Thyroid Cancer Guide

Up to 30% of thyroid cancer cases come back.
The majority of thyroid tumor incidences occur in people over 40.
Well-differentiated thyroid cancer makes up more than 90% of all cases.
Recurrence of the such location of tumors happens even decades after the first diagnosis.
 What is the thyroid gland, and why is it so important?
What is the thyroid gland, and why is it so important?
The thyroid gland is a vital hormone gland. It is responsible for how the body works, grows and develops. It keeps a steady amount of thyroid hormones in the bloodstream, which helps to keep many body functions in balance. The thyroid gland makes more hormones when the body needs more energy, such as growing, in the cold, or during pregnancy. They regulate blood pressure, heart rate, body temperature, and weight.
In medical terms, this organ, called the glandula thyreoidea, is in the front of the neck, right below the voice box. It looks like a butterfly: the two side lobes rest against and around the windpipe (trachea) and are joined at the front by a thin strip of tissue.
 What is thyroid cancer?
What is thyroid cancer?
Thyroid cancer is a growth in the gland caused by thyroid cells that divide and grow out of control. So, cells can move to other body parts, like the lungs, bones, etc. Metastasis is the name for this spread of cancer cells.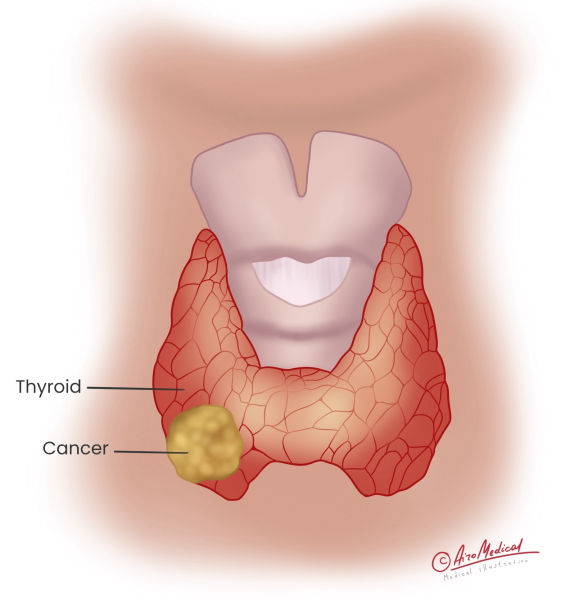
The thyroid gland can produce four different kinds of tumors:
- Papillary is the most common type, making up 90% of all thyroid cancers. Most of the time, it forms in one part, grows slowly, and goes all the way to the lymph nodes in the neck.
- Follicular is more common in middle-aged women and is 4% of cases. One type that starts in specific follicular cells is Hurthle cell cancer. It is significantly more likely than other follicular thyroid cancers to spread lymph nodes.
- Medullary cancer is rare and affects cells that control how much calcium is in the blood. This type makes up almost 2% of all cases of thyroid cancer.
- Anaplastic is about 2% to 3% of all thyroid gland neoplasms and is an aggressive malignant tumor. It is still one of the most deadly diseases, and the outlook is not good.
In the last few decades, the number of people getting thyroid cancer has increased worldwide. The amount of people who get thyroid cancer yearly is 5.4% for men and 6.5% for women.
 What are the factors that increase the risk?
What are the factors that increase the risk?
If you asked what causes thyroid cancer, there are no significant ones. Risk factors can increase the probability and do not immediately cause cancer. Some people with many risk factors never acquire cancer, whereas others without any do. Understand your potential risks and talk to your doctor to make better lifestyle and healthcare choices.
Thyroid cancer risk factors include:
- Gender. Women account for three-quarters of thyroid malignancies.
- Age. Two-thirds of thyroid cancer cases occur in adults 20–55. Over-60s have the most anaplastic thyroid cancer cases.
- Genetics. Some thyroid cancers are genetic. Here are key facts regarding this disease, its genes, and how it impacts families. Family history increases medullar thyroid cancer risk. Papillary thyroid carcinoma is more frequent in families with specific colon polyps.
- Radiation. Papillary and follicular thyroid cancers may increase with moderate head and neck radiation. These exposures include:
- Head-and-neck radiotherapy for lymphoma.
- I-131, especially in children.
- Nuclear power accidents like the 1986 Chornobyl accident and the 2011 Fukushima earthquake
- Atomic weapons factories release I-131.
- Low-iodine diet. The thyroid needs iodine for regular work. If the salt contains iodine, it can be used to prevent issues.
- Race. Thyroid cancer can affect anyone, but whites and Asians are more prone to have it.
- Breast cancer. A recent study indicated that breast cancer survivors might be more likely to get thyroid cancer, especially in the first five years and among younger survivors.
What about prevention?
Most people with thyroid cancer don't have any known risk factors, so we can not stop the cancer of the thyroid gland in most cases.
