Regional Chemotherapy Has Positive Effects in the Treatment of Pancreatic Cancer
Because pancreatic disease is often discovered too late, pancreatic cancer is among the oncological diseases with the worst prognosis. The Medias Clinic has developed an innovative treatment method that can dramatically improve the quality of life for those affected.
The best chance of curing pancreatic cancer is through surgical removal of the malignant tumor mass. If this is not possible, for example, because the cancer is discovered too late or is growing in a location that is difficult to access surgically, systemic chemotherapy is usually used as the current standard therapy, but this is often accompanied by significant side effects.
New Aherapeutic Approaches with Local Effects
Current clinical research is therefore focused on new therapeutic approaches that act directly on the tumor and metastases, thereby causing fewer systemic side effects. Interventional oncology encompasses treatment techniques that reach the tumor either via the arterial blood supply or via probes. In both cases, the procedure is usually minimally invasive.
Electroporation Makes Tumor Cells Permeable
Electroporation, in which probes generate an electrical voltage within tumor tissue, is showing promising initial results. This voltage makes the tumor's cell membranes more permeable. Irreversible electroporation permanently disrupts cell membranes, leading to tumor cell death.
Electrochemotherapy involves temporarily creating pores in cell membranes. This allows chemotherapy to penetrate the cell and exert its effects on the tumor. A major advantage is that with improved chemotherapy efficacy, the dosage can be significantly reduced, thereby also minimizing side effects.
Developed at Medias Clinic: Isolated Perfusion
If the pancreatic carcinoma grows in a location dangerously close to blood vessels or other sensitive anatomical structures that are difficult to reach even with probes, electroporation is often not possible. In these cases, the Medias Clinic has developed a specialized regional chemotherapy (RCT) called isolated perfusion. In this procedure, catheters are placed near the tumor via the blood vessels in the groin area, and undiluted cytostatic drugs are injected directly into the tumor, where they can act immediately.
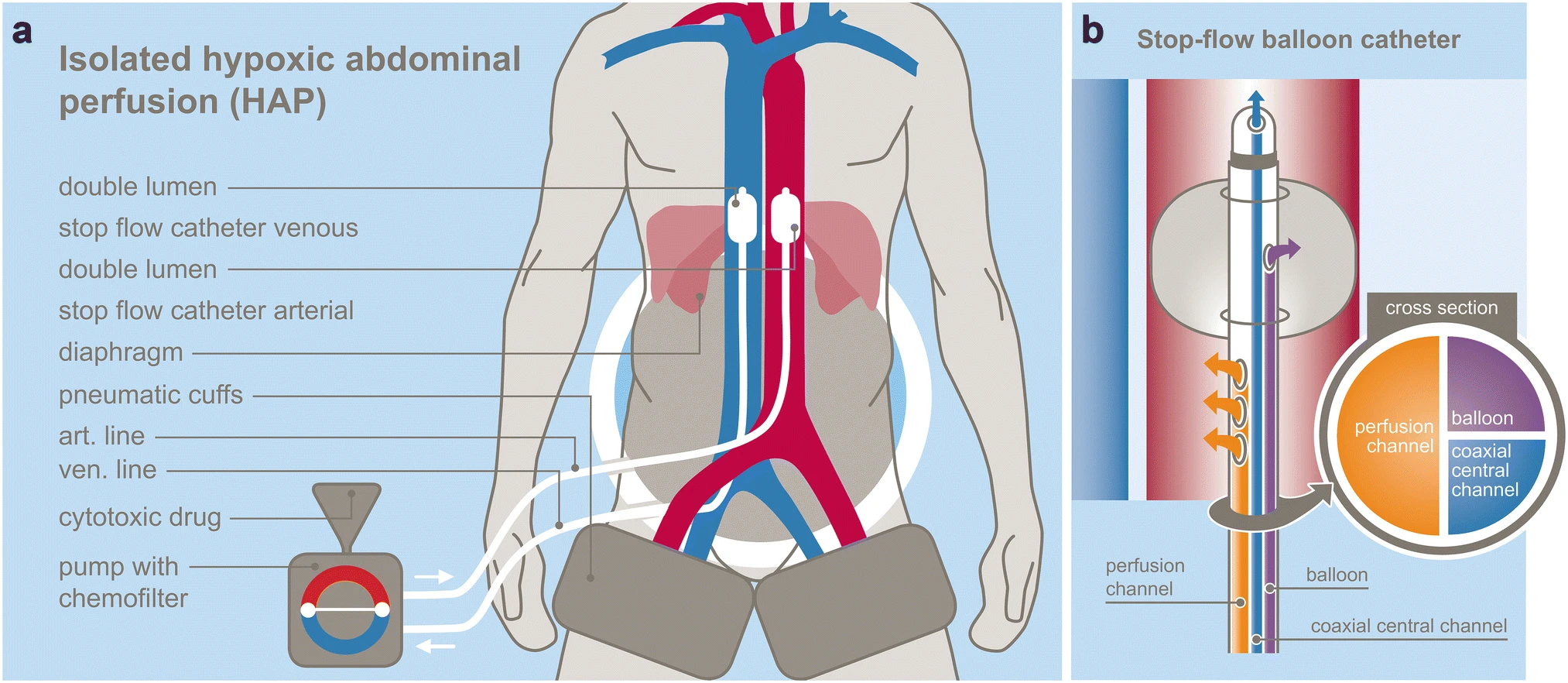
This procedure can also use balloon catheters to temporarily isolate the tumor from the rest of the bloodstream. This allows the cytostatic drugs to penetrate the malignant tissue particularly effectively.
