Spina Bifida Guide

75% of all disease cases are the most severe form of spina bifida (SB).
Prenatal SB surgery reduces the risk of a shunt almost twice.
1 in every 1000 babies has a form of SB with neurological symptoms.
Folic acid supplements taken before and during pregnancy can cut the risk by up to 72%.
 About the spina bifida development process
About the spina bifida development process
In the early stages of fetal development, a flat sheet of cells called the neural plate folds inward and fuses to form a tube-like structure that will eventually become the brain and spinal cord. This process, called neurulation, happens between day 18 and day 21 after fertilization. For it to work right, several genes and signaling pathways need to be expressed correctly.
Spina bifida happens when the neural tube, the part of an embryo that grows into the brain and spinal cord, doesn't close while the baby is still growing. This causes a hole or gap in the spine's bones, which lets the spinal cord and its coverings poke out. This can cause a number of neurological problems.
 What is spina bifida?
What is spina bifida?
It is a congenital disorder where the spine is open (bifid) and often involves the spinal cord. It comes from the Latin word for "split spine," which is a congenital disability that happens when part of a baby's spine doesn't form fitting.
SB occurs when the brain or spinal cord doesn't grow as it should. It can show up anywhere along the spine and is usually there when a person is born. A fluid-filled sac may cause a split on the spine, which has grown out of the body.
Types of spina bifida
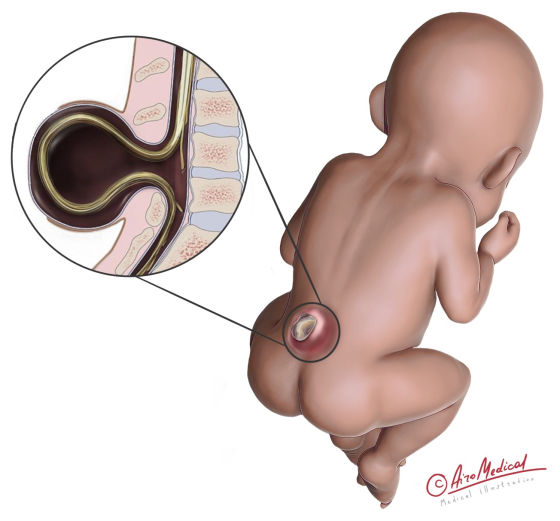 The disorder can range in type and severity, changing the symptoms and possible complications due to the characteristics of spina bifida.
The disorder can range in type and severity, changing the symptoms and possible complications due to the characteristics of spina bifida.
- Spina bifida occulta is the mildest form and is often not noticed. In this situation, the spine's vertebrae don't close all the way, but the spinal cord and nerves are usually unaffected. Some people with this form may have a small birthmark or patch of hair over the affected area, but this usually doesn't cause any problems. As estimated, 10% of adults have this form without symptoms.
- Meningocele occurs when the meninges, the protective layer around the spinal cord, don't close properly and stick out through a hole in the spine. It makes a fluid-filled sac at the baby’s back that might or might not be covered by skin. Most of the time, the sac does not affect the spinal cord or nerves. However, surgery is still needed. Due to the facts about spina bifida, this kind is the rarest.
- Myelomeningocele is the worst condition and occurs in the two third cases. It happens when part of the spinal cord sticks out of the back. It can make nerves and tissues stand out, leading to paralysis and problems with the bowels, bladder, and others. Surgery is needed to close the hole in the spine and protect the spinal cord.
Spina bifida complications
This condition leads to various complications and long-term issues. They include hydrocephalus, neurological, orthopedic, skin, mental health, cognitive, sexual, and reproductive problems. Early intervention and regular medical care can help improve the quality of life.
 Is it determined what the cause of spina bifida is?
Is it determined what the cause of spina bifida is?
Although the specific factors that are causes of spina bifida are not entirely understood.
Researchers identify such spina bifida risk factors
- Genetic. Even though much research has been done, scientists have found only a few genes. Researchers consider that genetic factors account for 60–70% of cases of the most severe form. At the same time, about 1,645 babies are born with SB annually only in the United States, and about 95% come from families where the condition has never been seen.
- Chronic conditions. Women with uncontrolled diabetes during pregnancy have more risks of having a baby with such a disorder. It is because high blood sugar levels can damage the developing nervous system. Women who are overweight or obese before pregnancy may also have an increased risk due to inflammation and nutrient imbalances.
