Keratoconus Guide

Only one in every ten patients has a relative with keratoconus disease.
People in the Middle East are five more likely to have keratoconus, up to 5% of the population.
Keratoconus disease usually starts when a person is in their 20s or 30s and worsens until their 40s.
In people with keratoconus, up to 59% have high allergy marker levels in their blood.
 What about the cornea?
What about the cornea?
The cornea is like the front window of the eye. A normal cornea is clear, dome-shaped, and helps focus light into the eye so we can see clearly. It's strong and maintains its round shape, helping to provide a clear vision. The cornea lets in light and bends it so that it can be focused onto the retina (a layer situated at the back of the eye). It is how we can see objects around us.
The cornea also works like a shield for the eye, protecting it from dust, germs, and other stuff that could damage it.
It's made up of five layers. The epithelium, the outermost layer, acts like a tough skin that helps keep out foreign things and soaks up oxygen and nutrients that the cornea needs to stay healthy.
 What is keratoconus disease?
What is keratoconus disease?
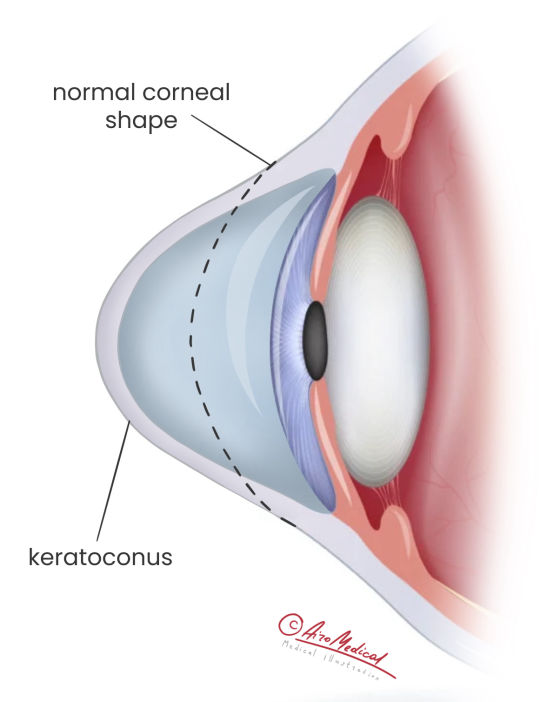 Keratoconus disease, or cone-shaped cornea, is a condition in the eye where the transparent front part, the cornea, gets thin and bulges like a cone. It can blur the vision with keratoconus, making lights seem too bright or glaring.
Keratoconus disease, or cone-shaped cornea, is a condition in the eye where the transparent front part, the cornea, gets thin and bulges like a cone. It can blur the vision with keratoconus, making lights seem too bright or glaring.
On the other hand, comparing keratoconus vs. normal eye, the cornea becomes thin and bulges into a cone-like shape. This change makes the cornea with keratoconus disease less capable of focusing light accurately onto the retina, which results in blurred and distorted vision. People with keratoconus can also become more sensitive to light and glare.
Keratoconus types
What does keratoconus look like? Keratoconus can look different depending on how the transparent front part of the eye, the cornea, has thinned and changed shape. The keratoconus types are:
- oval;
- globus;
- nipple (when it's in a small spot).
It can appear in the middle, top, or bottom of the front part of the eye, but it's mainly at the bottom. The spot that sticks out the most is the peak of the bulge.
 Causes of keratoconus and prevention
Causes of keratoconus and prevention
Keratoconus disease is thought to be caused by a mix of genes and environment. How do you get keratoconus? Doctors are still trying to figure out everything that can make someone more likely to get it. Knowing these risk factors can help adequately prevent or manage the condition if someone already has it.
Due to the study, frequent eye-rubbing, often seen with conditions like allergies, Down syndrome, or particular eye diseases, could be linked to a higher chance of getting corneal disease keratoconus.
The most significant risk factors
- Rubbing the eyes (up to 63% of patients with KC);
- Having a family member with KC (to the question is keratoconus genetic);
- Parents being closely related;
- Experiencing eye trauma;
- Wearing contact lenses;
- Being overweight;
- Smoking;
- Spending four or more hours per day in the sun.
Researchers say that in keratoconus, particular layers of the eye can be damaged or missing, and the vision can become scarred or thin. They are unsure why, but it might be related to changes in specific proteins.
Only about 10% of people with keratoconus have a family history of the condition, meaning it can be hereditary. Still, most people with it don't have an apparent genetic connection.
How to prevent it?
It's often not possible to prevent keratoconus disease because the exact causes of keratoconus are still unknown. However, you might lower your risk of developing it by:
- don't rub your eyes;
- ensure your contact lenses fit well;
- wear sunglasses to protect your eyes from UV rays;
- go to the doctor if your eyes hurt, like from allergies.
