Percutaneous Vertebroplasty / Osteoplasty - Spine Cement in Osteoporosis, Malignant Bone Tumors & Fractures at University Hospital Frankfurt
Frankfurt am Main, Germany
Overview
Age group
Kids, Adults
Type of care
Outpatient
Method
Microinvasive
About the offer
What’s included
Medical service
Examination
- clinical history-taking
- medical records review
- physical examination
- consultation with an interventional radiologist
Laboratory tests
- complete blood count (CBC)
- blood type test (ABO, Rh)
- biochemical analysis of blood (kidney and liver function tests, electrolytes)
- coagulation/INR/PTT
Diagnosis
- MRI or CT to assess fracture age and morphology
Treatment
- preoperative patient preparation
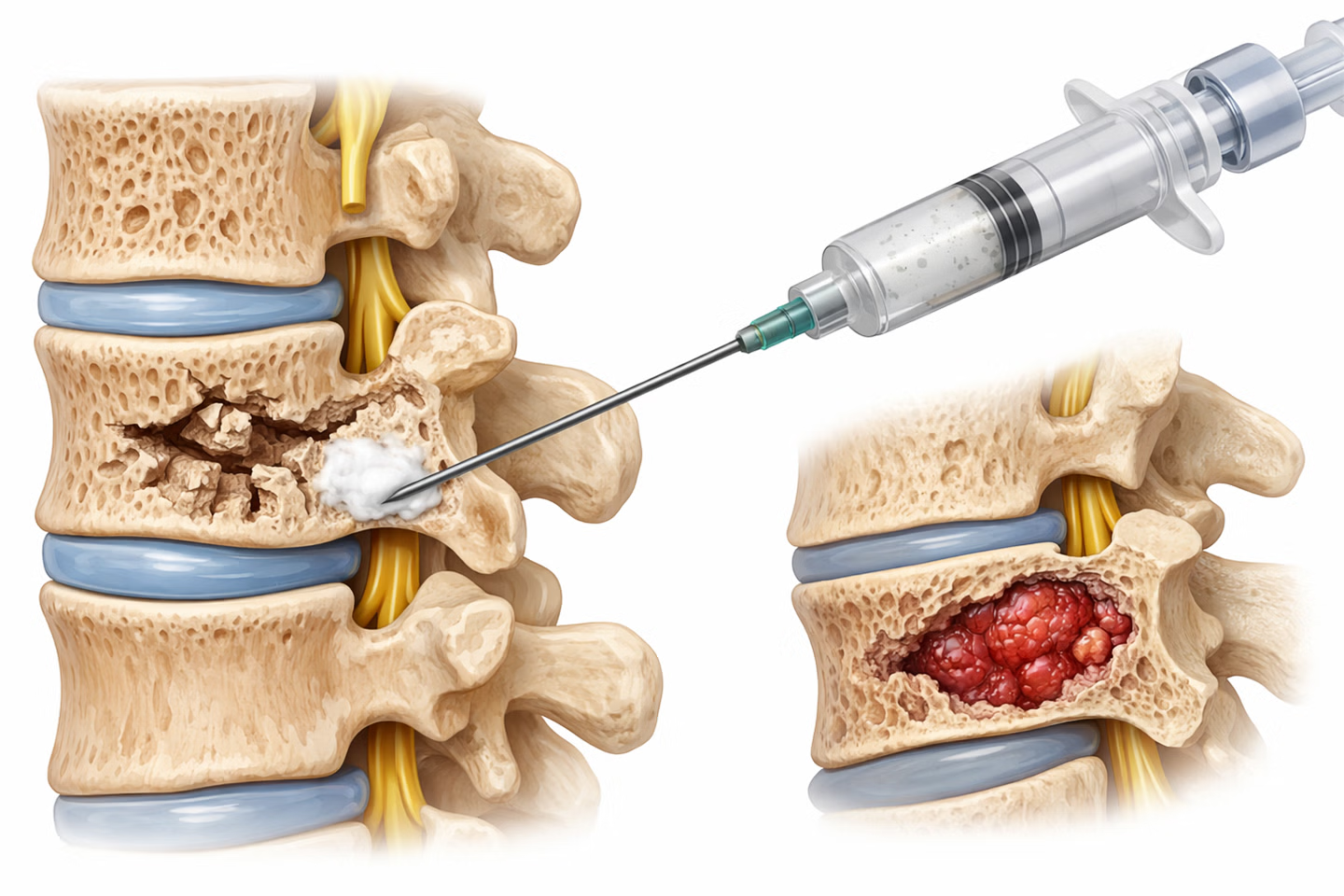
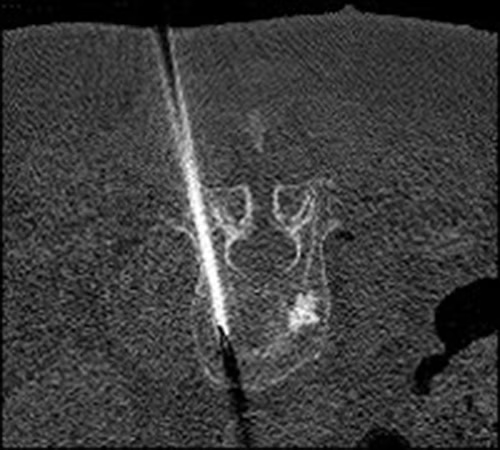
- percutaneous vertebroplasty/osteoplasty procedure with application of medical-grade bone cement (Polymethyl methacrylate - PMMA)
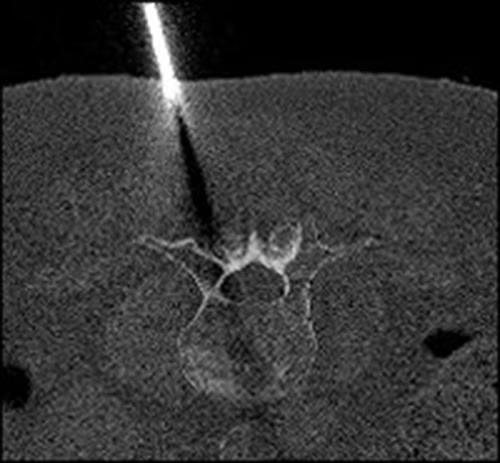
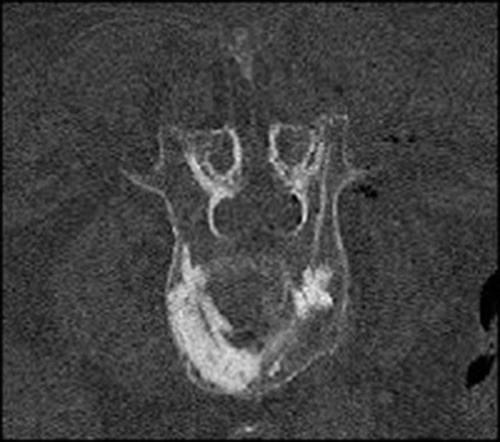
- high-resolution 3D imaging guidance (Siemens ARTIS icono or CT-fluoroscopy)
- postoperative care with pain level evaluation (Visual Analog Scale - VAS)
- symptomatic treatment
Other
- doctor's fee
- cost of essential medicines
- cost of essential materials
- deep sedation/general anesthesia