- Toxins exposure and malnutrition during pregnancy. SB can be caused by exposure to toxins, poor nutrition in pregnant women, such as folic acid deficits, and some drugs like valproate and carbamazepine. These medications are connected to disease development and are frequently prescribed to treat epilepsy and some issues with mental health, like bipolar disorder.
- Combining the factors. To the question of is spina bifida genetic only, The Spina Bifida Association answers that a combination of genetic predisposition and environmental factors bring on the disorder.
Knowing the risk factors and taking suitable precautions can help lower the chance of getting SB and improve life for people with it.
Prevention for spina bifida
Some things can be done to lessen the likelihood of having the disorder. To decrease the risk:
- Take folic acid supplements. Several studies have demonstrated that taking folic acid supplements before becoming pregnant and while pregnant can considerably reduce the likelihood of having a baby born with SB. It is recommended that women who are trying to conceive take a daily supplement of folic acid containing 400 micrograms and that they continue doing so throughout their pregnancy. Folic acid is critical for the proper development of a healthy baby.
- Consuming a nutritious diet high in whole fruits, vegetables, and whole grains is one of the best to ensure you get enough of the critical nutrients your body needs while pregnant.
- Staying away from potentially hazardous substances, such as chemicals, pesticides, and some drugs, is especially important during the first trimester of pregnancy.
- Take care of chronic conditions: Women with diabetes or epilepsy, for example, should work closely with their healthcare practitioner to manage their condition during pregnancy to help lower the likelihood of SB occurring in their offspring.
- Seek the advice of a genetic counselor: If you have a close family member with SB or already have a child affected by the condition, you should talk with a genetic counselor to understand your risk and potential prevention strategies.
 Spina bifida signs and symptoms
Spina bifida signs and symptoms
This disorder affects how the spinal cord grows and develops. It can cause several different symptoms. Some of them are as follows:
- Physical problems: The most apparent sign of spina bifida is a visible spine deformity, like a bulge or sac-like protrusion on the back. It can happen anywhere along the spine and can be covered by skin or not. If the deformity is large enough, the spinal cord may be visible.
- Sensory issues: SB can cause numbness, tingling, or weakness in the legs, feet, or other body parts. Some people with SB may also lose feeling in the regions of their bodies affected by the condition.
- Bladder and bowel control problems: As the nerve endings that control the bladder and bowel functions are affected, this can cause incontinence or make emptying the bladder or bowels hard.
- Hydrocephalus is a frequent sign of spina bifida. It means that cerebrospinal fluid builds up in the brain. It can lead to headaches, nausea and vomiting, and trouble seeing.
- Mobility problems include paralysis, weakness or limited movement, difficulty walking, balance issues, and spinal cord tethering.
The severity of spina bifida symptoms varies greatly and depends on the location of the tear in the spine. Some people may have any or very few. A gap having few parts is more likely to cause leg paralysis and mobility difficulties. Gaps in the middle or at the base are often just incontinence problems.
 How is spina bifida diagnosed?
How is spina bifida diagnosed?
The illness can be found during pregnancy or after giving birth. Spina bifida occulta might not be discovered until late childhood or might never be recognized.
The disease can be diagnosed with such tests
- Maternal blood screening measures alpha-fetoprotein (AFP) levels in the mother's blood that may indicate the presence of spina bifida in the developing fetus. The blood test is done between the 16th and 18th week of pregnancy. In the case of SB in the fetus, the level of AFP rises.
- Ultrasound uses high-frequency sound waves to create images of the fetus and can help detect abnormalities in the spine.
- Amniocentesis: In this test, a small amount of amniotic fluid is removed from the sac surrounding the fetus. Then doctors analyze it for signs of spina bifida.
After birth, a physical examination and imaging tests, including X-rays, CT scans, and MRI scans, can help to diagnose SB.
As the causes of spina bifida are still not precisely known, it is recommended that pregnant women who are planning to become pregnant undergo prenatal screening and testing for spina bifida in pregnancy. Early detection and treatment can improve outcomes for both the mother and the baby.
Stages or degrees
Due to the National Institute of Neurological Disorders and Stroke, the SB is divided into the following degrees:
- Occulta is the mildest and most common, where one or more vertebrae are malformed and covered by a layer of skin. It shows no symptoms in most people and is discovered by accident on an x-ray.