Regular eye check-ups are the key to managing keratoconus disease. These visits can spot the condition early, slowing it down and keeping your sight better for longer. The doctor can also notice changes in your vision or the shape of your cornea, helping to adjust treatment as needed.
 Keratoconus symptoms
Keratoconus symptoms
Keratoconus disease is an eye issue that can cause a bunch of problems. Someone with it might see things as blurry or warped. Bright lights could seem too firm, and driving at night might be challenging. This person might need new glasses often because how they see can change fast. Vision might even become cloudy all of a sudden. It could be hard to see in the dark, and lights might have a halo around them. There might also be some eye pain or headaches because of this issue.
Even though keratoconus might start in one eye, it usually affects both eyes in about 96 percent of cases.
Typical signs of the disease
Keratoconus shows different signs and symptoms. A person might not notice anything in the beginning. But then, they might start to have problems like being more sensitive to light, seeing circles around objects, or having sore, itchy, or painful eyes. They might want to rub their eyes more, have trouble seeing things near and far, and see things blurry. The progressive condition leads to nearsightedness, uneven vision because of astigmatism, and even scars on the cornea, which can worsen vision.
About complications
Corneal hydrops is a problem that can happen with severe keratoconus. It occurs suddenly and makes the cornea cloudy because it fills with fluid. This fluid comes from a break in a layer of the cornea called Descemet's membrane, which can break because the cornea is weak. This causes a sudden and painful drop in vision.
 Diagnosing keratoconus: methods & tools
Diagnosing keratoconus: methods & tools
How to diagnose keratoconus? Several diagnostic tests can help detect keratoconus disease. Doctors perform:
- An eye examination is an initial step where a doctor-ophthalmologist checks for the telltale signs of keratoconus, such as corneal thinning, scarring, or changes in shape.
- The refraction test determines if there's a change in how light is bent when it enters the eye, which could indicate keratoconus.
- Slit-lamp examination: The doctor uses a vertical beam of light and a low-powered microscope to look at the front and back of the eye, checking for issues in the cornea.
- Corneal topography is the best method for measuring the cornea's curve, often considered the "gold standard." It creates a detailed, map-like image of the cornea's surface curvature. It identifies early signs, even if no symptoms appear.
- Keratometry measures the curve of the cornea. This part of the keratoconus test works by shining a circle of light on the cornea and looking at the light that bounces back. It can show if the cornea is distorted, a sign of the illness.
- Pachymetry measures the thickness of the cornea. A thinner cornea can be a sign of keratoconus.
- Pentacam corneal tomography is an easy eye test that uses a camera to create a 3D picture of the cornea. It helps doctors see if the cornea is bulging and how thick it is, which can help track the disease over time.
Each test provides valuable information, helping diagnose keratoconus disease and differentiate it from other conditions like corneal degeneration that lead to bilateral blindness.
Stages of keratoconus disease
Keratoconus is a condition that worsens over time, moving from early to severe stages. Different systems categorize these, like the Amsler-Krumeich system. They check how curved or thin the cornea is and how much short-sightedness and uneven eye shape there is. All these measurements increase as keratoconus gets worse.
- At Stage 1, or mild keratoconus disease, vision can usually be corrected well with glasses or keratoconus contact lenses. The person might not even know anything is wrong. Treatment at this stage usually involves corneal cross-linking to strengthen the cornea and prevent the keratoconus from worsening.
- At Stage 2, or the moderate keratoconus disease sign worsens, it might become hard to entirely correct vision with glasses or contacts. Rigid contact lenses might be needed to improve vision, and corneal cross-linking should be done if it hasn't been already.
- Stage 3 is severe keratoconus. At this point, glasses or contacts can't correct vision well. Rigid contact lenses become necessary to improve vision. It is the last stage where corneal cross-linking for keratoconus disease can be done safely. Beyond this stage, the cornea is too thin for the treatment.
- At Stage 4, vision is feeble and can't be corrected well. In this advanced stage, the cornea might have scars that limit vision. The cornea is too thin for cross-linking. For this stage of the keratoconus disease, a corneal transplant is usually the only option. After a transplant, rigid contact lenses might still be used to correct vision.
Overall, keratoconus stages help us understand what to expect from the condition but don't directly influence how to treat keratoconus disease.
Where to go to treat keratoconus?
 Treatment options for keratoconus disease
Treatment options for keratoconus disease
Keratoconus disease treatment depends on how severe the condition is, mainly focusing on fixing vision problems. If you ask if keratoconus can be cured, we say yes. And there are many options, from lenses to transplant surgery.