- nursing service
- discharge medical records
- further recommendations
Extra add-ons
Airport transfer
Personal coordinator
HealthDocs translate
Visa Support
Telemedicine
AiroCare
AiroMedical support
Payment protection
Patient advocacy
Price match
Meet the provider
interventional radiology, interventional oncology, chemoembolization (TACE) & chemoperfusion (TACP)
9.90
Gallery
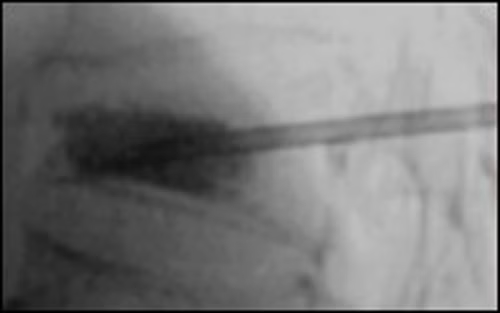
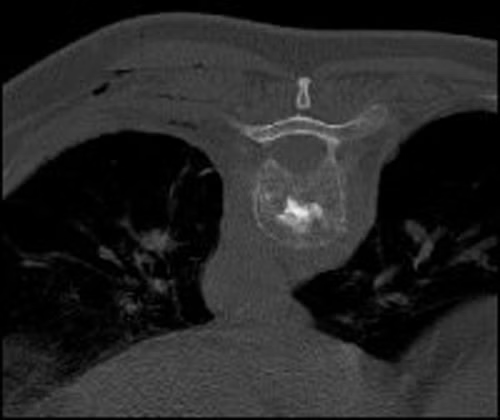
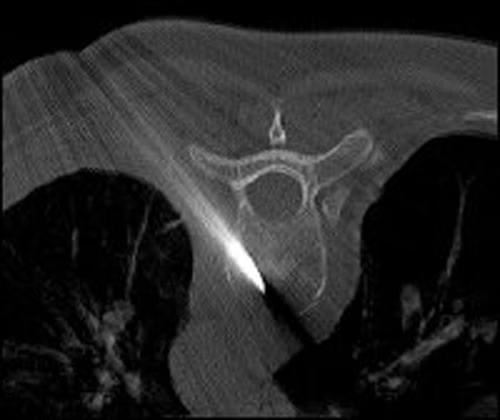
Customize this offer
If you're not seeing exactly what you need here, send your custom request. You can discuss the content, specifics, price & timeline to create a personalized plan.
Location
Theodor-Stern-Kai 7, 60596 Frankfurt am Main, Germany
FAQ
What is the rating of the offer?
Percutaneous Vertebroplasty / Osteoplasty - Spine Cement in Osteoporosis, Malignant Bone Tumors & Fractures at University Hospital Frankfurt is rated as 9.90 by AiroMedical.
Who is offering a deal?
The provider is Prof. Dr. med. Thomas Vogl.
How long does the offer take?
The offer is designed for 4 days.
Individual cost estimate. Non-binding 100% free assessment.
HomeOffersPercutaneous Vertebroplasty / Osteoplasty - Spine Cement in Osteoporosis, Malignant Bone Tumors & Fractures at University Hospital Frankfurt