- Closed neural tube defects are a group of disorders where the spine may have malformations of fat, bone, or the meninges that cover the spinal cord. These often require surgery for spina bifida in childhood and can cause weakness of the legs and bowel and bladder control issues.
- Meningocele is a disorder where a spinal fluid sac protrudes through a hole in the bone covering the spine. Meningocele contains no nerves and may or may not be covered by a layer of skin. Symptoms are usually mild.
- Myelomeningocele is the most severe, where a portion of the spinal cord or nerves protrude through an opening in the spine that may or may not is covered by the meninges. It can cause numerous symptoms like leg weakness, bladder and bowel dysfunction, and changes in brain structure. It requires surgical treatment for spina bifida when the defect must be closed shortly after birth.
Where to treat SB the best?
 What treatments are available for spina bifida?
What treatments are available for spina bifida?
SB is a complex condition that requires various treatments to manage symptoms and improve quality of life. Here are some of the available SB treatments:
Surgical options
Surgery is often the first line of treatment, particularly for the most severe forms of the condition, such as myelomeningocele. The surgery treatment of spina bifida in babies is typically performed within the first 48 hours after birth to prevent further damage to the exposed spinal cord and to reduce the risk of infection.
During the spina bifida surgery after birth, the neurosurgeon will carefully place the spinal cord and surrounding tissues back into the spinal canal and cover them with multiple layers of tissue, such as muscle or skin, to protect them. A plastic surgeon could help with the next step if closing a defect is hard.
While spina bifida surgeries can help prevent further damage to the spinal cord, they cannot reverse the damage already done. Some individuals may experience long-term effects, such as paralysis, loss of sensation, and bladder and bowel dysfunction, despite surgery.
About 80% to 90% of children get hydrocephalus, which happens when too much cerebrospinal fluid accumulates in the brain's ventricles, and the pressure inside the head rises. Most kids will need a ventricular shunt to prevent cerebrospinal fluid from building up in their brains. The shunt stays in a person's body for the rest of their life.
So, patients living with spina bifida need
- Medications to manage symptoms such as pain, muscle spasms, urinary incontinence, and bowel incontinence.
- Physical therapy improves strength, flexibility, and mobility and prevents deformities and pressure sores.
- Occupational therapy teaches patients how to perform daily activities and improve their independence.
- Braces and orthotics support the spine, hips, and legs, improve posture, and reduce the risk of deformities.
- Various techniques include catheterization, enemas, and medications to manage bladder and bowel function.
- Assistive devices, such as wheelchairs, walkers, and crutches, help with mobility.
- Surgery for associated conditions such as scoliosis or clubfoot.
All these measures can be used in spina bifida treatment in adults, promoting physical and emotional well-being, improving overall health, and enhancing the quality of life.
Spina bifida clinics
 What are the new treatment options for spina bifida?
What are the new treatment options for spina bifida?
Surgery is the best way how can spina bifida to be cured, to close the spine and stop the nerves from getting hurt. Thanks to recent improvements, the spine can now be fixed less invasively.
Fetal surgery is done on a developing fetus to fix problems from the start or treat conditions that could affect the baby's health or development. It is a highly specialized field requiring a multidisciplinary and experienced medical team.
There are two main types of fetal surgery for spina bifida
- Open fetal surgery: A large cut is made in the uterus to reach the fetus. The hole in the spine is fixed, and the uterus is closed, which lets the pregnancy go on. Most open surgery on a fetus is done between 19 and 25 weeks of pregnancy.
- Fetoscopic surgery involves making minor cuts in the uterus and inserting a fetoscope, which is a tiny camera, to see the fetus. The hole in the spine is then fixed with surgical tools. Most fetoscopic surgeries are done between 24 and 26 weeks of pregnancy. That is the best way how can spina bifida be corrected.
What surgical approach is better
Compared to fetoscopic surgery, however, open fetal surgery has a higher risk of complications, such as early labor and a ruptured uterus.
The spina bifida surgery success rate depends on several things, such as the type and severity of the condition, the gestational age of the baby at the time of surgery, and the surgical team's experience.
Overall, babies with SB have better neurological outcomes after surgery when they are still in the womb. Intervention can reduce the need for a shunt to treat hydrocephalus and improve motor function and bladder control in some cases. The Management of Myelomeningocele Study (MOMS), a landmark study that compared fetal surgery to surgery after birth, found that babies who had fetal surgery did better than those who had surgery after birth. The study found that babies who had surgery while still in the womb were less likely to need a shunt for hydrocephalus and were more likely to be able to walk on their own by the time they were 30 months old.
