Motor neuron disease guide
 What is motor neuron disease?
What is motor neuron disease?
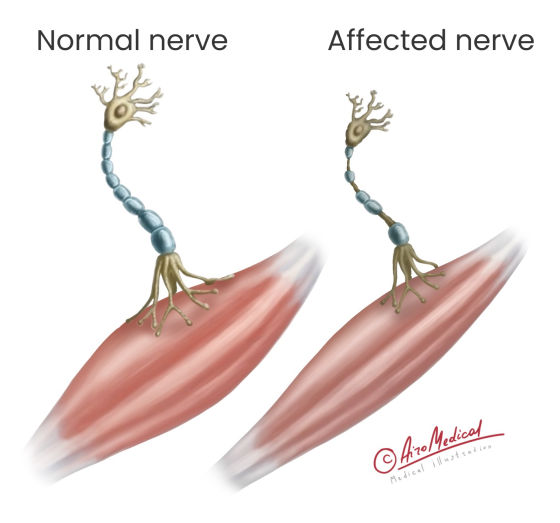 Motor neurons are a specific type of nerve cell. Their job is to send information throughout the body so it can move. There are two types of neurons: the upper ones are located in the brain and transmit information to the spinal cord, and the lower ones act in the opposite direction (data from the spinal cord goes to the brain).
Motor neurons are a specific type of nerve cell. Their job is to send information throughout the body so it can move. There are two types of neurons: the upper ones are located in the brain and transmit information to the spinal cord, and the lower ones act in the opposite direction (data from the spinal cord goes to the brain).
Like other parts of the human body, motor neurons can become damaged. In this case, motor neuron disease (MND) happens. MND is a rare disorder that affects the nerves and brain. It is a progressive condition when affected nerve cells degenerate and die.
MND can affect anyone, but most people over 40 are affected, with men slightly more than women. Approximately 2 out of 100,000 people develop motor neuron disease. Renowned English physicist Stephen Hawking lived with motor neuron disease for many decades until his death in March 2018. In some people (5-10%), MND is caused by hereditary mutations.
 Diagnostic tests
Diagnostic tests
Initial symptoms depend on the condition. However, the most common early symptom is weakness in the arms and legs. Often it is more pronounced on one side of the body. Other early signs of the condition include:
- muscle twitching and atrophy;
- stiffness and clumsiness in gait;
- general fatigue of the body;
- difficulty chewing, swallowing and speaking.
There are no specific tests for motor neurone disease, and diagnosing it can be challenging in the early stages. Diagnosis is based on medical history, neurological examination, and diagnostic tests. A referral to a neurologist is recommended if motor neuron disease is suspected. Standard tests used in the diagnostic process are:
- Blood and urine tests - can help rule out other conditions and detect any increase in creatine kinase, a substance that muscles produce when they break down.
- Brain MRI scan - helps rule out other conditions such as a stroke, brain tumour, or unusual brain structures.
- Electromyography (EMG) - measure the amount of electrical activity in the muscles.
- Nerve Conduction Study (NCS) - measures the rate electricity travels through the muscles.
- Spinal tap or lumbar puncture - the doctor takes a sample of the cerebrospinal fluid surrounding the brain and spinal cord. This test can help rule out other conditions.
- Muscle biopsy - helps to detect or rule out muscle disease.
After the indicated tests have been carried out, the medical team observes the patient for some time before diagnosing motor neuron disease.
 Treatment methods
Treatment methods
What is the danger of motor neuron disease? It is because the disease progresses, and the patient's condition worsens every day. Moving, swallowing, and breathing becomes more and more difficult. There comes a time when the patient cannot perform daily activities independently. And then, for example, a probe may be needed for feeding and a face mask for inhaling air. Then, of course, the patient needs constant outside help.
Nowadays, there is no cure for motor neuron disease. In current conditions, doctors are faced with the task of slowing down the progression of the disease and maximizing comfort, independence and self-sufficiency.
The choice of drugs depends on many factors, such as:
- form of motor neuron disease;
- type and severity of symptoms;
- personal needs and wishes of the patient;
- access to medicines and treatments.
