Our Interventional Experience Results: 12 Years in Managing Inoperable Pancreatic Cancer
Being diagnosed with pancreatic cancer that cannot be removed surgically (what we call inoperable or unresectable) is deeply challenging. For many years, treatment options were limited mainly to chemotherapy, often with modest results. Over the past decade, however, we at Interventional Radiology Institute of University Hospital Frankfurt in Germany have explored additional approaches, especially minimally invasive, image-guided treatments, to help control the disease and improve quality of life.
These approaches do not replace standard therapies like chemotherapy, but they open an additional trail, allowing us to directly target tumors in ways previously not possible. Our recently published clinical experience reflects what we have observed in everyday practice, not just under ideal research conditions, but in real patients with complex medical situations.
The Methods We Used
Pancreatic cancer is particularly challenging because it is often diagnosed late. By the time symptoms appear, the tumor may already involve critical blood vessels or have spread beyond the pancreas. In such cases, surgery (the only potentially curative option) is no longer possible. This is where interventional treatments begin to play an important role.
One of the techniques we frequently use is transarterial chemoembolization (TACE). In simple terms, this involves navigating a very fine catheter through the blood vessels directly to the tumor. Chemotherapy is delivered precisely where it is needed, and the tumor’s blood supply is partially blocked at the same time. This dual effect allows us to concentrate treatment locally while reducing the impact on the rest of the body.
Another method we employ is microwave ablation (MWA). Using imaging guidance, we place a thin probe into the tumor and apply controlled heat to destroy cancer cells. Patients often find it reassuring to understand that this is not open surgery, but a targeted procedure performed through the skin with careful precision.
Results We Received
Over the years, we began combining these two approaches in selected patients. What we observed was encouraging. While no treatment could fully eliminate the disease in these advanced cases, we saw that tumors could often be controlled more effectively when therapies were combined. In some patients, tumor growth slowed significantly, and in others, the disease remained stable for prolonged periods.
Summarizing 150 patients with unresectable locally advanced pancreatic cancer treated between 2010 and 2023, we observe the following results. Group A: Combination therapy of TACE and MWA. Group B: Monotherapy with TACE.

The results showed a clear difference between the groups. In Group A, nearly 70% of patients were alive 1 year after treatment, with a median survival of about 14.6 months. In Group B, about 44% of patients were alive at one year, with a median survival of around 9 months. This means that patients in Group A generally survived longer and had better overall outcomes compared with those in Group B.
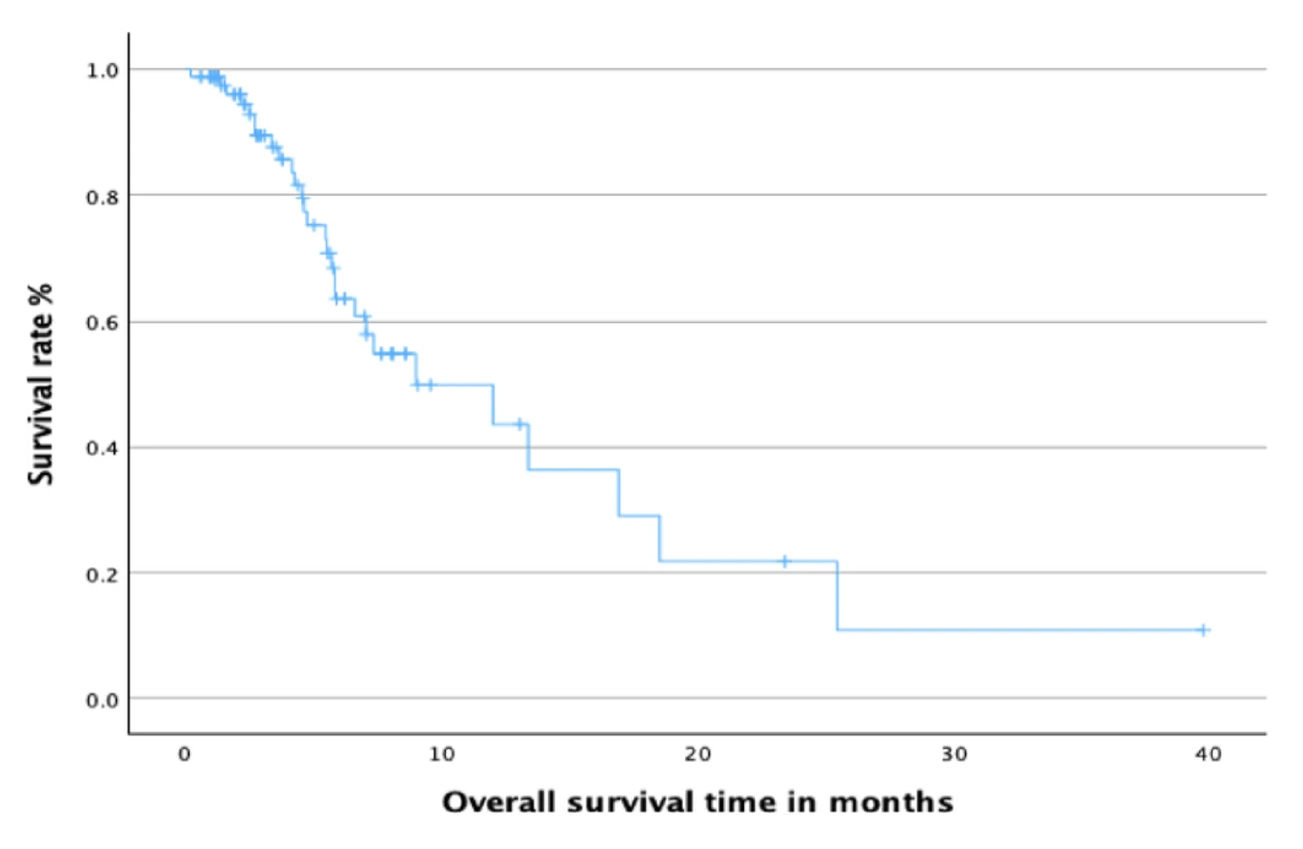
Overall, the findings suggest that the treatment strategy used in Group A may provide a meaningful survival advantage for patients with advanced pancreatic cancer who cannot undergo surgery.
Procedure-Related Safety
Equally important is the question of safety. Patients understandably worry about undergoing additional procedures when they are already dealing with a serious illness. In our experience, both TACE and microwave ablation have been well tolerated. Complications were relatively uncommon, and most patients recovered quickly, often with shorter hospital stays than those required by traditional surgical approaches.
Conclusion Statement
Looking ahead, I believe the future lies in combining therapies more intelligently and tailoring them more precisely. Advances in imaging, technology, and systemic treatments will likely further enhance the role of interventional oncology. What once seemed experimental is gradually becoming an established part of comprehensive cancer care.
For patients and their families, the most important message I can offer is this: even when surgery is not an option, there are still meaningful treatments available. Medicine continues to evolve, and with it, new opportunities to manage disease and preserve quality of life.
Further information on the study can be found here: Vogl, T.J.; Cojocaru, R.; Dahm, D.M.; Adwan, H. Interventional management of unresectable pancreatic cancer using transarterial chemoembolization and microwave ablation: a single-center evaluation over 12 years. J. Cancer Res. Clin. Oncol. 2026, 152, 78. doi: 10.1007/s00432-026-06463-3.