Radiation exposure, especially when a child is young, is known to increase the risk of getting thyroid cancer. Radiation is no longer used to treat less severe illnesses because of this. Children are also exposed to radiation during imaging tests like x-rays and CT scans. Still, the doses are much lower, so it's not clear how much they would perhaps increase the likelihood of thyroid cancer (or other cancers). Even if there is a minimal increase in risk, children shouldn't have all these tests unless they're indispensable. When required, they should be done with the tiniest dose of radiation that still gives a clear picture.
You can do genetic tests to determine the gene changes linked to familial medullary thyroid cancer. Because of this, most cases in families can be stopped or treated early if the thyroid gland is removed. Once the disease is found in a family member, doctors can test the rest to see if they also have the mutated gene.
Suppose your family has a history of thyroid cancer. In that case, you should see an up-to-date doctor on the latest developments in genetic counseling and genetic testing for this disease. In the cases of an abnormal gene, thyroid gland removal should be considered a stopped cancer measure.
 What are the symptoms?
What are the symptoms?
Like other kinds of cancer, the thyroid, in its early stages, does not cause any signs. However, as the tumor grows, the following symptoms of thyroid cancer may occur:
- A bump or lump in the front of the neck that doesn't hurt. However, only 1 in 20 neck lumps is cancer.
- Neck glands that are swollen.
- The voice can change.
- Dry cough with no apparent cause and doesn't get better after a few weeks.
- Sore throat that doesn't go away.
- Having trouble swallowing is also a symptom of thyroid cancer
Signs indicating thyroid cancer are a reason to perform additional tests.
 Diagnostic tests
Diagnostic tests
The results of these tests will tell your doctor more about the problem and help them figure out the best way to treat you:
- Blood tests do not directly show if a person has thyroid cancer, but they show how well the gland works.
- Ultrasound: A picture of the thyroid gland is made with special equipment that sends sound waves and records the echoes that come back. If there are scans, they might show knots or shapes. The doctor concludes.
- Radioactive iodine scanning (scintigraphy): patient swallows a small amount of radioactive iodine or is injected into a vein. The gland takes in radioactive iodine. The organ is then looked at with a special camera. Malignancy can happen in lymph nodes that have less iodine.
- A CT scan, or computer tomography, is a procedure during which the x-rays and a computer make detailed images of the internal structure of organs and body parts. It takes photos from multiple points of view. The computer puts them all together to create a 3D picture.
- Magnetic resonance imaging (MRI) An MRI can help physicians determine how big the thyroid cancer is and how far it has expanded. It can show that the tumor occurs in the neck lymph nodes. The doctor may also prescribe this scan to determine whether the neoplasm has spread to other body parts (chest, abdomen).
- A PET scan (positron emission tomography) involves giving a specific type of glucose to a patient so that a camera can see what's happening inside their body. If there is a disease, this difference shows up where the cancer is forming.
- During a biopsy, a special (thin and flat) needle is inserted directly into the lump to remove a small piece of tissue with fluid and cells. This test is done in a lab, and a doctor-pathologist can look at it. Labs give accurate answers about whether cancer cells are present.
After the confirming diagnosis, the stage of the tumor is determined. Knowing the type of thyroid cancer and its stage will allow the doctor to choose a strategy for the best further treatment.
Where to go for treatment?
 Methods of cure
Methods of cure
Most types of thyroid cancer can be treated differently, mainly if the neoplasm hasn't spread to other organs. So, there are various options to treat. When doctors know more about a case, they can choose the best chance to cure it.
- Systemic chemotherapy, in which a drug is injected into the blood and spreads throughout the body to kill cancer cells. The procedure is done in cycles that are spaced out. The treatment can take months.
- Immunotherapy is when certain medicines boost a patient's immune system to kill off malignant thyroid cells.
- Radioiodine therapy (I-131 therapy) is a type of treatment that uses nuclear medicine. I-131, an isotope of iodine that gives off radiation, is injected into the bloodstream in a small amount. The thyroid gland then makes more of the isotope and uses it to eliminate the cancer cells.
- Targeted therapy uses drugs that only affect the genes or proteins that cancer needs to expand. At the molecular level, thyroid cancer cannot grow or spread.
- Hormonal therapy uses hormone-like drugs to make up for hormones that the thyroid gland isn't making enough. It stops the substances that cause cancer cells from growing.
- External-beam radiation therapy is rarely required for thyroid cancer treatment, preferably in later stages, when cancer spreads to the trachea, voice box, or esophagus. Radiation therapy usually follows surgery, and only cancer cells in one region are affected. Young thyroid cancer patients rarely receive it.
- Surgical removing the thyroid gland is the most common treatment for thyroid cancer. There are three ways to do this: remove part of the gland, remove the whole gland, or remove the gland and the lymph nodes simultaneously.
