many other diseases, including 60-81% of cases with specific partial performance deficits (inability to count, read, etc.) and an attention deficit disorder (ADHD).
Also, about 11% of kids with neurofibromatosis develop conditions of the autism spectrum. As a result, these patients often might require a specific approach to the educational process and treatment. Some countries created neurofibromatosis treatment centers where these kids can get proper treatment with specially trained medical practitioners.
Prognosis of neurofibromatosis
Life expectancy for patients with neurofibromatosis highly varies depending on the severity of the disease. Also, patients with tumors that developed malignant properties often have shorter life expectancies than those without malignancies. Still, even in these cases, everything depends on the treatment process results and many other factors. Unfortunately, the average life expectancy of patients with neurofibromatosis is significantly shorter than among the general population. Take a look at the graph to get a better idea.
Life expectancy on the chart
The average life expectancy of patients with different types of neurofibromatosis compared to the mean age of death in the USA
- The mean age of death among the US population - is 76,4 years
- The mean age of death among patients with NF type 1 - is 54,4 years
- The mean age of death among patients with NF type 2 - is 62 years
- The mean age of death among patients with schwannomatosis - is 70 years
The main idea that will help patients with neurofibromatosis increase their life expectancy is to be patient with their condition and seek medical help in case of any deterioration. Still, some patients with these diseases are not well enough socially adapted, so in some cases, it's necessary to look for specific therapy and trained medical practitioners who can teach them how to live a longer and happier life with their condition.
AiroMedical might provide all necessary information regarding doctors, clinics, and hospitals created specifically for neurofibromatosis patients.
References:
- Farschtschi S, Mautner VF, McLean ACL, Schulz A, Friedrich RE, Rosahl SK. The Neurofibromatoses. Dtsch Arztebl Int. 2020;117(20):354-360. doi:10.3238/arztebl.2020.0354
- Kresak JL, Walsh M. Neurofibromatosis: A Review of NF1, NF2, and Schwannomatosis. J Pediatr Genet. 2016;5(2):98-104. doi:10.1055/s-0036-1579766
- Tamura R. Current Understanding of Neurofibromatosis Type 1, 2, and Schwannomatosis. Int J Mol Sci. 2021;22(11):5850. Published 2021 May 29. doi:10.3390/ijms22115850
- Farschtschi S, Mautner VF, McLean ACL, Schulz A, Friedrich RE, Rosahl SK. The Neurofibromatoses. Dtsch Arztebl Int. 2020;117(20):354-360. doi:10.3238/arztebl.2020.0354
- Gross AM, Wolters PL, Dombi E, et al. Selumetinib in Children with Inoperable Plexiform Neurofibromas [published correction appears in N Engl J Med. 2020 Sep 24;383(13):1290]. N Engl J Med. 2020;382(15):1430-1442. doi:10.1056/NEJMoa1912735

