The reduced treatment volume achieved with balloon catheters enables significantly higher drug concentrations to be reached with a low dose than would be possible with systemic chemotherapy.
In a 2019 observational study conducted at the Medias Clinic under the direction of Professor Karl R. Aigner, the impact of regional chemotherapy on pancreatic cancer was investigated with regard to survival time, tumor response, and quality of life. The results suggest that the perennial dilemma of chemotherapy, finding the right balance between efficacy and side effects, can be resolved by isolated perfusion.
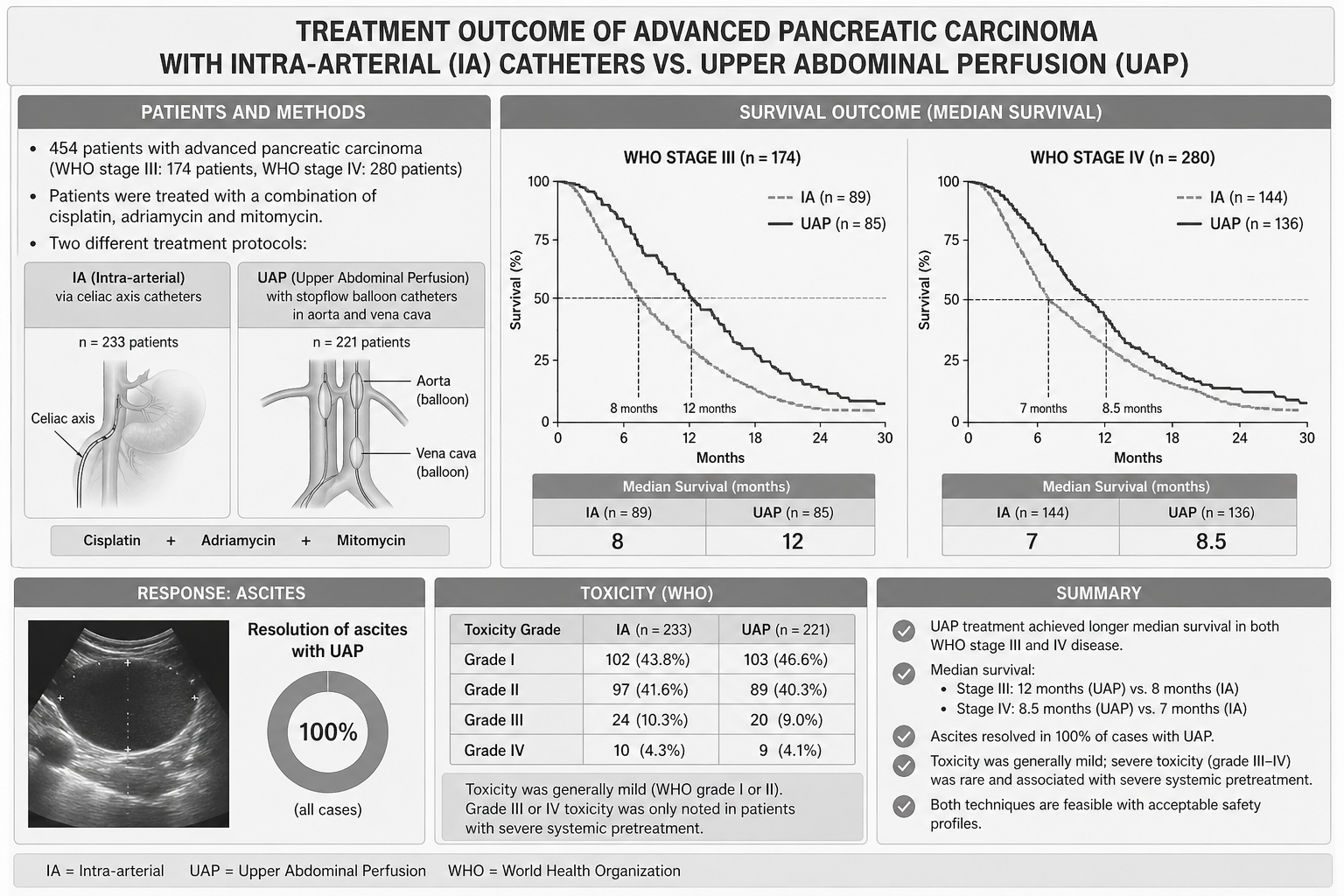
Observational study with 454 patients, published in the International Journal of Cancer Research and Clinical Oncology: Aigner KR, Gailhofer S, Selak E, Aigner K. Intra-arterial infusion chemotherapy versus isolated upper abdominal perfusion for advanced pancreatic cancer: a retrospective cohort study on 454 patients. J Cancer Res Clin Oncol. 2019 Nov;145(11):2855-2862. doi: 10.1007/s00432-019-03019-6. Epub 2019 Sep 10. PMID: 31506738; PMCID: PMC6800855