Lenses
- Glasses are used for better vision and to fix minor astigmatism and, in most cases, are part of a permanent cure for keratoconus.
- New soft lenses for keratoconus disease are helpful for early keratoconus disease, correcting unclear or warped vision.
- Rigid gas permeable lenses are stronger and suitable for worsening keratoconus.
- Hybrid contact lenses have a firm center and soft edge, which might be more comfortable.
- Sclera lenses for keratoconus are best for advanced stages. These sit on the white part of the eye and provide a smooth surface for better vision.
Keratoconus surgery
They are another solution for treating keratoconus eye disease, usually considered when the lenses are insufficient to correct the vision problems.
Cross-linking treatments
- Epithelium-off CXL: Doctors remove the cornea's top layer, put special eye drops, and then shine a UV-A light. It helps to make the cornea stronger, treating keratoconus disease.
- Epithelium-on CXL is like the first method, but the top layer of the cornea stays on. It means fewer side effects, but the riboflavin eye drops don't get in as quickly.
- Accelerated cross-linking is a faster version of the first two methods. It uses a brighter UV light, so it's quicker.
- Customized cross-linking (PiXL): This keratoconus eye surgery only targets the vulnerable parts of the cornea. It helps to reduce problems and improve healing.
The standard CXL treatment was safe and helped keep the sharpness of vision and eye shape steady in people with severe, worsening keratoconus disease. After two years of checking, the condition stopped in about 96.6% of the cases.
Intracorneal Ring Segments
Doctors put tiny, half-circle inserts into the cornea to make it flatter and help improve vision. It is usually used for more severe cases of keratoconus.
These treatment methods can stop the disease from getting worse, but they can't fix the eye damage that has already happened.
Alternative treatment for keratoconus
Keratoconus is challenging, but several alternative treatments can complement traditional medical approaches. These therapies focus on non-invasive methods and natural remedies to support eye health and potentially slow disease progression:
- Natural treatment refers to non-invasive practices such as maintaining a healthy diet and regular exercise, which can contribute to overall eye health.
- Natural remedies may include specific eye exercises, dietary changes, or herbal therapies that may help improve eye health.
- Supplements include vitamins or minerals known to support eye health, such as Vitamin A or Omega-3 fatty acids. Some studies report on the Vitamin D positive effect in keratoconus patients.
- Microwave: A non-invasive treatment that uses controlled heat to reshape the cornea.
- Ayurvedic is a traditional Indian medicinal approach that promotes healing and includes herbal treatments, dietary changes, and lifestyle adjustments.
- Homeopathy is a treatment philosophy that uses small amounts of natural substances to stimulate the body's healing abilities.
- Stem cell therapy uses the approach when stem cells, potentially developing into many different types of cells, help to repair the damaged cornea.
While alternative treatments may not replace conventional medicine, these options can offer supportive measures to improve overall eye health. However, discuss any alternative therapy with a healthcare provider before using it.
Selected keratoconus centers
 New keratoconus treatments
New keratoconus treatments
When the condition is severe and causes significant changes to the cornea or vision, doctors might suggest new treatments for keratoconus disease, including surgery. Cornea replacement is one of the most promising approaches and best treatments for keratoconus disease.
Cornea transplant (keratoplasty)
Penetrating keratoplasty
This is a full cornea transplant. The middle part of the cornea, which is damaged, is replaced with healthy tissue from a donor. Vision is usually blurry for around three to six months after the surgery. Patients must also take medicine to prevent their bodies from rejecting the new tissue.
Deep anterior layered keratoplasty
This latest keratoconus disease treatment replaces the cornea's front part but keeps the inner lining. It can avoid some problems that might happen with a full cornea transplant. There's also no risk of the body rejecting the transplant, and vision often improves more quickly. The success rate (graf survival) is 93-100% after one year.
Photorefractive keratectomy
This keratoconus laser surgery can be used alongside corneal cross-linking to correct any remaining vision problems. It's unsuitable for all patients, particularly those with a very thin cornea. Due to the study, 7 out of 10 people who get PRK surgery can see as well as someone with 20/20 vision a year after the procedure, even without glasses or contacts. Additionally, more than 92% of these patients can see at least as well as someone with 20/40 vision, again without needing glasses or contacts.
An artificial cornea transplant
It is an operation where doctors replace a damaged cornea with an artificial one, also known as keratoprosthesis. It's often used when a regular cornea transplant doesn't work for the patient. Many studies looking at middle-term outcomes show good results. More than 80% of patients keep seeing well after treatment. Also, most patients, or over 70%, can see clearly, with at least 20/200 or better vision.