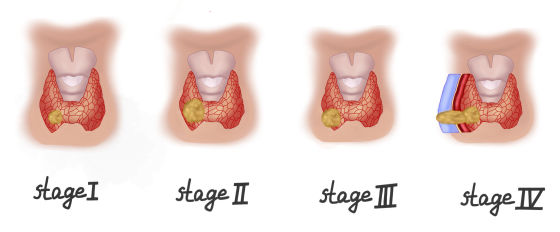
Different types and stages of thyroid cancer may need other treatments. A group of experts will help you figure this out.
What clinics do experts recommend for thyroid cancer treatment?
 New ways to treat illness
New ways to treat illness
There is no one way to treat cancer because of the difference between each patient and each tumor. Knowing as much as possible about the patient's medical history and the tumor is essential for successful treatment. This information will help you keep up with the latest advances in thyroid cancer treatment and know how to use them. When the most up-to-date methods are used, treatment dynamics improve.
These ways are:
- Transarterial chemoembolization (TACE) is a minimally hurting procedure in which chemotherapy is given directly to a thyroid tumor through a blood vessel. During the process, the arteries are embolized, and the blood flow to the gland is cut off. So, the chemotherapy stays at a high level in the center of the neoplasm.
- Transarterial chemoperfusion (TACP): Chemotherapy drugs are put directly into the artery that feeds the thyroid tumor through a catheter. The drug kills cancer cells because there is so much inside the tumor.
- Ablation therapy (RFA, MWA, ethanol) uses needle electrodes to send heat energy to the tumor, which shrinks and destroys the thyroid tumor. Minimally invasive techniques like ablation therapy have become an alternative to surgical procedures for people who are too sick for surgery or want a more active treatment plan.
- A beam of radiation (protons) is used in proton therapy, a type of radiotherapy. The particles with a certain amount of radiation are sent directly to the cancerous tissue in the thyroid, skipping over the healthy tissue nearby.
- Surgical treatment (Da Vinci® robotic thyroid surgery) is a minimally hurting type of thyroid surgery that uses a robot. The automated system makes it possible to make tiny cuts and use stitches that can't be seen. It isn't possible with traditional surgery.
When someone is told they have thyroid cancer, they usually feel scared. But it's important to remember that almost every disease can be treated. You must put together a team of experts with much experience and make the right choice. And we will help.
Who treats thyroid cancer the best?
 Stats and predictions
Stats and predictions
A large number of thyroid cancers are well-treatable. Oncologists can successfully cure papillary and follicular cancer (the most common thyroid cancer) at the early stages in more than 98% of cases. That cancer is less likely to expand outside of the thyroid gland.
Thyroid cancer is the most commonly found endocrine cancer in the world. Statistics from the research show that thyroid cancer has become more frequent in the last few decades. Researchers think this is because new sensory diagnostic tests have made it easier to find smaller cancers.
The American Cancer Society says that the 5-year survival rate for cancer only in the thyroid gland is almost 100% or 2/3 of all cases found.
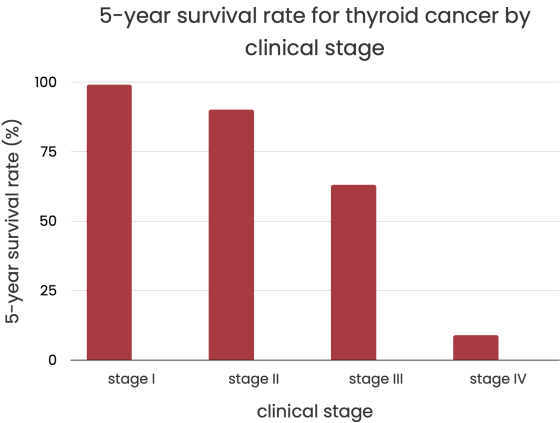
Cancer in stage II has a 90% chance of being cured, stage III has a 63% chance, and stage IV has a 9% chance.
Using information about tumors, the latest medical advances, and disease statistics, the team of experts comes up with a unique solution for each case. Doctors can choose the best treatment plan only by considering how each patient is different. We collaborated only with such specialists and trusted clinics.
References:
- The Lancet Diabetes & Endocrinology: A worldwide journey of thyroid cancer incidence centered on tumor histology
- NHS: Treatment Thyroid cancer
- American Cancer Society: If You Have Thyroid Cancer
- Endocrine Web: What Is Thyroid Cancer?
- WebMD: What Are The Treatments for Thyroid Cancer?
- Cancer Council NSW: Targeted therapy for thyroid cancer
- American Society of Clinical Oncology (ASCO): Thyroid Cancer: Statistics
- National Library of Medicine: Global Burden of Thyroid Cancer From 1990 to 2017

