About stem cell therapy for spina bifida
A recent study suggests that injecting stem cells into the amniotic fluid of fetuses with SB may help them move better and reduce the need for shunt placement. But more research must ensure this treatment is safe and works.
Spina bifida specialists
 Statistics for spina bifida
Statistics for spina bifida
SB disorder affects the patients' lives leading to numerous health and mental issues. The Centers for Research and Prevention of Birth Defects in the US say that 14% of children born with myelomeningocele die before they turn five. This is primarily because of problems caused by a herniated hindbrain. In addition, 85% of patients need shunting, and 45% of shunts have issues within the first year.
Concerning life expectancy for spina bifida
75% of children born with a more severe form of this disability can live into their early 20s and beyond with help and support. Most of the time, doctors say that about 90% of people with SB will live into their fourth decade. But this number has increased over time because medical technology has improved.
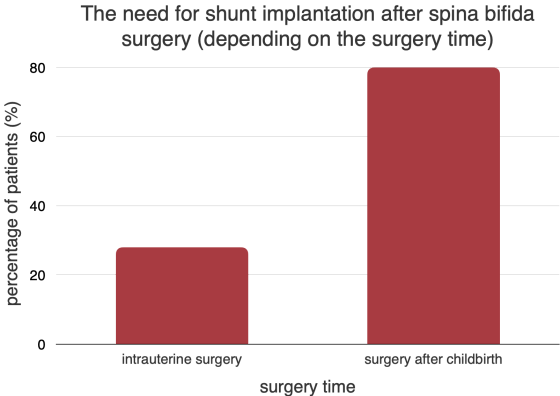
A study done in Poland is constructive for comparing different types of treatment. This study aimed to look at the outcomes of intrauterine myelomeningocele repair using data from newborns and babies in the postnatal period. A shunt had to be put in 27.8% of patients who had surgery while still in the womb, compared with 80% of people who had surgery after birth. Intrauterine surgery makes it much less likely that the disease will progress.
AiroMedical experts are ready to find the best solution suitable for each case. If it exists somewhere, we will find it. We can help and give the proper medical care, which makes it possible for many children with spina bifida to live whole, active lives. With the new information we have, their chances keep getting better.
References:
- Zamłyński J, Olejek A, Koszutski T, Ziomek G, Horzelska E, Gajewska-Kucharek A, Maruniak-Chudek I, Herman-Sucharska I, Kluczewska E, Horak S, Bodzek P, Zamłyński M, Kowalik J, Horzelski T, Bohosiewicz J. Comparison of prenatal and postnatal treatments of spina bifida in Poland--a non-randomized, single-center study. J Matern Fetal Neonatal Med. 2014 Sep;27(14):1409-17. Doi: 10.3109/14767058.2013.858689. Epub 2013 Nov 26.
- MRC Vitamin Study Research Group. Prevention of neural tube defects: results of the Medical Research Council Vitamin Study. Lancet. 1991 Jul 20;338(8760):131-7. doi: 10.1016/0140-6736(91)90133-a. PMID: 1677062.
- Oakeshott, P., Hunt, G. M., Poulton, A., & Reid, F. (2010). The expectation of life and unexpected death in open spina bifida: a 40-year complete, non-selective, longitudinal cohort study. Developmental Medicine & Child Neurology, 52(8), 749-753. doi: 10.1111/j.1469-8749.2009.03543.x. PMID: 20015251.
- Wei, X., Ma, W., Gu, H., Liu, D., Luo, W., Bai, Y.,& Yuan, Z. (2020). Transamniotic mesenchymal stem cell therapy for neural tube defects preserves neural function through lesion-specific engraftment and regeneration. Cell Death & Disease, 11(7), 523. doi: 10.1038/s41419-020-2734-3. PMID: 32655141; PMCID: PMC7354991.
- Copp, A. J., Adzick, N. S., Chitty, L. S., Fletcher, J. M., Holmbeck, G. N., & Shaw, G. M. (2015). Spina Bifida. Nature Reviews. Disease Primers, 1, 15007. doi: 10.1038/nrdp.2015.7. PMID: 27189655; PMCID: PMC4898641; EMSID: EMS68524.

