Types of manufactured corneas
- Boston keratoprosthesis: This is the most common type. It has a clear plastic front and back with a donor cornea. This type is used for people whose own corneas are very cloudy. The success rate for keratoconus disease treated by Boston keratoprosthesis is over 80%, even after previous graft failure.
- AlphaCor: This is a one-piece device made from flexible plastic. It allows light to pass through and improves vision. It's used when patients have rejected many donor corneas or a regular transplant wouldn't work.
Artificial cornea transplants can significantly help people who can't see better than regular ones. But like all operations, there are risks, so discussing these with the doctor is essential, even if it seems the best keratoconus treatment in the world.
Leading keratoconus specialists
 Some keratoconus statistics
Some keratoconus statistics
Keratoconus disease often starts in people aged 10 to 25. It worsens until around 40 and usually doesn't worsen after that point.
A thorough analysis of keratoconus was published in the journal Contact Lens & Anterior Eye. The study confirmed that the chosen treatment depends heavily on the disease's severity and progression. Usually, glasses are used for mild cases, contact lenses for moderate conditions, and corneal surgery for severe cases. 87% of patients are treated with contact lenses.
Keratoconus is the primary reason for corneal transplant and implant procedures, accounting for 58% of these surgeries. However, patients can maintain good visual function with early detection and timely surgical intervention. The success rates for some methods reach 100%.
The success rate of cornea transplant
Approximately 12-20% of individuals with keratoconus disease might need a corneal transplant.
Corneal transplants can be either full-thickness, known as penetrating keratoplasty, or partial-thickness, called lamellar keratoplasty. Corneal transplants are the most frequently performed transplant surgeries today. They have an impressive success rate, with over 90% being successful after one year and 74% remaining successful after five years.
Due to another study, the results of corneal graft procedures were evaluated using an extensive database consisting of 4,499 entries. The survival rate of penetrating corneal grafts was 91%after one year, decreasing to 72% at the five-year mark and 69% after seven years.
Like any surgery, a cornea transplant for keratoconus disease comes with potential risks. These might include the body not accepting the new cornea, infections, or continued problems with vision. However, most cornea transplants are successful and are usually problem-free for at least a decade.
But, even after the operation, many patients still need glasses or contacts. The strength required depends on how severe the eye shape problem is.
What is keratoconus prognosis?
Keratoconus gets worse over time but rarely causes blindness. At the same time, even when it stops, it can still cause some issues.
Pediatric keratoconus tends to be more severe than in adults. This difference is often attributed to variations in corneal structure between these two age groups.
If it is left untreated, it can cause severe vision problems. In some cases, it can cause scars on the cornea, making vision even worse and making it hard to wear contact lenses. In simpler terms, keratoconus isn't a disability by itself. However, the significant vision loss it can cause might be considered a disability.
Combining keratoconus and driving can be challenging, especially if the disease has progressed significantly. The symptoms can make it difficult to see, especially at night or in bright sunlight, affecting driving ability.
People with keratoconus need to correct their vision for safe driving. It's essential for individuals with keratoconus to regularly visit their eye care provider to monitor the progress of the disease and adjust their vision correction as necessary.
AiroMedical works hand-in-hand with top eye doctors worldwide to help people with keratoconus. Most patients can return to their daily lives with the correct diagnosis and treatment. Choose AiroMedical for a clear path to better vision.
References:
- Arnalich-Montiel, F., Alió del Barrio, J. L., & Alió, J. L. (2016). Corneal surgery in keratoconus: which type, which technique, which outcomes? Eye and Vision, 3, Article 2.
- Lim, L., & Lim, E. W. L. (2020). Current perspectives in the management of keratoconus with contact lenses. Eye (London, England), 34(12), 2175–2196. https://doi.org/10.1038/s41433-020-1065-z. PMCID: PMC7784906, PMID: 32641797.
- Williams, K. A., Muehlberg, S. M., Lewis, R. F., & Coster, D. J. (1995). How successful is corneal transplantation? A report from the Australian Corneal Graft Register. Eye, 9, 219-227. doi 10.1038/eye.1995.43
- Motlagh MN, Moshirfar M, Murri MS, Skanchy DF, Momeni-Moghaddam H, Ronquillo YC, Hoopes PC. Pentacam® Corneal Tomography for Screening of Refractive Surgery Candidates: A Review of the Literature, Part I. Med Hypothesis Discov Innov Ophthalmol. 2019;8(3):177-203. PMCID: PMC6778463. PMID: 31598520.
- Masiwa, L. E., & Moodley, V. (2020). A review of corneal imaging methods for the early diagnosis of pre-clinical keratoconus. Journal of Optometry, 13(4), 269–275. https://doi.org/10.1016/j.optom.2019.11.001. PMCID: PMC7520528, PMID: 31917136

