Symptomatic treatment helps for the following:
- Slowing the progression of the disease - is achieved by drugs such as Edaravone (Radikava), Nusinersen (Spinraza) and Onasemnogen Abeparvovec (Zolgensma). For example, the drug Riluzole changes the activity of natural bodily substances that affect the muscles and nerves.
- Muscle spasms and stiffness - Botulinum Toxin (Botox) helps block signals from the brain to tense muscles for about three months. Baclofen (Lioresal), a muscle relaxant, may relieve muscle stiffness, spasms, and yawning.
- Pain relief - anti-inflammatory drugs may help with mild to moderate pain from muscle spasms
- Other signs - Scopolamine is a drug that can help with salivation and easily can be absorbed through a patch on the skin. Antidepressants can help with episodes of uncontrollable laughter or crying, which doctors call emotional lability.
- Assistive devices and treatments - over time, the patient may need special devices to help with movement, communication, swallowing and breathing. Some devices allow a person to stay independent longer, and others prolong life. For example, feeding tubes and ventilators can support vital functions.
Rehabilitation helps improve functional independence and, ultimately, quality of life. As a rule, it is carried out in specialized clinics. And the recovery process is as follows:
- Physiotherapy - procedures and exercises that help increase muscle strength, reduce muscle stiffness and spasms, reduce the risk of falls, etc.
- Occupational therapy - hand therapy using an exercise program and functional activities alone or in groups.
- Speech and language therapy - to teach family members and caregivers to communicate with patients with MND, assistance in written communication.
 New treatment options
New treatment options
Continuous research has given doctors a better understanding of the disease and its mechanisms, but there is still no effective cure. The challenge for scientists is to do much more to expand knowledge of the disease and the application of new methods:
- Stem cell therapy - uses the ability of stem cells to self-renew and is an attractive feature for treating motor neuron diseases.
- Gene therapy - is a new but promising strategy for treating motor neuron disease. Drugs developed based on gene modifications have shown excellent results in treating such a type of MND as spinal muscular atrophy - until 2017, a completely incurable disease.
In recent years, there has been an increase in research and an expansion in treating patients with motor neuron disease.
 Statistics and prognosis
Statistics and prognosis
The prospect is different for each type of motor neuron disease. Some types are milder and progress more slowly than others. Life expectancy for about half of people with the condition is three years from the onset of the symptoms. However, some people can live up to 10 years, and in rare cases, longer.
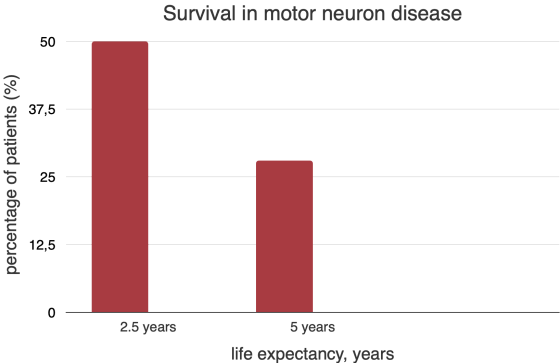
The Scottish Motor Neuron Disease Registry (SMNDR) is a promising collaborative population-based project that has collected data on diseased patients and their diagnosis and compared their prognosis with previous survival studies since 1989. The overall 50% survival from symptom onset was 2.5 years, and the 5-year survival was 28%.
Living with motor neuron disease is extremely difficult and often presents a horrifying picture before a diagnosis is made. However, with the support provided by AiroMedical in selecting specialized hospitals and specialists, many will be able to maintain independence for a significant part of their life.
References:
- American Association of Neuromuscular & Electrodiagnostic Medicine: Motor Neuron Disease
- National Library of Medicine: Diagnosis and management of motor neurone disease
- NHS : Motor neurone disease
- Healthline Media UK: What is motor neuron disease?
- WebMD: What Are Motor Neuron Diseases?
- healthdirect's information: Motor neurone disease (MND)
- MND Association: What is MND?
- Southern Cross: Motor neurone disease - symptoms, diagnosis, treatment
- Brain Research UK: Motor neurone disease
- Springer Nature Switzerland: The prognosis of adult-onset motor neuron disease: a prospective study based on the Scottish Motor Neuron Disease Register