What is Better Actinium, Radium or Lutetium for Prostate Cancer?
New PSMA treatment options for prostate cancer
Men with prostate cancer have many ways to get treatment, such as surgery, radiation therapy, chemotherapy, hormonal therapy, and immunotherapy. When androgens, which are male sex hormones, move through the bloodstream, they can make prostate cancer grow. One type of prostate cancer treatment lowers the level of androgens in the body or stops them from doing their job. Even with these treatments, some prostate cancers keep getting worse. Castration-resistant prostate cancer is the name for this type of cancer (CRPC).
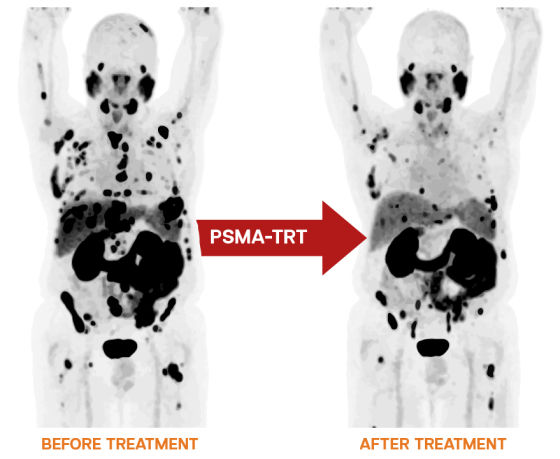 A new way to treat prostate cancer could save many men's lives and improve their quality of life. When the FDA (Food and Drug Administration) approved a new PSMA therapy, the number of people who could get better went up quickly.
A new way to treat prostate cancer could save many men's lives and improve their quality of life. When the FDA (Food and Drug Administration) approved a new PSMA therapy, the number of people who could get better went up quickly.
PSMA (Prostate-specific membrane antigen) is a protein that is attached to the cell surface of the prostate's epithelial cells. It is made in small amounts by a healthy gland but in significant quantities by a cancerous gland. So, PSMA is the perfect target for therapy to kill cancer cells, both primary tumors and metastases. Because they can bind to this protein and send radiation doses to cancer cells, radiopharmaceuticals are a unique way to treat cancer.
Radioligands send beta-particle radiation to the cancerous cells, which is how prostate cancer is treated. Different radionuclides are used for these things:
- Lutetium-177 PSMA therapy is based on the notion that Lu-177 can stick to the surface of the cell membranes that make PSMA. Lutathera and Pluvicto, two drugs with lutetium, were the first to get FDA approval. Radiologists can use it if the tumor has spread to other body parts and isn't responding to chemo or hormone therapy.
- Radium-223 dichloride, Xofigo, is used to treat advanced prostate cancer metastasizing to the bones. Radium's structure is also similar to that of Calcium, which is the main element in bone tissue. This similarity makes it easier for Ra-223 to get into bone metastases and kill cancer cells. Since there are no cancerous cells in the internal organs, this radioligand is given.
- Actinium-225 PSMA therapy is a novel radioligand-based approach to treating cancerous tumors. The medication molecule can bind to the protein in the same way that Lutetium can. It is used in place of Lutathera in cases where the latter medication is ineffective against prostate cancer.
Patients treated with beta and alpha radionuclide treatment employing PSMA labeled with radioactive elements have shown some encouraging results, as has been described. Patients with advanced cancer now have new treatment options, improving their chances of survival and quality of life.
What differentiates one method from another?
It is essential to have an understanding of the potential differences between the various types of treatments for metastatic prostate cancer, which include the following:
- the physical characteristics of the source of radiopharmaceuticals;
- the radiation radius of surrounding tissues;
- the half-life of the radionuclide;
- the efficacy of binding to tumor receptors.
Let's look at the details:
The most short-lived, Lutetium-177
 The half-life of radioactive Lu-177 is 6.5 days. 100–200 cells are in the distance of the radiation. Beta radiation is given off by lutetium.
The half-life of radioactive Lu-177 is 6.5 days. 100–200 cells are in the distance of the radiation. Beta radiation is given off by lutetium.
The most precise, Actinium-225
 Actinium has a half-life of 10 days, and its radiation can only reach 1-2 cells around it (alpha radiation).
Actinium has a half-life of 10 days, and its radiation can only reach 1-2 cells around it (alpha radiation).
The most bone-related, Radium-223
 The Ra-223 has a half-life of 11.5 days. The type of radiation used is natural alpha radiation, which affects 2–10 nearby cells. Primary bone metastases are the reason to use Ra-223 therapy.
The Ra-223 has a half-life of 11.5 days. The type of radiation used is natural alpha radiation, which affects 2–10 nearby cells. Primary bone metastases are the reason to use Ra-223 therapy.
As we can see, the effects of Actinium-225 and Radium-223 last longer, and their radiation range is smaller. When there is no answer to Lu-177 therapy, these radionuclides can help.
What about clinical results for metastatic prostate cancer?
Here we’ve compared the promising results of radioligand treatment.
The results of many clinical trials show the efficiency of Lu-177 treatment:
- Increasing the 5-year survival rate by 30%;
- Decreasing the risk of recurrence;
- Improving the quality of life in 70% of patients.
The investigations in Ac-225 efficacy presented:
- Lowering levels of an indicator of prostate cancer PSA in 80% of patients;
- Decreasing of 50-80% of metastases;
- Increasing the life expectancy.
The studies in Ra-223 showed:
- Increasing average survival;
- Decreasing risks of death by 30%;
- Reducing pain and making the life quality higher.
We can say that the Lutetium-177, Actinium-225, and Radium-223 therapy significantly improve prostate cancer patients' condition. It makes a longer life expectancy because it is successful and does not cause significant harm.
Which one of the targeted treatments is safer?
Targeted therapy is not toxic because it binds directly to the cell membranes. Actinium-225 gives the best results and does minor damage to the nearby tissues (affects 1-2 surrounding cells, compared to 100-200 cells affected by Lu-177). Also, one of the good things about PSMA therapy is that it doesn't have too much of an effect on the red bone marrow and the blood system. But if the bone metastases spread to other body parts, you are more likely to get anemia and other blood problems. Therapy could have mild adverse effects on the kidneys (except for Radium, which is eliminated by the intestine).
In general, targeted therapy is safe, doesn't involve harsh treatments, and has a low level of toxicity compared to other ways to treat cancer.
How can doctors ensure that radionuclide therapy works?
As we said, the surface of prostate cells contains a unique protein PSMA (prostate-specific membrane antigen). When a person is healthy, his level isn't very high, but it goes up a lot when he has prostate cancer. PSMA is also found on cells that have spread.
The ability of tumor cells to store PSMA is a requirement for Lu177-PSMA therapy to work. PET-CT with Ga68-PSMA or dosimetry with an iodine isotope is done before therapy to predict what the treatment might do. Scintigraphy is also performed.
Using this method in a few of the best foreign clinics has shown that patients' conditions have improved in 50% of cases. The distant metastases have shrunk or disappeared, which is usually very hard to treat.
Benchmarks to test the effectiveness of PSMA therapy
For people with metastatic prostate cancer, doctors use the following main criteria to judge how well the Lu-177 treatment works:
- Dropping the PSA level. Doctors track how long the patient stays stable and how quickly the PSA level drops after treatment. The treatment worked when the amount of PSA in the blood went down by 50-60%.
- Bettering PET scan for PSMA resuts. The pictures we all can see can show when there are metastases. Compare the images taken before and after therapy to see how well the treatment worked. Then, using regular scans, doctors determine how long the patient can stay stable without worsening the disease.
- Improving the patient's condition is another way to measure how well it works. Metastases in bones and soft tissues got smaller, and pain syndrome got less severe. Clinical studies have shown that therapy can help lessen symptoms like pain and improve life. The treatment had no significant side effects, and the quality of life was good. But the indicator is different when different groups of patients are studied.
Hospitals for targeted radiotherapy
The database of hospitals that provide high-quality targeted therapy has hundreds of clinics worldwide. We present you a list of TOP medical facilities which perform Lu-177, Ac-225, and Ra-223 cancer treatment:
What about actual patients' cases?
Researchers from Australia in the clinical study proved that radioligand therapy works well; it is safe and low-toxic for outpatient palliative treatment.
Patients with mCRPC (metastatic castration-resistant prostate cancer) whose bone marrow and liver worked well enough were included. Gallium-68-PSMA-11 PET/CT was used to measure the patients' starting point and response. Up to four cycles of therapy, each lasting eight weeks, were given. The answer was measured by the prostate-specific antigen (PSA) and a PET/CT at week 12. Researchers looked at how often toxicity of grade 3 happened and how it related to risk factors like age 70, prior/concurrent therapy, the existence of metastases, and the number of cycles finished.
Results: One hundred patients finished one cycle of Lu 177 PSMA I&T and had both PSA and PET/CT tests to see how their bodies reacted. The median age was 70, the number of previous treatments was three, and the median time between visits was 12 months. The 68Ga-PSMA-11 PET/CT response is linked to a better overall survival rate after one year.
Regarding hematological toxicity, 11% of people had cytopenia of grade 3.
Myelodysplasia/acute leukemia has not been seen or heard of. There was no evidence of a link between risk factors.
How can we help?
Lutetium and other radioligand therapy have been approved by scientists as a way to treat prostate cancer that has already spread. AiroMedical will help you find a clinic with skilled doctors and up-to-date equipment that offers this therapy.
Our database has information on hundreds of good hospitals worldwide that use Lutathera, Pluvicto, Xofigo, or Actinium-225 to treat advanced prostate cancer.
Treatment depends on a lot of different things. Patients with cancer can talk to an oncologist about treatment options and studies that support these suggestions. A second opinion from an expert can give the patient more information.
Please contact us, and we'll help you find the best solution!
References:
- The New England Journal of Medicine: Lutetium-177–PSMA-617
- Nаtional Library of Medicine: Safety and Efficacy of Lutetium-PSMA therapy
- Nаtional Library of Medicine: Prostate-Specific Membrane Antigen-Targeted Radiopharmaceuticals in Diagnosis and Therapy of Prostate Cancer: Current Status and Future Perspectives
- Prostate Cancer Foundation: Breaking News: First-in-Class Radioligand Therapy Approved for Advanced Prostate Cancer








